Nephrology — MCQs

On this page
A 12-year-old child is diagnosed with systemic lupus erythematosus (SLE) and presents with nephrotic-range proteinuria. Renal biopsy reveals "wire loop lesions." Which of the following is the drug of choice in this case?
Which of the following is not a recognised cause of recurrent renal stone formation?
A 30-year-old hypertension patient presents with flank pain. CT abdomen was performed. All are true about the condition shown except?
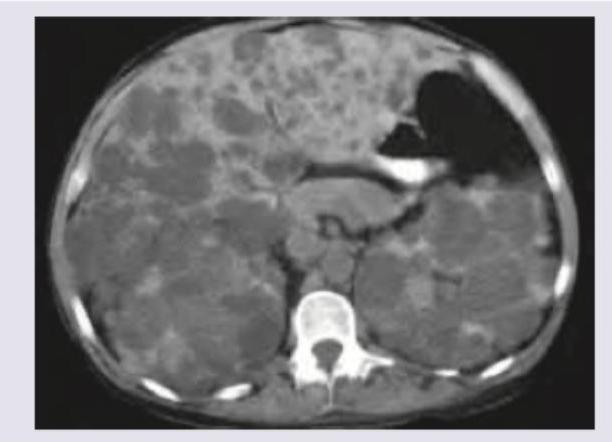
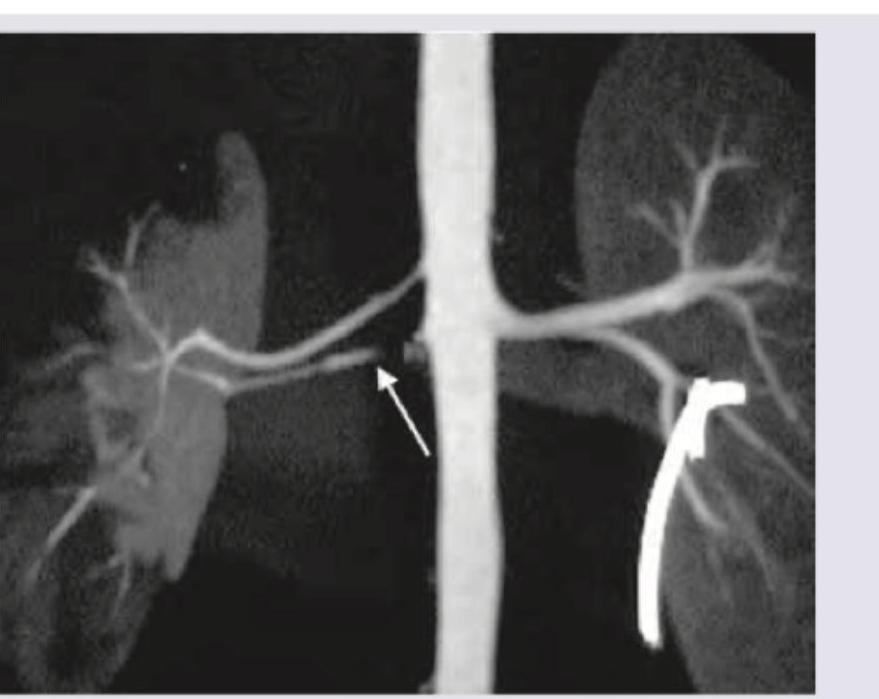
All are true about the condition shown in the above figure except:
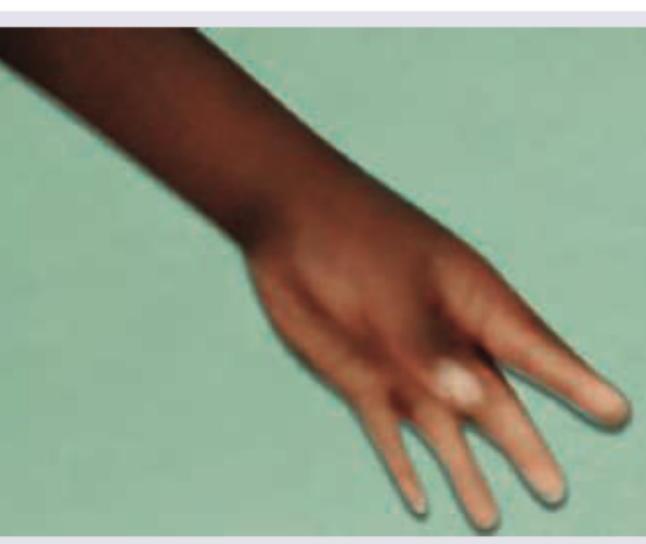
The hand of a patient of Gitelman syndrome shows?
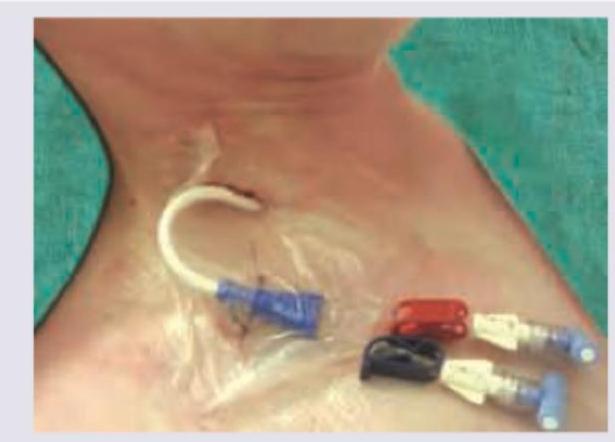
Hemodialysis is being performed on a patient of ESRD. Central dialysis catheter is placed at which site?
A patient of ESRD is scheduled for hemodialysis. He complains of palpitations. Which of the following findings are seen on ECG?
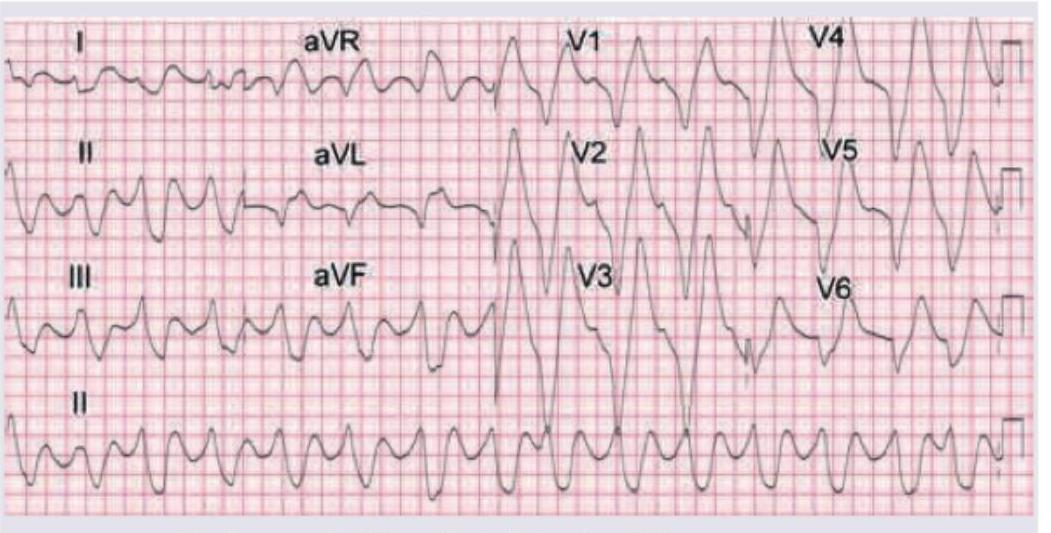
A 30-year-old lady with crush injury was admitted to the casualty. Her urobag shows 100 mL red color urine. ECG is shown below. All are indicated for this patient except?
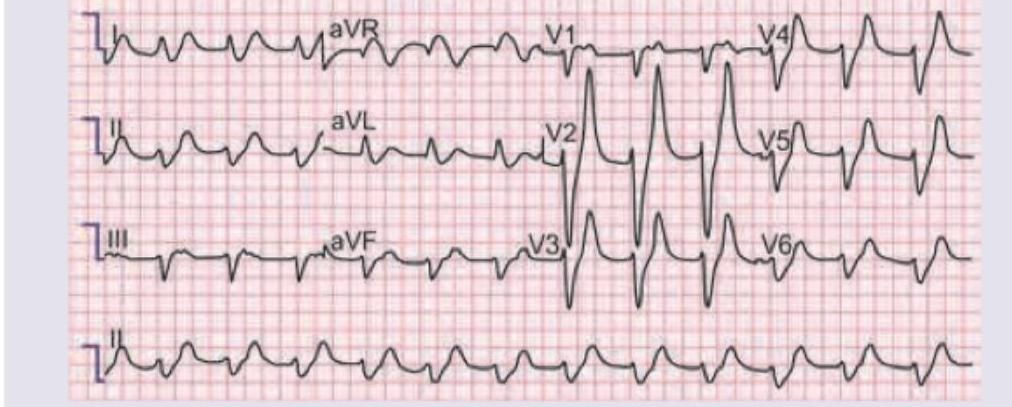
Which of the following findings in a patient are suggestive of acute nephritis? I. Hematuria II. Oliguria III. Reduced size of both kidneys IV. Edema Select the correct answer using the code given below :
Which one of the following hereditary tubulo-interstitial kidney diseases has an autosomal recessive mode of inheritance?
Practice by Chapter
Acute Kidney Injury
Practice Questions
Chronic Kidney Disease
Practice Questions
Glomerular Diseases
Practice Questions
Tubulointerstitial Diseases
Practice Questions
Nephrotic and Nephritic Syndromes
Practice Questions
Urinary Tract Infections
Practice Questions
Renal Replacement Therapy
Practice Questions
Fluid and Electrolyte Disorders
Practice Questions
Acid-Base Disorders
Practice Questions
Kidney in Systemic Diseases
Practice Questions
Kidney Stones and Obstructive Uropathy
Practice Questions
Hypertension in Kidney Disease
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
