Nephrology — MCQs

On this page
Which of the following is not seen in Alport syndrome?
Chinese herb nephropathy is caused by which of the following?
Which of the following conditions is characterized by the shown urine microscopy finding?
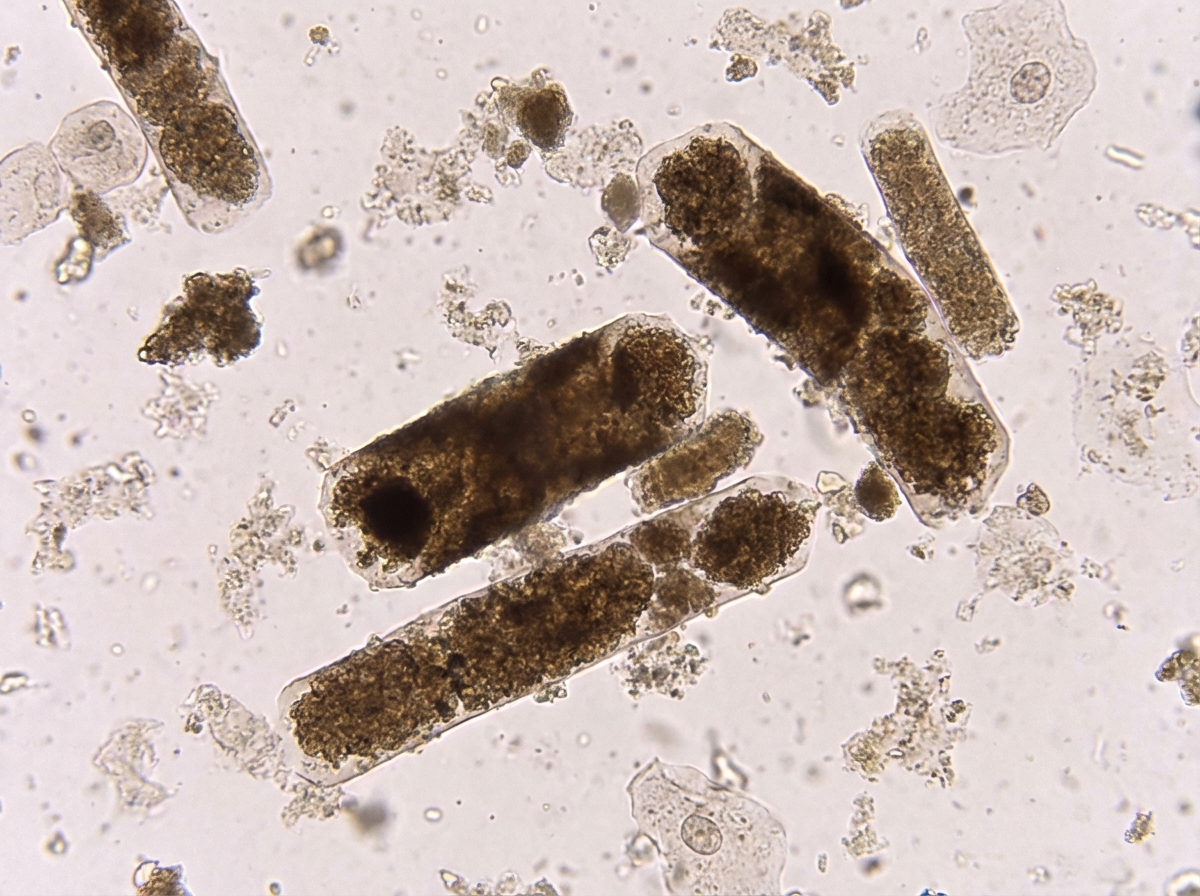
Chyluria is associated with the passage of urine which is:
Uremia is not associated with hypertension in which of the following situations?
All are features of HIV-associated nephropathy, EXCEPT:
A 28-year-old male sustained a severe crush injury in an accident. Which of the following complications is he most likely to develop?
Which of the following statements regarding analgesic nephropathy is true?
Most unlikely cause of acute tubular necrosis amongst the following is:
Hematuria with dysmorphic RBCs is a feature of which one of the following?
Practice by Chapter
Acute Kidney Injury
Practice Questions
Chronic Kidney Disease
Practice Questions
Glomerular Diseases
Practice Questions
Tubulointerstitial Diseases
Practice Questions
Nephrotic and Nephritic Syndromes
Practice Questions
Urinary Tract Infections
Practice Questions
Renal Replacement Therapy
Practice Questions
Fluid and Electrolyte Disorders
Practice Questions
Acid-Base Disorders
Practice Questions
Kidney in Systemic Diseases
Practice Questions
Kidney Stones and Obstructive Uropathy
Practice Questions
Hypertension in Kidney Disease
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
