Nephrology — MCQs

On this page
A 70-year-old man presents with right flank pain that radiates to his groin. He has a long history of heavy smoking and alcohol use and reports passing a kidney stone approximately 20 years prior to this event. His past medical history is also remarkable for diabetes mellitus, high cholesterol, and obesity. A computed tomography scan reveals a right 7-mm ureteral stone. In addition, coronal imaging was obtained. Which of the following is the greatest risk factor for the development of additional findings on the imaging study?
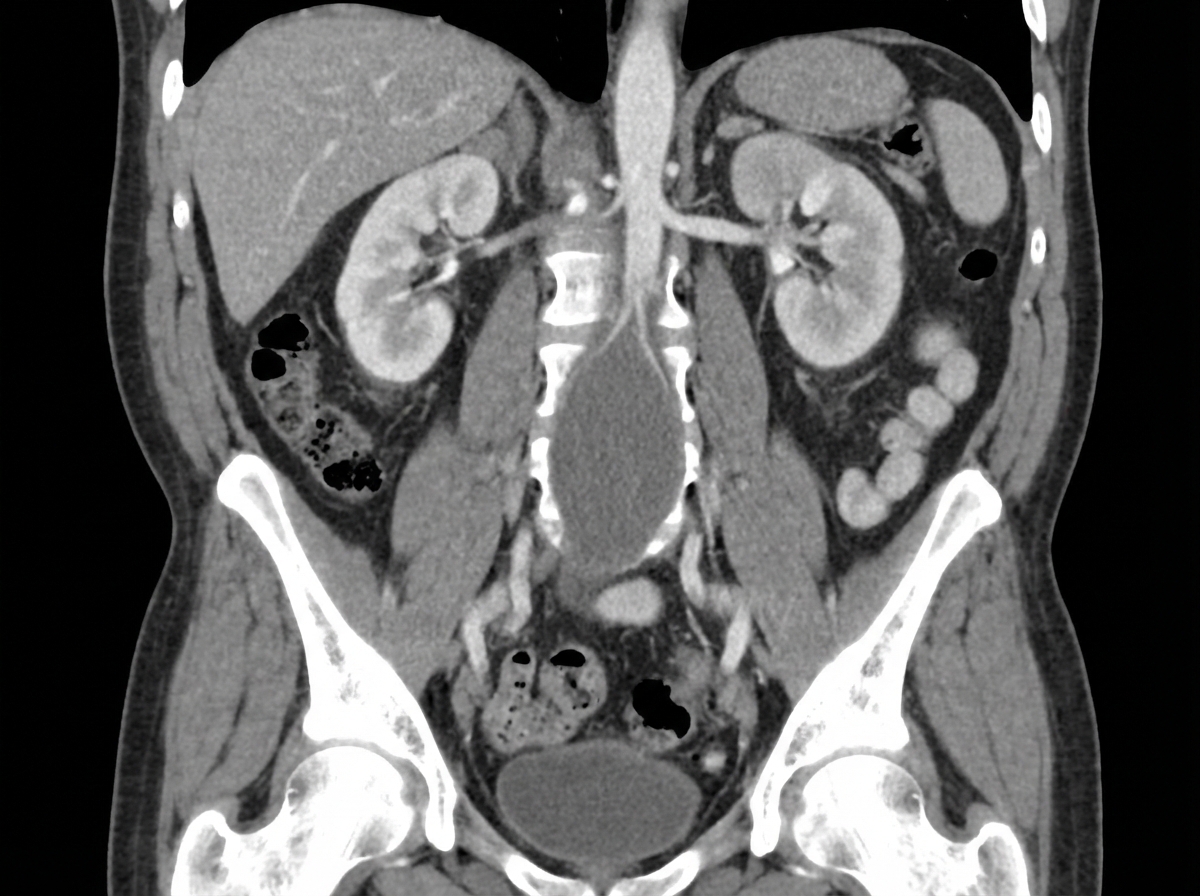
What is the most common cause of death in patients undergoing dialysis for acute renal failure?
A patient with acute urinary tract infection (UTI) usually presents with:
Chronic kidney disease is defined as GFR less than (mL/ min/ 1.73 m2):
Which of the following drugs is NOT used for the treatment of acute hyperkalemia?
Mutation in the PKHD1 gene causing autosomal recessive polycystic kidney disease (ARPKD) maps to which chromosome?
Which of the following conditions causes normal anion gap metabolic acidosis?
All are measures taken to address hyperkalemia in acute kidney injury, except?
In Dent's disease, which of the following is seen on laboratory evaluation?
What is a characteristic feature of glomerular hematuria?
Practice by Chapter
Acute Kidney Injury
Practice Questions
Chronic Kidney Disease
Practice Questions
Glomerular Diseases
Practice Questions
Tubulointerstitial Diseases
Practice Questions
Nephrotic and Nephritic Syndromes
Practice Questions
Urinary Tract Infections
Practice Questions
Renal Replacement Therapy
Practice Questions
Fluid and Electrolyte Disorders
Practice Questions
Acid-Base Disorders
Practice Questions
Kidney in Systemic Diseases
Practice Questions
Kidney Stones and Obstructive Uropathy
Practice Questions
Hypertension in Kidney Disease
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
