General Medicine — MCQs

On this page
Which of the following conditions is not associated with clubbing?
In a patient with a smoking history, which factor is most important to assess?
The 'C' wave in the JVP waveform is caused by which of the following events?
Hepatosplenomegaly is not seen in which of the following conditions?
20 mEq (mmol) of potassium chloride in 500 ml of 5% dextrose solution is given intravenously to treat which of the following conditions?
Which of the following conditions is associated with an increase in Lactate Dehydrogenase (LDH) levels?
Which of the following statements regarding obesity is true?
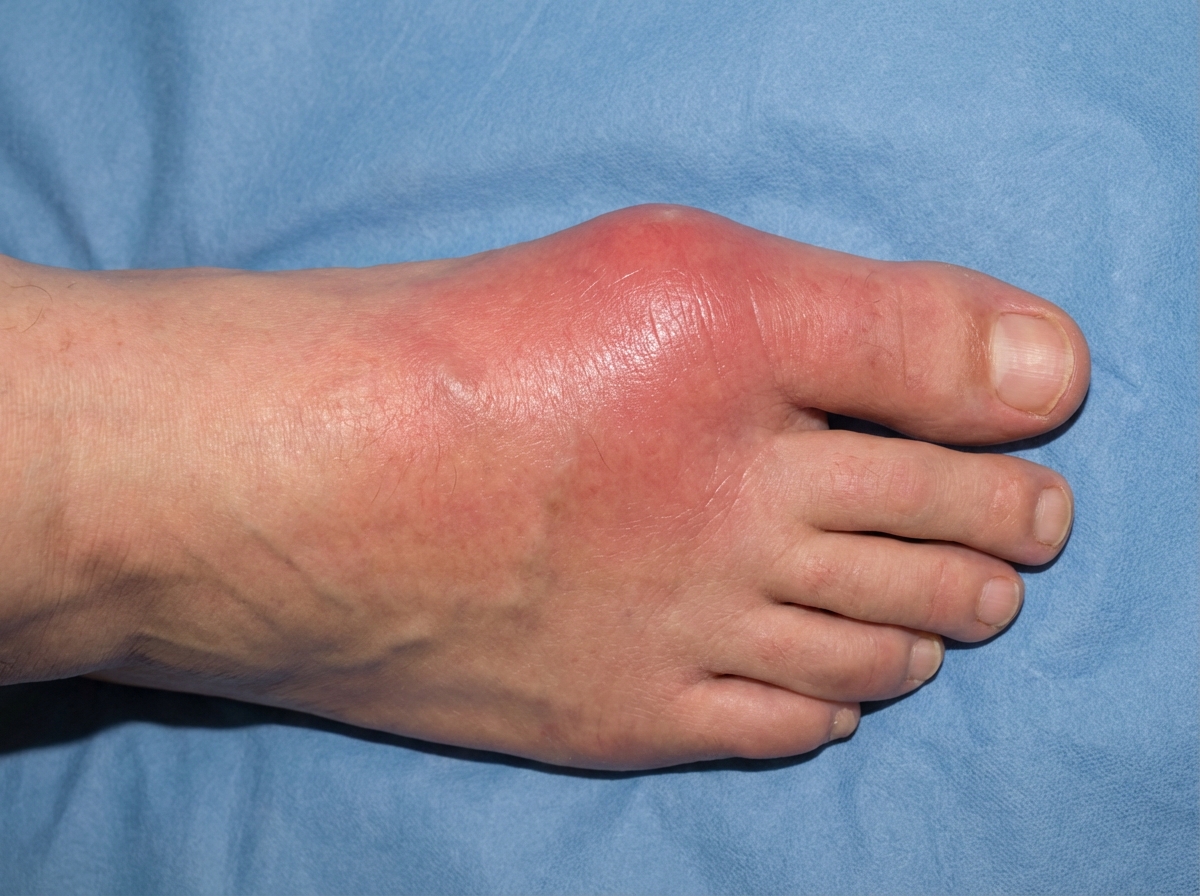
A 35-year-old man presents with acute onset of pain, swelling, and redness of his right big toe as shown in the image. What is the most likely diagnosis?
The second heart sound (S2) is best appreciated in which of the following areas?
Which of the following is not associated with zinc deficiency?
Practice by Chapter
Approach to the Medical Patient
Practice Questions
Differential Diagnosis Development
Practice Questions
Rational Diagnostic Testing
Practice Questions
Medical Decision Making
Practice Questions
Cost-effective Care
Practice Questions
Patient-centered Communication
Practice Questions
Interprofessional Collaboration
Practice Questions
Systems-based Practice
Practice Questions
High-value Care
Practice Questions
Transitions of Care
Practice Questions
Chronic Disease Management
Practice Questions
Medical Uncertainty Management
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
