General Medicine — MCQs

On this page
A 60-year-old male with a history of diabetes and hypertension is found unconscious. On examination, his pulse rate is 120/min and BP is 160/100 mm Hg. What is the next step in management?
Obesity is associated with decreased risk of:
Which is the first center activated before skilled voluntary movements?
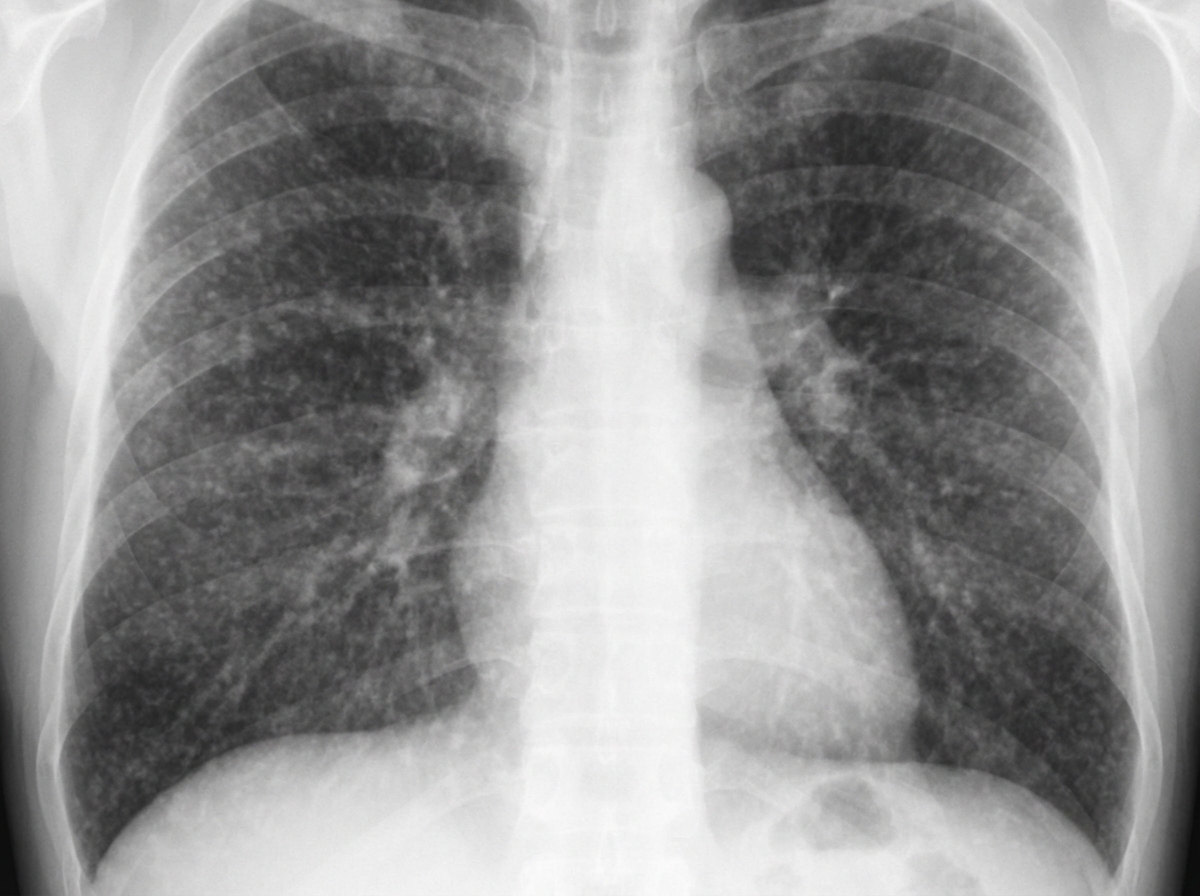
A 71-year-old man presents with low-grade fever, generalized malaise, and a feeling of being run-down. He has experienced weight loss and exhibits stigmata of chronic illness. There is no history of occupational exposure. On physical examination, vital signs are: pulse 110 bpm; temperature 99°F; respirations 19/min; blood pressure 90/60 mm Hg. The patient is frail and appears cachectic with temporal wasting. Other aspects of his physical exam are unremarkable. Laboratory data: Hb 10 g/dL; Hct 30%; MCV 90 fL; WBCs 3000/uL; differential normal; BUN 19 mg/dL; creatinine 1.0 mg/dL; sodium 129 mEq/L; potassium 5.0 mEq/L; ABGs (RA): pH 7.42, PCO2 35 mm Hg, PO2 58 mm Hg. Spirometry: FVC 60% of predicted; FEV1 60% of predicted. PPD skin test is negative (0 mm); induced sputum for AFB smear is negative. Chest radiograph is shown. What is the most likely diagnosis?
Which is the function of the tube mentioned below?
Which of the following statements about hemoptysis is false?
Which of the following is NOT true about chronic fatigue syndrome?
What is the temperature range considered hyperpyrexia?
Internal jugular vein pressure directly reflects the pressure of which cardiac chamber?
What is the investigation of choice for interstitial lung disease?
Practice by Chapter
Approach to the Medical Patient
Practice Questions
Differential Diagnosis Development
Practice Questions
Rational Diagnostic Testing
Practice Questions
Medical Decision Making
Practice Questions
Cost-effective Care
Practice Questions
Patient-centered Communication
Practice Questions
Interprofessional Collaboration
Practice Questions
Systems-based Practice
Practice Questions
High-value Care
Practice Questions
Transitions of Care
Practice Questions
Chronic Disease Management
Practice Questions
Medical Uncertainty Management
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
