Endocrinology — MCQs

On this page
A smoker presented with altered sensorium. His blood osmolality was found to be 240 mOsm/kg, urine osmolality 340 mOsm/kg, and serum Na+ is 122 mEq/L. What is the most likely diagnosis?
Which vaccine can be given to an individual with chronic diabetes mellitus?
Which of the following statements regarding Wolfram syndrome is FALSE?
What is used for long-term glycemic control in Diabetes Mellitus?
Hypothyroidism is seen in which of the following conditions?
Tetany may be a feature of the following conditions except?
If both parents have type 2 diabetes, what is the approximate risk of inheritance for their offspring?
A 33-year-old woman presents with gradually increasing coarse hair on her upper lip, chin, and lower abdomen for the past 3 years. She has mild facial acne but denies frontal balding or deepening of voice. Her menses are irregular, occurring every 28 to 60 days. Her BMI is 29.0 and her waist circumference is 36 inches. There is mild acanthosis nigricans of the axillae. Pelvic examination is normal without ovarian mass or clitoromegaly. What evaluation is indicated for her hirsutism?
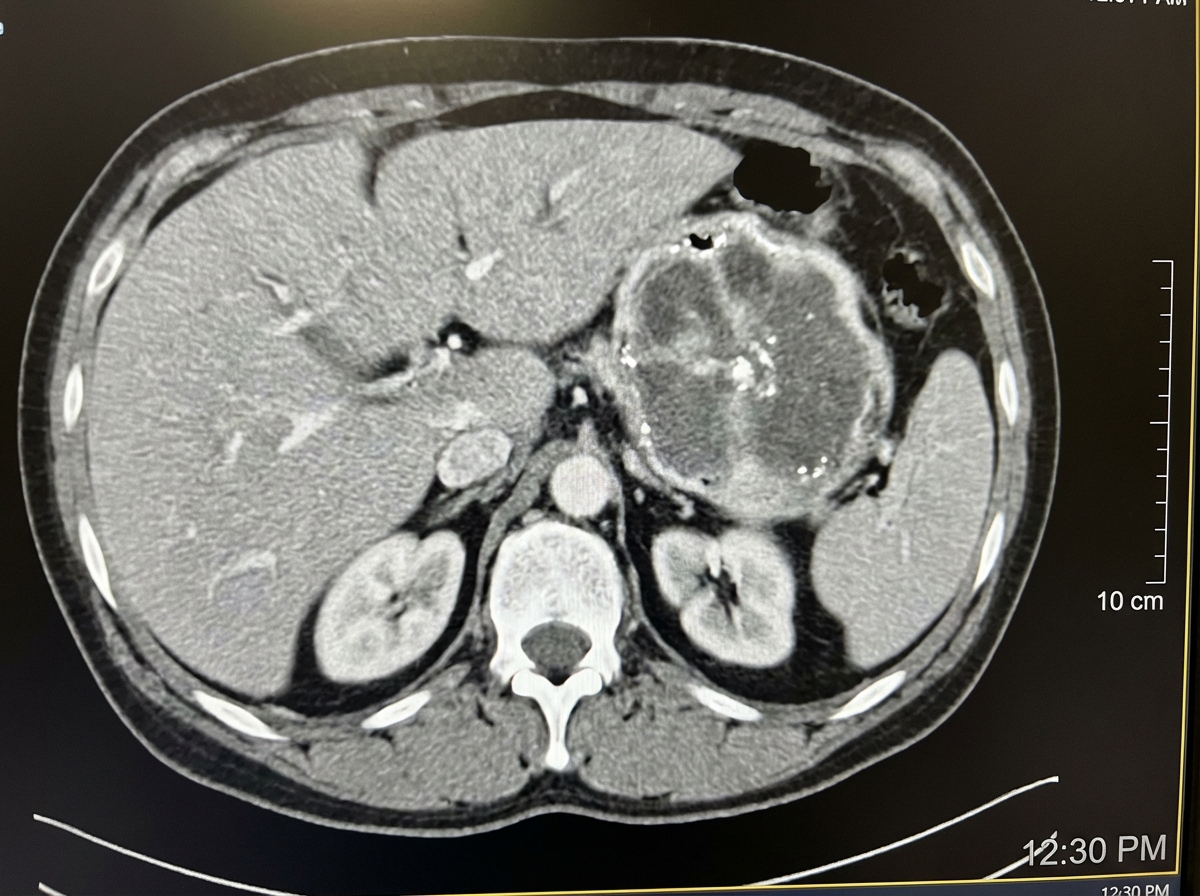
A 40-year-old patient presents with episodic hypertension, severe headache, diaphoresis, and palpitations. The CT scan of the abdomen is shown in the image. What is the most likely diagnosis?
Hypoglycemia is associated with all of the following conditions, EXCEPT:
Practice by Chapter
Diabetes Mellitus
Practice Questions
Thyroid Disorders
Practice Questions
Adrenal Gland Disorders
Practice Questions
Pituitary Disorders
Practice Questions
Calcium and Bone Metabolism
Practice Questions
Reproductive Endocrinology
Practice Questions
Lipid Disorders
Practice Questions
Endocrine Hypertension
Practice Questions
Multiple Endocrine Neoplasia
Practice Questions
Obesity and Metabolic Syndrome
Practice Questions
Neuroendocrine Tumors
Practice Questions
Endocrine Emergencies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
