Endocrinology — MCQs

On this page
A 40-year-old woman presents with an 8-month history of severe headaches, weakness, and dizziness. Her blood pressure is 180/110 mm Hg. Physical examination shows diminished tendon reflexes. An abdominal CT scan reveals a 4-cm mass in the right adrenal gland. Laboratory studies include serum potassium of 2.3 mEq/L, serum sodium of 155 mEq/L, plasma cortisol of 25 mg/dL (8 AM) and 20 mg/dL (4 PM), and low plasma renin. These clinical and laboratory findings are consistent with an adrenal tumor that secretes which of the following hormones?
Activation of the renin stimulates which of the following?
What is the most common symptom of thyrotoxicosis?
Hypercalcemia would not be expected to occur as a result of which of the following conditions?
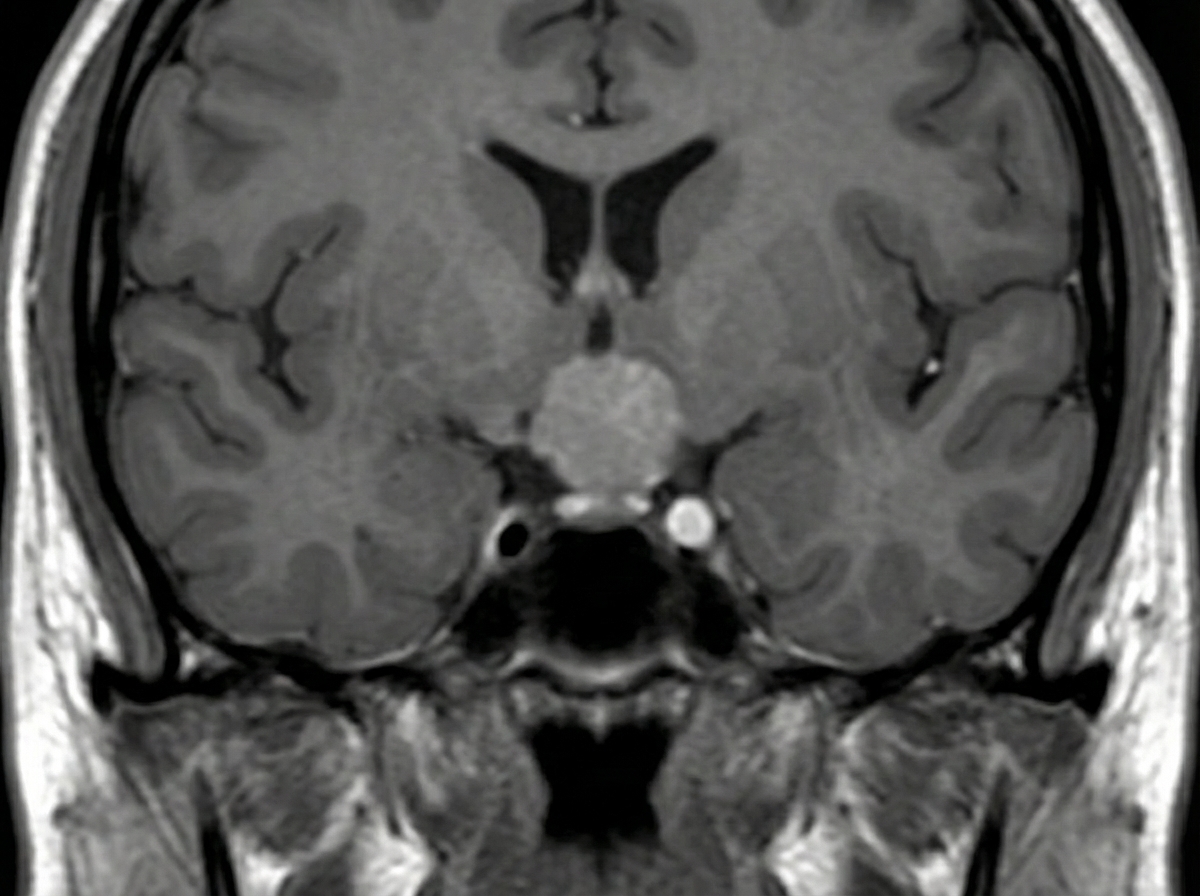
A 34-year-old man presents with a chief complaint of blurring of vision in both eyes and headache for the past six months, accompanied by decreased libido. Examination reveals bitemporal hemianopia. An MRI was performed. What is the most likely diagnosis?
Which of the following conditions can cause hypoglycemia, except?
The syndrome of inappropriate antidiuretic hormone (SIADH) is characterized by which of the following findings?
Grave's disease is characterized by:
Secondary hyperparathyroidism is seen in all of the following conditions EXCEPT:
What is characteristic of primary hyperaldosteronism?
Practice by Chapter
Diabetes Mellitus
Practice Questions
Thyroid Disorders
Practice Questions
Adrenal Gland Disorders
Practice Questions
Pituitary Disorders
Practice Questions
Calcium and Bone Metabolism
Practice Questions
Reproductive Endocrinology
Practice Questions
Lipid Disorders
Practice Questions
Endocrine Hypertension
Practice Questions
Multiple Endocrine Neoplasia
Practice Questions
Obesity and Metabolic Syndrome
Practice Questions
Neuroendocrine Tumors
Practice Questions
Endocrine Emergencies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
