Endocrinology — MCQs

On this page
Which of the following clinical features of diabetes insipidus is false?
A 63-year-old woman with Type 2 diabetes is seen for follow-up after a fasting lipid profile. She has no other medical conditions and feels well. Her diabetes is well controlled and the last hemoglobin A1c value was 6.5%. Her total cholesterol is 240 mg/dL, HDL is 50 mg/dL, low-density lipoprotein is 160 mg/dL, and triglycerides are 150 mg/dL. For this patient with dyslipidemia, what is the most appropriate treatment?
Which type of thyroiditis is also known as "Painless Thyroiditis"?
A 60-year-old man with small cell carcinoma of the lung presents to the emergency room in a coma after a clonic-tonic seizure. His temperature is 37°C, blood pressure is 100/50 mm Hg, and pulse is 88 per minute. Laboratory studies show a serum sodium of 103 mmol/L, normal serum levels of BUN and creatinine, and a dilute but otherwise normal urine. A CT scan of the head is normal. What is the most likely cause of seizures in this patient?
A 40-year-old lady presents with weight loss and palpitations, having a heart rate of 110/min, BP 130/70 mmHg, bilateral proptosis, and warm, moist skin. Investigations show undetectable TSH and normal free T4. What is the next best step in diagnosis?
Diffuse toxic goiter is characterized by:
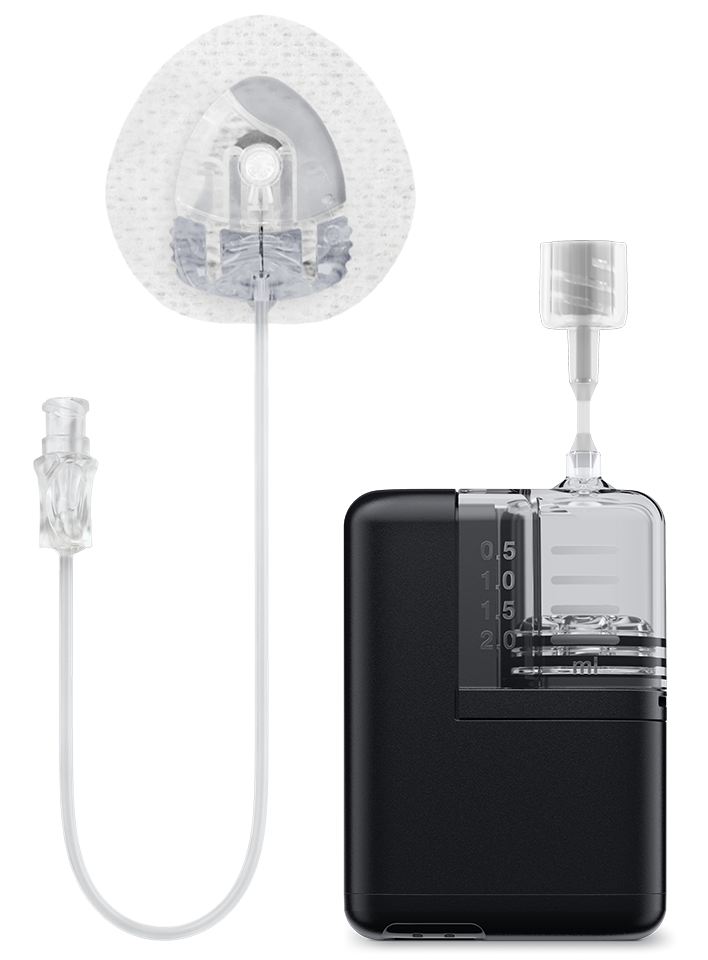
Which of the following is NOT a complication arising out of the use of the medical device shown?
Obesity is associated with all the following conditions except?
A 53-year-old woman presents with weight loss, increased appetite, sweating, palpitations, and preference for cold weather, hot, moist palms, and tremors. What is the best investigation for the clinical diagnosis of this patient?
Eosinopenia occurs in which of the following conditions?
Practice by Chapter
Diabetes Mellitus
Practice Questions
Thyroid Disorders
Practice Questions
Adrenal Gland Disorders
Practice Questions
Pituitary Disorders
Practice Questions
Calcium and Bone Metabolism
Practice Questions
Reproductive Endocrinology
Practice Questions
Lipid Disorders
Practice Questions
Endocrine Hypertension
Practice Questions
Multiple Endocrine Neoplasia
Practice Questions
Obesity and Metabolic Syndrome
Practice Questions
Neuroendocrine Tumors
Practice Questions
Endocrine Emergencies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
