Endocrinology — MCQs

On this page
Which of the following is the LEAST likely symptom of hyperthyroidism in a 77-year-old man?
Which of the following obesity-related syndromes is associated with hypogonadism in males but not in females?
Anuria is defined as urine output less than?
All of the following are true of cerebral salt wasting syndrome, except:
Which of the following is NOT a primary cause of hypogonadism?
A 40-year-old female presenting with intolerance to cold, constipation, and hoarseness of voice was found to have cardiomegaly on chest roentgenogram. Which of the following investigations is the best to determine the cause of her cardiomegaly?
A 30-year-old female complains of palpitations, fatigue, and insomnia. On physical exam, her extremities are warm and she is tachycardic. There is diffuse thyroid gland enlargement and proptosis. There is a thickening of the skin in the pretibial area. Which of the following lab values would you expect in this patient?
Which of the following is not typically seen in Cushing syndrome?
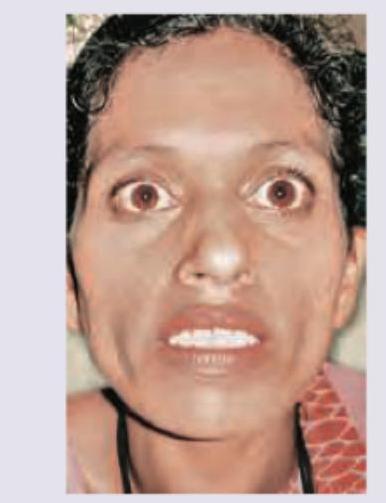
Which condition is characterized by the following clinical feature?
Which of the following is NOT seen in hyperparathyroidism?
Practice by Chapter
Diabetes Mellitus
Practice Questions
Thyroid Disorders
Practice Questions
Adrenal Gland Disorders
Practice Questions
Pituitary Disorders
Practice Questions
Calcium and Bone Metabolism
Practice Questions
Reproductive Endocrinology
Practice Questions
Lipid Disorders
Practice Questions
Endocrine Hypertension
Practice Questions
Multiple Endocrine Neoplasia
Practice Questions
Obesity and Metabolic Syndrome
Practice Questions
Neuroendocrine Tumors
Practice Questions
Endocrine Emergencies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
