Endocrinology — MCQs

On this page
All of the following are true about Graves disease except?
Which of the following statements is not true regarding Hashimoto's thyroiditis?
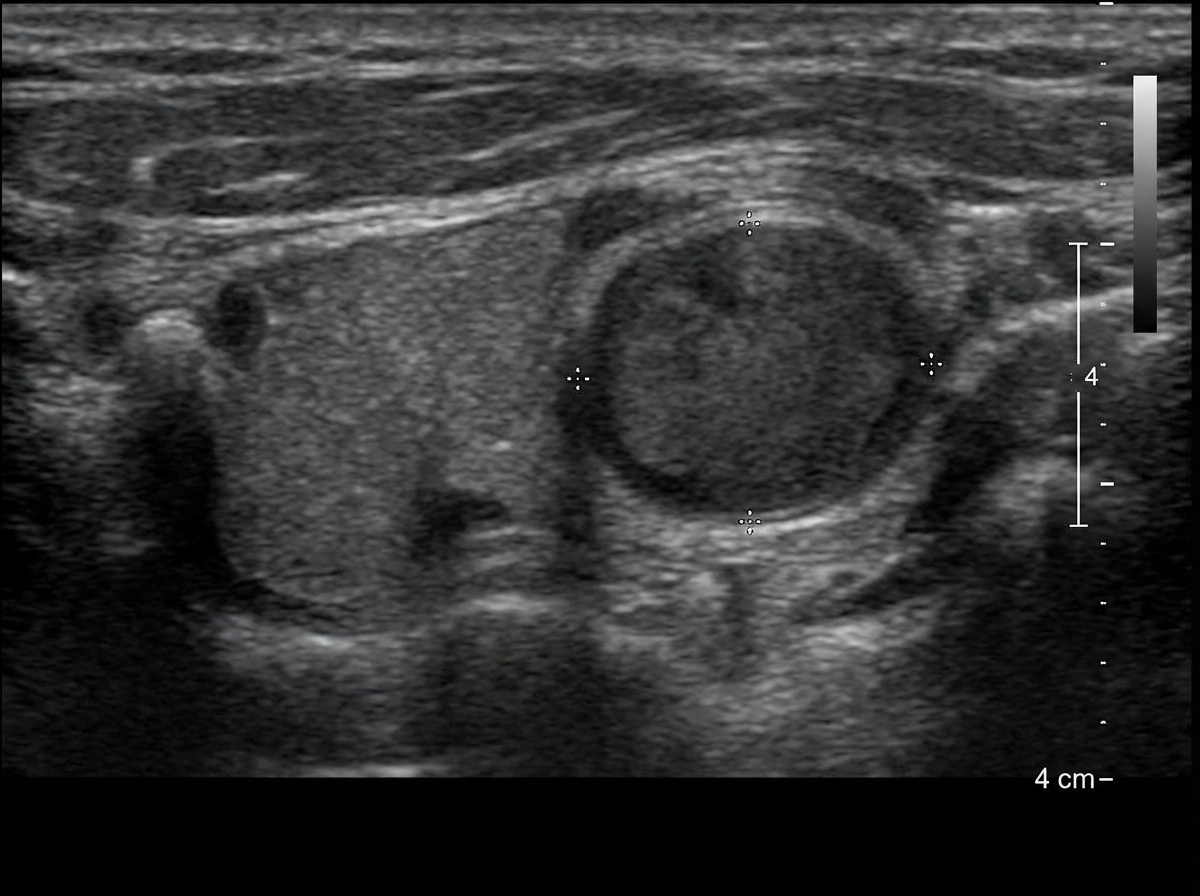
What laboratory test is most appropriate for this patient?
In osteoporosis, what change occurs?
A 68-year-old patient, postoperative from thyroidectomy, presents with muscle cramps. Chvostek's and Trousseau's signs are noted on examination. What is the most likely finding on electrocardiogram?
All of the following statements about Pseudohypoparathyroidism are true, except?
Which of the following is true for Klinefelter's syndrome?
Which of the following is NOT a feature of Kallmann syndrome?
All of the following are helpful in the initial treatment of severe hypercalcemia associated with hyperparathyroidism except?
Weight gain is seen in all of the following conditions except?
Practice by Chapter
Diabetes Mellitus
Practice Questions
Thyroid Disorders
Practice Questions
Adrenal Gland Disorders
Practice Questions
Pituitary Disorders
Practice Questions
Calcium and Bone Metabolism
Practice Questions
Reproductive Endocrinology
Practice Questions
Lipid Disorders
Practice Questions
Endocrine Hypertension
Practice Questions
Multiple Endocrine Neoplasia
Practice Questions
Obesity and Metabolic Syndrome
Practice Questions
Neuroendocrine Tumors
Practice Questions
Endocrine Emergencies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
