Injuries and Their Significance — MCQs

On this page
Heat rupture can be differentiated from an incised wound by which of the following?
Overlying leads to death due to which of the following mechanisms?
Black gunpowder is primarily composed of which substances?
What is the most common organ affected by underwater blast injuries?
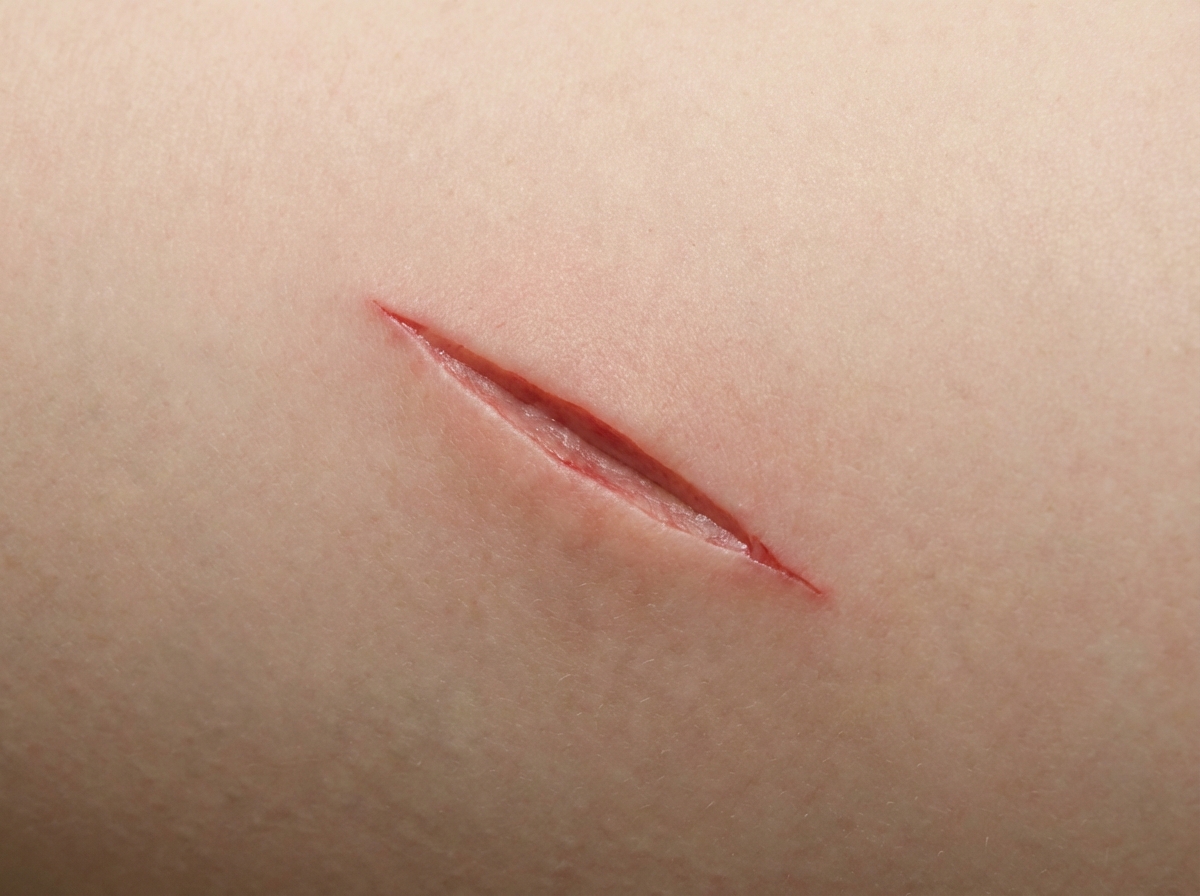
What type of inflicted weapon is suggested by the wound characteristics?
What is the effective range of a rifle?
Ante-mortem and post-mortem wounds could be differentiated by all, except:
The Rule of Nines is related to which of the following?
In cases of perforating stab wounds, which of the following is true?
In deceleration accidents, which of the following fixed parts of the aorta is not ruptured?
Practice by Chapter
Mechanical Injuries
Practice Questions
Transportation Injuries
Practice Questions
Fall from Height
Practice Questions
Blunt Force Trauma
Practice Questions
Sharp Force Trauma
Practice Questions
Ballistic Injuries
Practice Questions
Burn Injuries
Practice Questions
Drowning
Practice Questions
Electrocution
Practice Questions
Lightning Injuries
Practice Questions
Explosion Injuries
Practice Questions
Pattern Injuries and Their Recognition
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
