Forensic Toxicology — MCQs

On this page
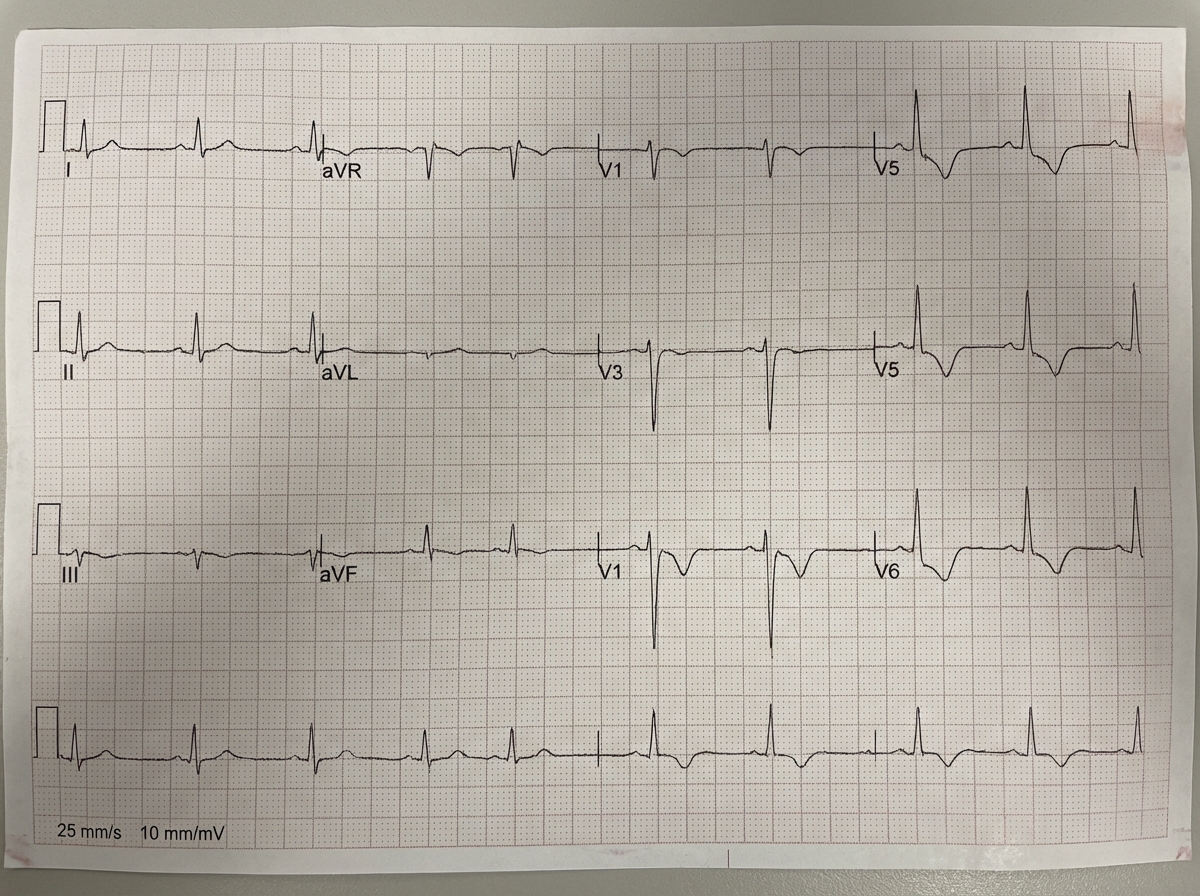
A 10-year-old girl was admitted to the emergency room with a history of ingesting 10 crushed seeds of an unknown plant. Her ECG showed specific abnormalities. What is the probable cause of these ECG changes?
Shedding of red tears is seen in which of the following conditions?
Rain drop pigmentation is seen in:
Green colored urine is found in which of the following conditions?
Two individuals presented with symptoms and subsequently died. A distinctive smell of bitter almonds was noted emanating from their mouths. These deaths are suspected to be due to which poison?
A middle-aged man presents with paresthesia of the hands and feet. Examination reveals 'Mees' lines in the nails and raindrop pigmentation on the hands. What is the most likely causative toxin for these symptoms?
Which substance is typically excreted in lead poisoning?
If the 4th infralabial scale is larger than others on either side, the snake may be:
A factory worker presented with tremors, personality change, and a blue line in the gum. What is the probable diagnosis of chronic poisoning with?
What is the fatal dose of potassium cyanide?
Practice by Chapter
General Principles of Toxicology
Practice Questions
Corrosive Poisons
Practice Questions
Metallic Poisons
Practice Questions
Non-Metallic Poisons
Practice Questions
Organic Irritant Poisons
Practice Questions
Neurotic Poisons
Practice Questions
Cardiac Poisons
Practice Questions
Asphyxiant Poisons
Practice Questions
Food Poisoning
Practice Questions
Drug Abuse and Dependence
Practice Questions
Analytical Toxicology Methods
Practice Questions
Interpretation of Toxicology Results
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
