Pediatric Otolaryngology — MCQs

On this page
Cyanosis in a newborn that disappears on crying is characteristic of which condition?
Which of the following is a feature of Scheibe's syndrome?
The most likely cause of persistent snoring and mouth breathing in a child is:
A 5-year-old boy, while having dinner, suddenly develops phonation difficulty and stridor, and is brought to the casualty department with complaints of respiratory distress. What is the most appropriate immediate management?
What is the percentage of newborns with deviation of the nasal septum?
What is the most common congenital anomaly of the larynx?
What is a recognized cause of stridor in a newborn?
Which of the following is the commonest cause of stridor in a newborn?
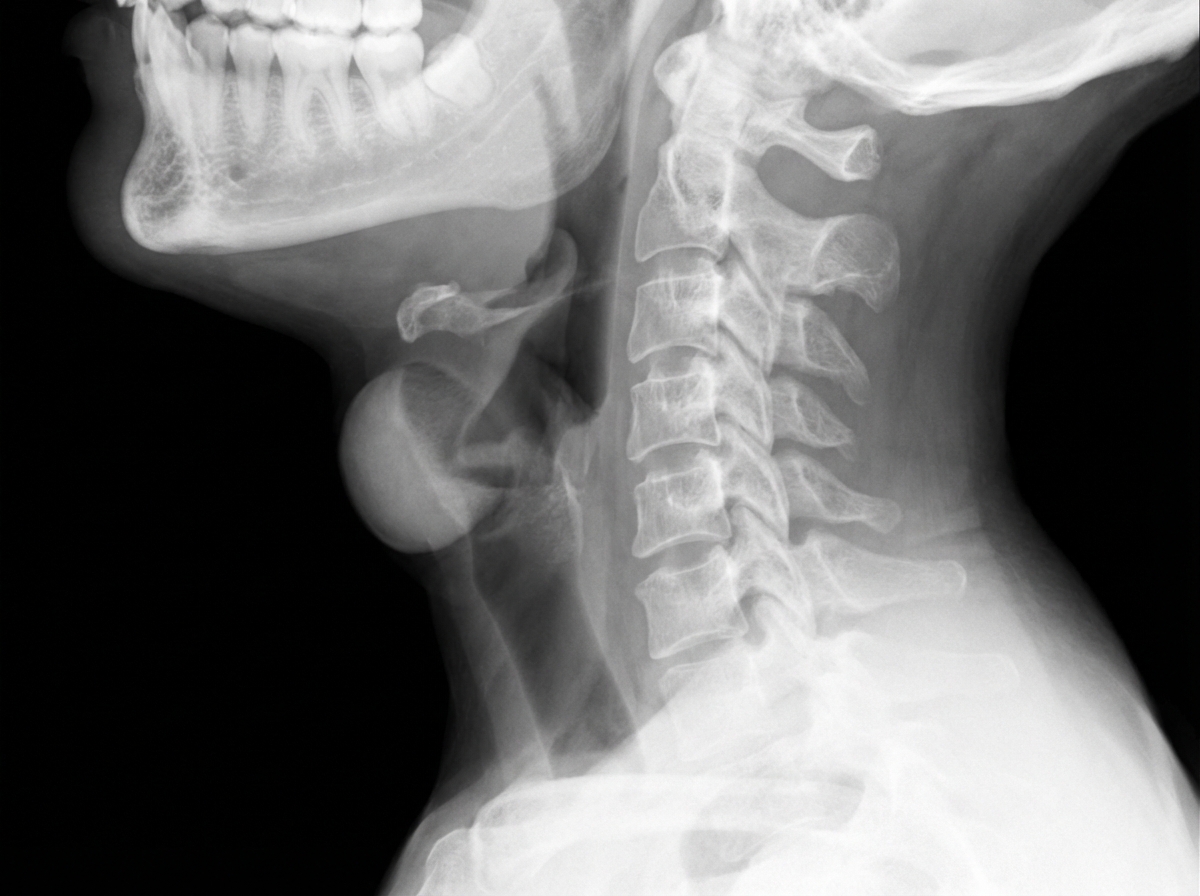
A 4-year-old child presents to the emergency department with high-grade fever, respiratory difficulty, and noisy breathing. An X-ray of his neck is shown below. What is the most probable diagnosis?
What is the main treatment for congenital laryngeal stridor?
Practice by Chapter
Congenital Anomalies of the Ear
Practice Questions
Pediatric Hearing Loss
Practice Questions
Otitis Media in Children
Practice Questions
Pediatric Sinusitis
Practice Questions
Pediatric Sleep Apnea
Practice Questions
Stridor in Children
Practice Questions
Congenital Airway Anomalies
Practice Questions
Foreign Body Management
Practice Questions
Pediatric Head and Neck Masses
Practice Questions
Pediatric Tracheostomy
Practice Questions
Pediatric Voice Disorders
Practice Questions
Pierre Robin Sequence and Airway Management
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
