Otology — MCQs

On this page
Loudness recruitment phenomenon is associated with which type of hearing loss?
Types of tympanoplasty include all except?
Which of the following is NOT true about otitic barotrauma?
Which abscess is related to the sternocleidomastoid muscle?
What is the indication for radical mastoidectomy in a middle-aged female?
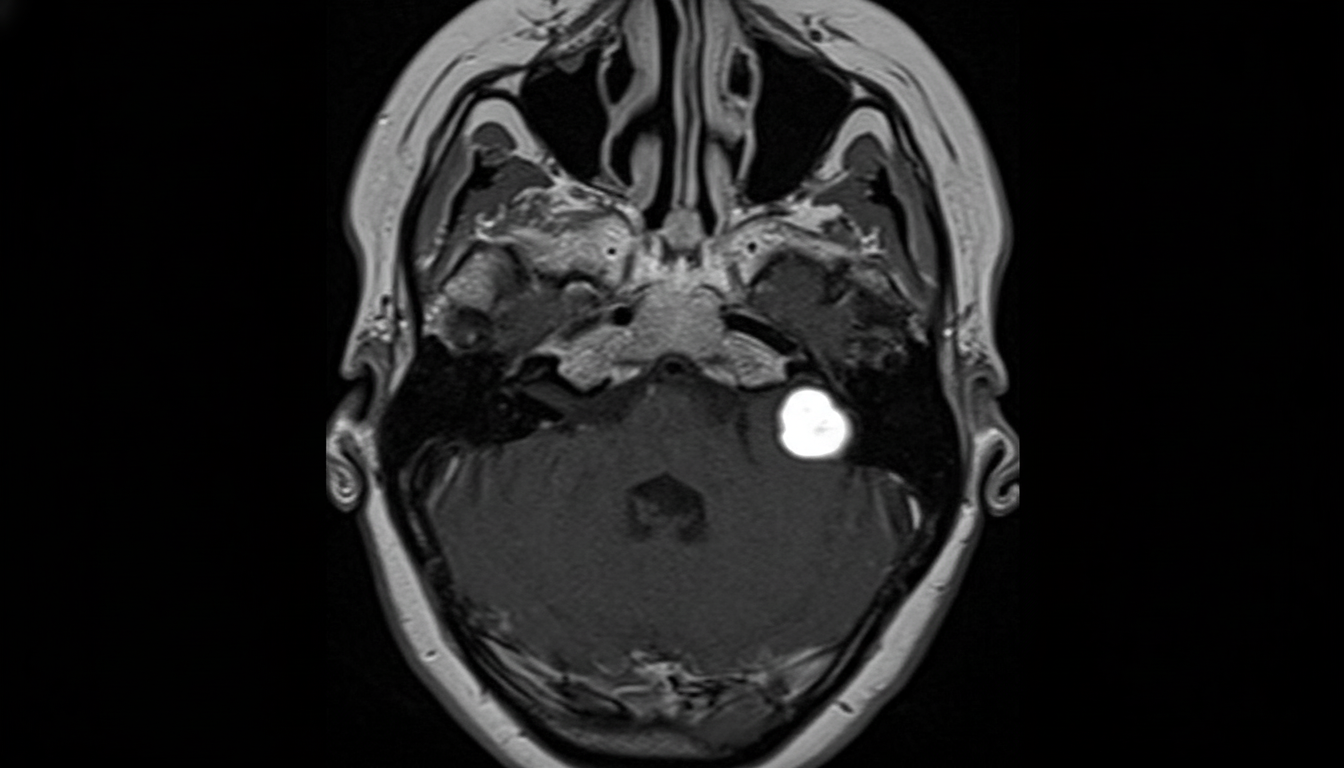
A 70-year-old man presents with tinnitus. What is the most probable diagnosis?
A 12-year-old child presents with fever, unilateral postauricular pain, and mastoid bulging that displaces the pinna forward and outward, with loss of bony trabeculae. The patient has a history of chronic persistent pus discharge from the same ear. What is the treatment of choice?
A diabetic female patient presents with severe ear pain, granulation tissue in the external auditory canal, and facial palsy. What is the most likely diagnosis?
For Grommet tube insertion in serous otitis media, where is the incision on the tympanic membrane typically made?
In which quadrant is myringotomy typically performed?
Practice by Chapter
Tympanic Membrane Perforation
Practice Questions
Cholesteatoma
Practice Questions
Tympanoplasty Techniques
Practice Questions
Ossicular Chain Reconstruction
Practice Questions
Mastoidectomy
Practice Questions
Stapedectomy
Practice Questions
Implantable Hearing Devices
Practice Questions
Congenital Aural Atresia
Practice Questions
Otologic Trauma
Practice Questions
Glomus Tumors
Practice Questions
Facial Nerve Decompression
Practice Questions
Rehabilitative Audiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
