Otology — MCQs

On this page
Identify the treatment option with the image given below:
A 35-year-old woman presented to the clinic with the symptoms of hearing loss and pulsatile tinnitus. Further examination reveals conductive hearing loss with the Rinne test negative. A reddish mass is seen behind the tympanic membrane. What is the most likely diagnosis for this patient?
A patient presents to the clinic with a history of chronic ear drainage and hearing loss for several months. Otoscopic examination reveals a central perforation of the tympanic membrane. Pure tone audiometry confirms a conductive hearing loss. Based on these findings, what is the most appropriate next step in the definitive management of this patient's condition?
A 30-year-old male presents to the clinic with a history of recurrent ear infections and a recent "popping" sensation in his left ear. Otoscopic examination of the left ear reveals a central perforation of the tympanic membrane. The pure tone audiometry (PTA) results show the following: Right Ear: Air conduction and bone conduction thresholds are within normal limits. Left Ear: A significant air-bone gap is present, with bone conduction thresholds within the normal range. Based on these findings, what is the most likely diagnosis regarding the type of hearing loss?
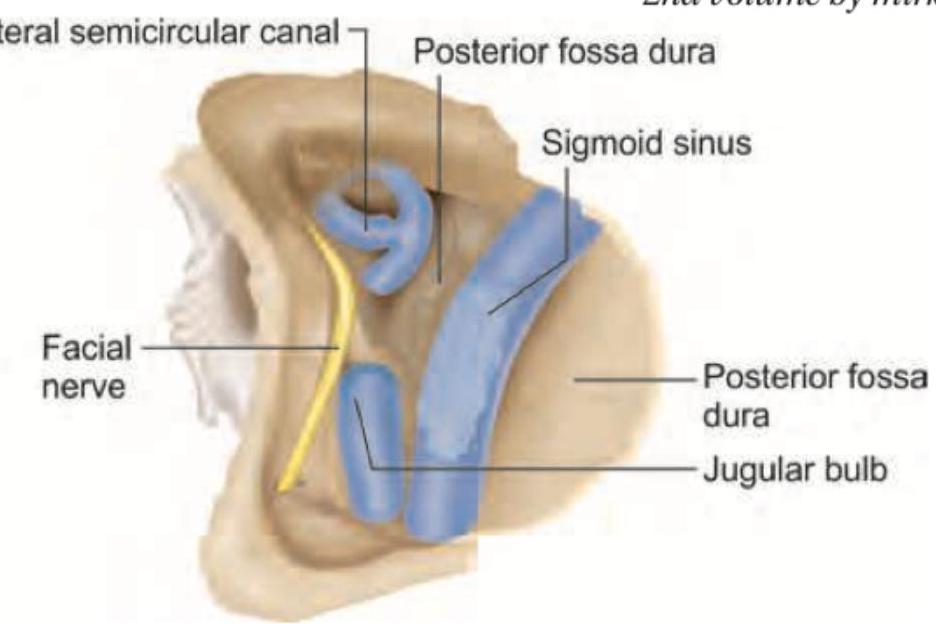
Identify the structure marked in the given image:
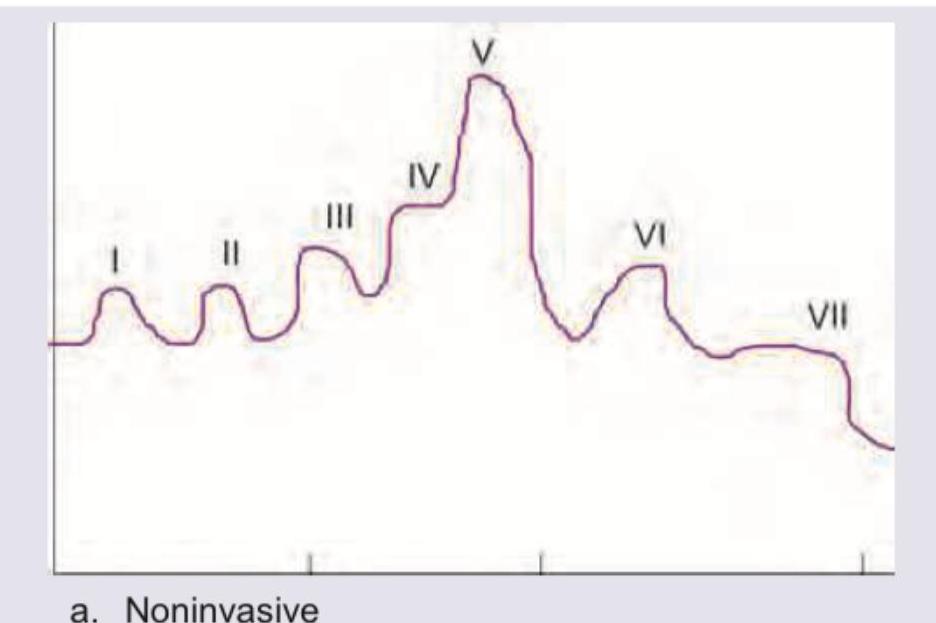
All are true about the recording shown in the image except:
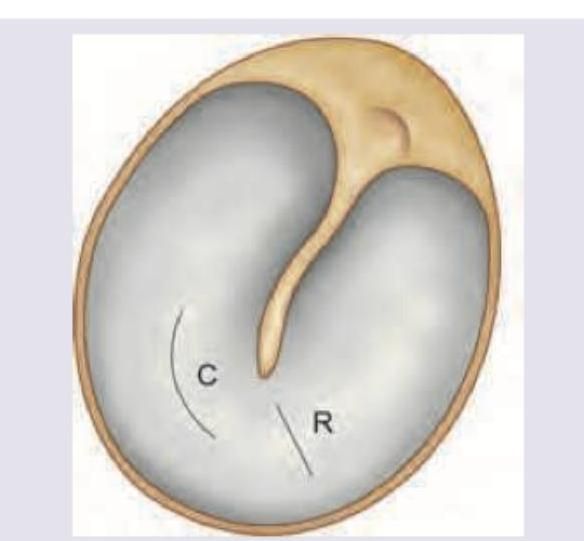
Which of the following is a contraindication to the procedure shown below?
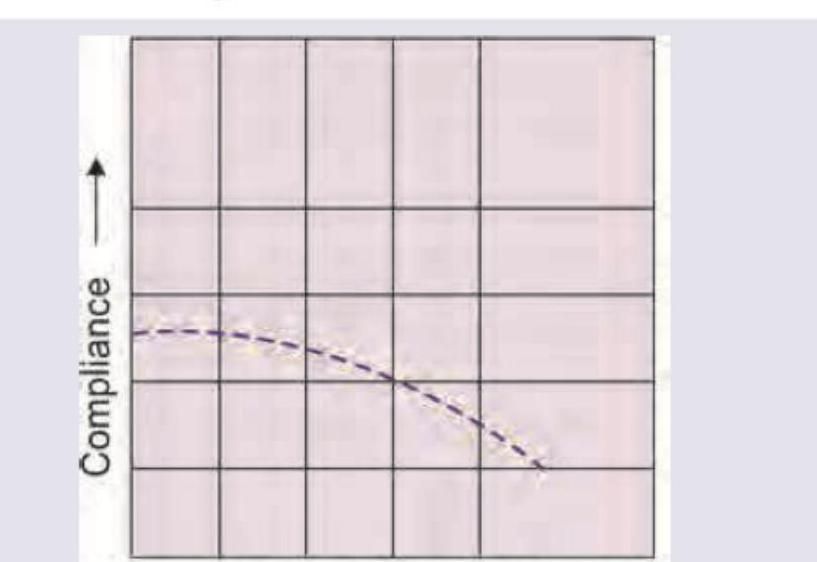
The tympanogram shown below is seen in which of the following conditions?
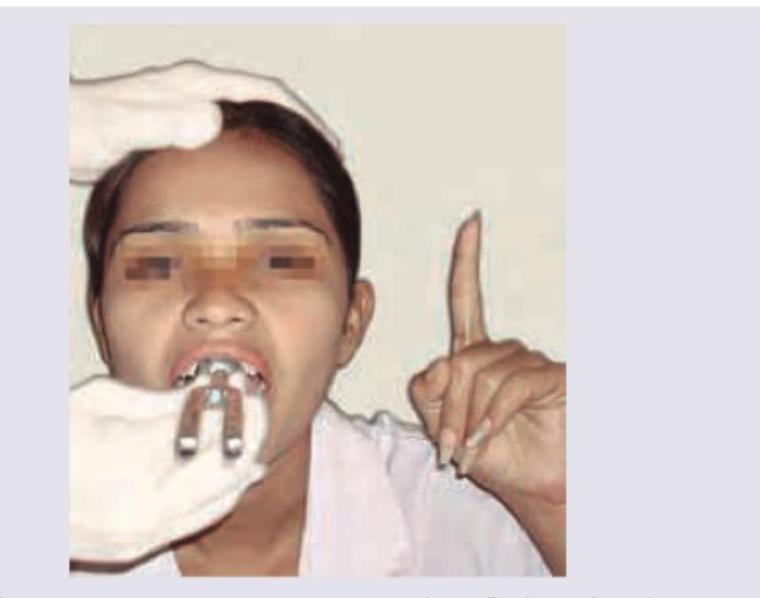
Which test is being performed in the patient?
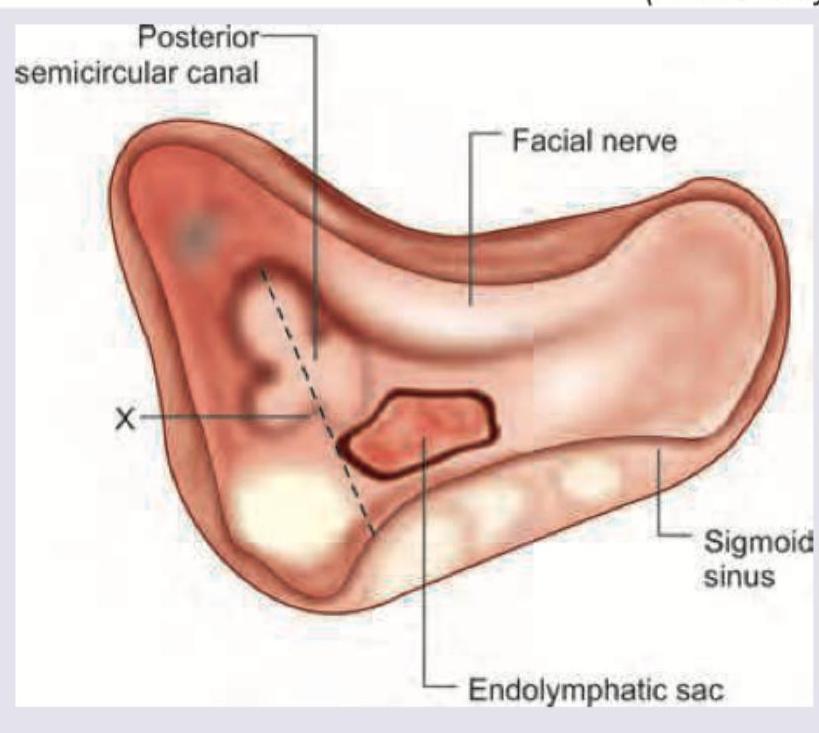
Identify the line shown in the given image:
Practice by Chapter
Tympanic Membrane Perforation
Practice Questions
Cholesteatoma
Practice Questions
Tympanoplasty Techniques
Practice Questions
Ossicular Chain Reconstruction
Practice Questions
Mastoidectomy
Practice Questions
Stapedectomy
Practice Questions
Implantable Hearing Devices
Practice Questions
Congenital Aural Atresia
Practice Questions
Otologic Trauma
Practice Questions
Glomus Tumors
Practice Questions
Facial Nerve Decompression
Practice Questions
Rehabilitative Audiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
