Otology — MCQs

On this page
What is the scutum?
Cauliflower ear is due to what condition?
Endolymphatic decompression is indicated for which condition?
An elderly diabetic patient consults a physician due to severe earache. Examination reveals foul-smelling purulent otorrhea and a red mass lesion in the external ear canal. Biopsy of the mass demonstrates granulation tissue. What is the most likely causative organism?
Pulsatile tinnitus in the ear is most commonly due to which of the following conditions?
A 3-year-old girl ruptured her eardrum when she inserted a pencil into her ear. Her mother took her to the emergency department after noticing that the child was crying and complaining of pain in her ear with a few drops of blood in the external auditory meatus. The attending doctor examined the child for possible injury to a nerve that runs across the eardrum. Which is the MOST likely nerve to be injured?
Galle's test is used for which of the following conditions?
What is the most mobile part of the tympanic membrane?
A 60-year-old lady presented with mild hearing loss and pulsatile tinnitus of the right ear. Otoscopy revealed specific findings. What is the most probable diagnosis?
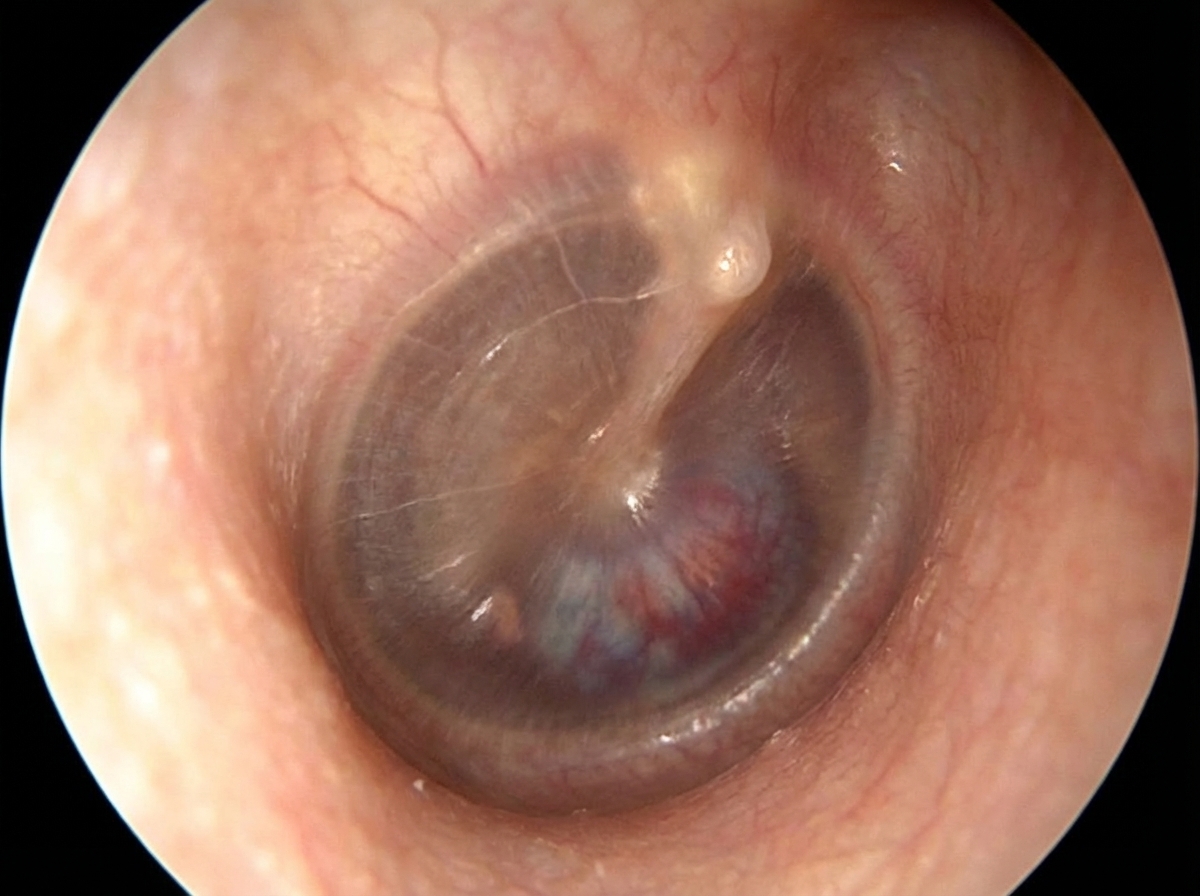
A one-year-old child presents with bilateral hearing difficulty. Impedance audiometry shows a Type B curve and there is a bilateral conductive hearing deficit. There are no signs of infection. What is the next step?
Practice by Chapter
Tympanic Membrane Perforation
Practice Questions
Cholesteatoma
Practice Questions
Tympanoplasty Techniques
Practice Questions
Ossicular Chain Reconstruction
Practice Questions
Mastoidectomy
Practice Questions
Stapedectomy
Practice Questions
Implantable Hearing Devices
Practice Questions
Congenital Aural Atresia
Practice Questions
Otologic Trauma
Practice Questions
Glomus Tumors
Practice Questions
Facial Nerve Decompression
Practice Questions
Rehabilitative Audiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
