Otology — MCQs

On this page
What are the indications for a brain stem implant in a two-year-old child?
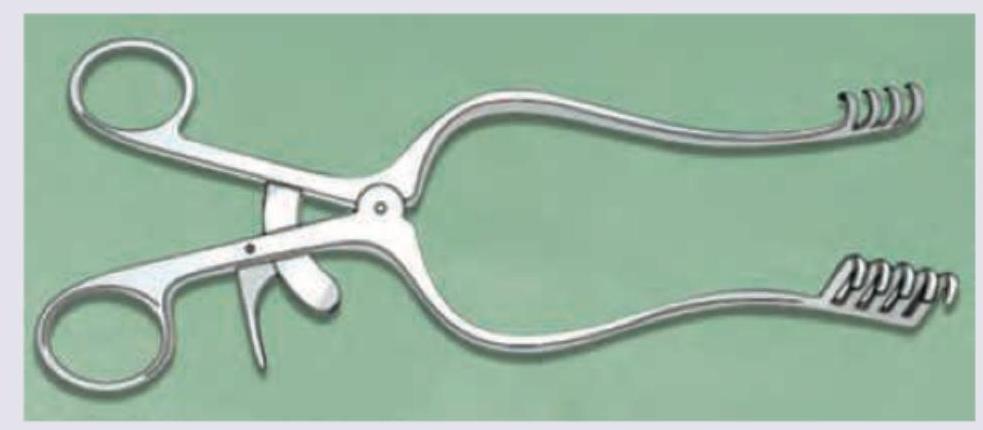
All of the following are uses of the given instrument except:
Otitic barotrauma occurs during which of the following activities?
Which of the following is NOT a test for Eustachian tube function?
Which part of the middle ear is most commonly involved in otosclerosis?
A child presents with a three-month history of left ear hearing loss. On examination, foul-smelling purulent discharge is observed, along with a perforation in the pars flaccida. What is the most appropriate management?
For acute otitis media (AOM), in which quadrant of the tympanic membrane is a myringotomy typically performed?
Atticoantral disease is treated by which surgical approach?
What procedure involves widening of the cartilaginous part of the external auditory canal?
Which of the following materials are commonly used in tympanoplasty?
Practice by Chapter
Tympanic Membrane Perforation
Practice Questions
Cholesteatoma
Practice Questions
Tympanoplasty Techniques
Practice Questions
Ossicular Chain Reconstruction
Practice Questions
Mastoidectomy
Practice Questions
Stapedectomy
Practice Questions
Implantable Hearing Devices
Practice Questions
Congenital Aural Atresia
Practice Questions
Otologic Trauma
Practice Questions
Glomus Tumors
Practice Questions
Facial Nerve Decompression
Practice Questions
Rehabilitative Audiology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
