Diseases of the Oral Cavity and Salivary Glands — MCQs

On this page
A person experiences throbbing pain at night. What is the most likely cause?
Facial nerve paralysis is commonly associated with which of the following conditions?
A 50-year-old male with a history of chronic smoking and alcohol intake presents with an oral cavity lesion. What is the most probable diagnosis?
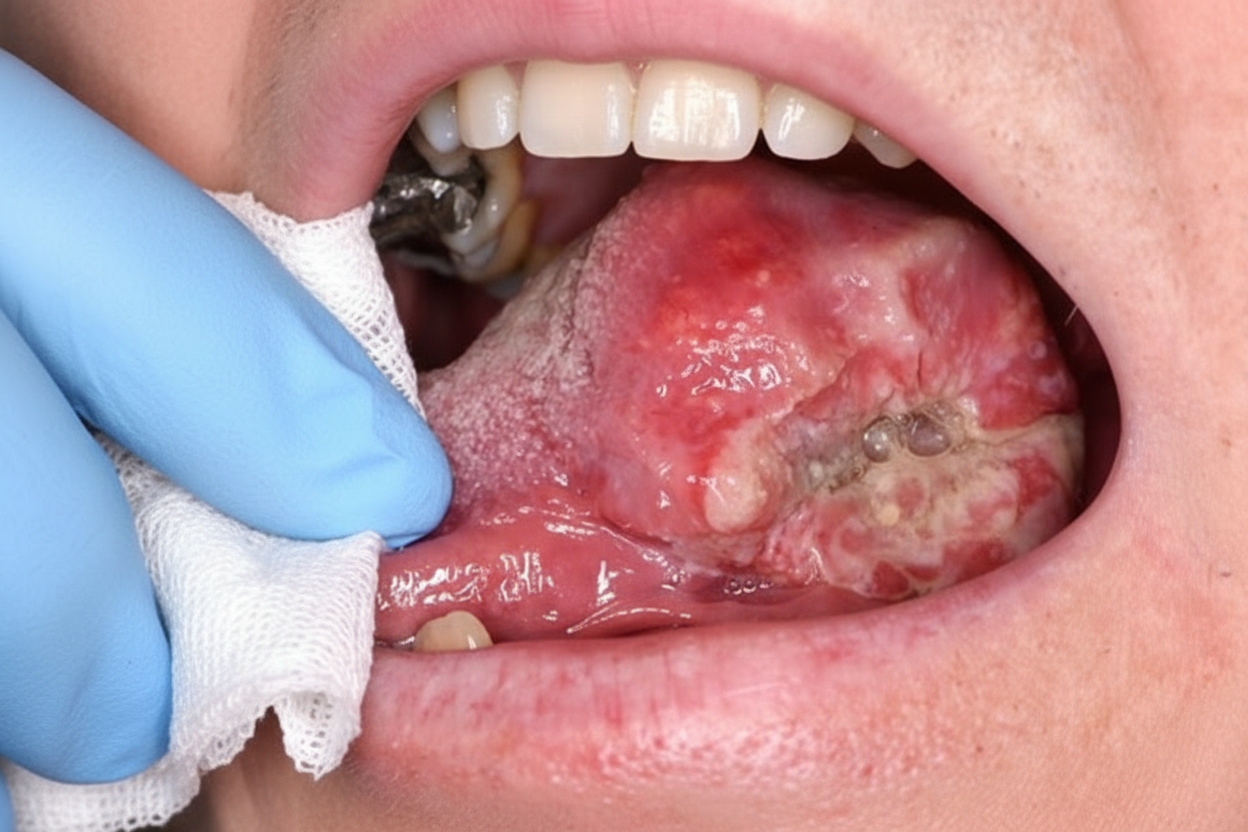
What is the most common histological type of carcinoma of the tongue?
Which of the following is NOT a vital part of the physical examination for patients with temporomandibular joint (TMJ) complaints?
Invasion of the perineural space is a characteristic feature of which of the following tumors?
What is the pathognomonic finding in sialography for Sjogren syndrome?
Major aphthous ulcers are seen in which of the following conditions?
Patey's operation refers to which of the following procedures?
What is the most common route for furcation involvement of the maxillary permanent first molar?
Practice by Chapter
Stomatitis
Practice Questions
Oral Ulcers
Practice Questions
Oral Leukoplakia
Practice Questions
Oral Cancers
Practice Questions
Sialadenitis
Practice Questions
Sialolithiasis
Practice Questions
Salivary Gland Tumors
Practice Questions
Ranula
Practice Questions
Xerostomia
Practice Questions
Sjögren's Syndrome
Practice Questions
Oral Manifestations of Systemic Diseases
Practice Questions
Temporomandibular Joint Disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
