Diseases of the Larynx — MCQs

On this page
Right-sided vocal cord palsy is most commonly seen in which of the following conditions?
Vocal cord palsy is NOT associated with which of the following conditions?
What is the typical resting position of a vocal cord in a cadaver?
Which of the following subunits is associated with inspiratory stridor?
Which of the following is true about laryngeal cancer stage T1bNOMO?
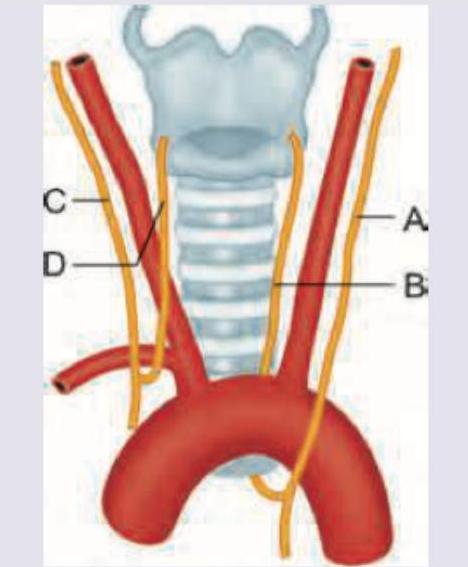
Which of the following is shown in the image below?
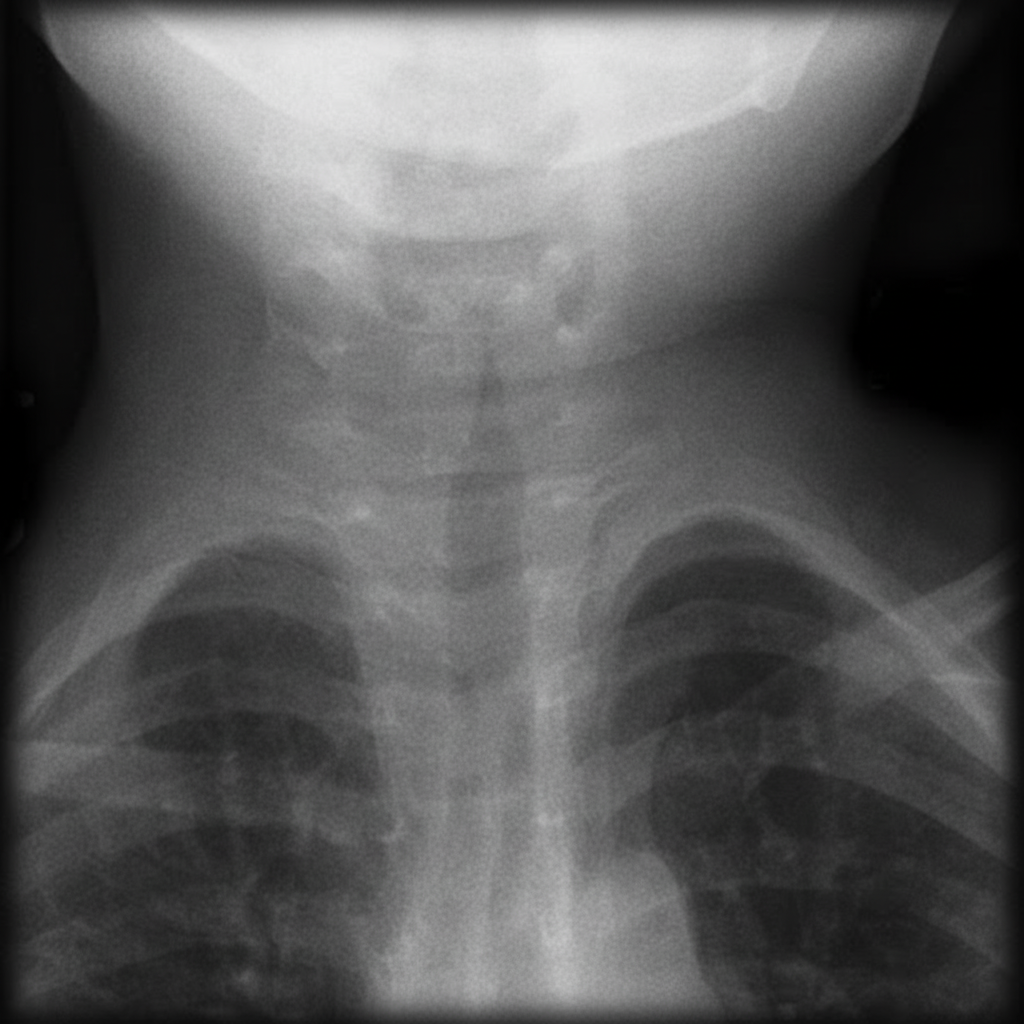
All of the following are correct about the image shown except:
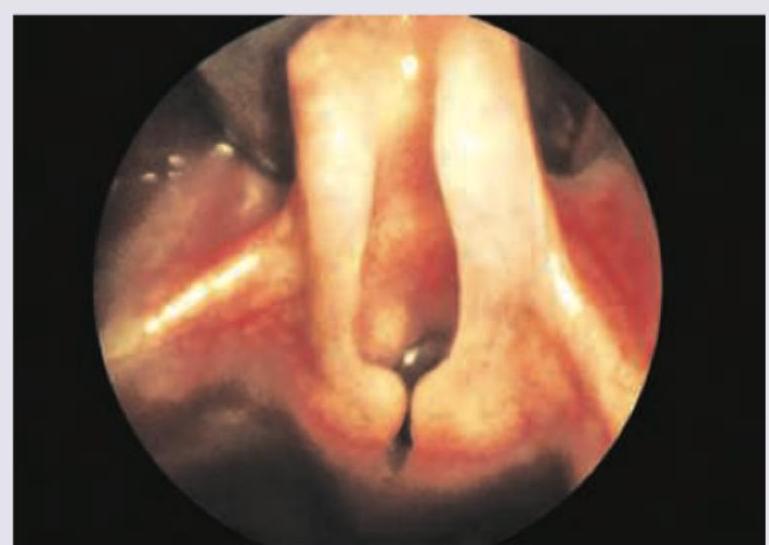
What is the most likely diagnosis shown in the image?
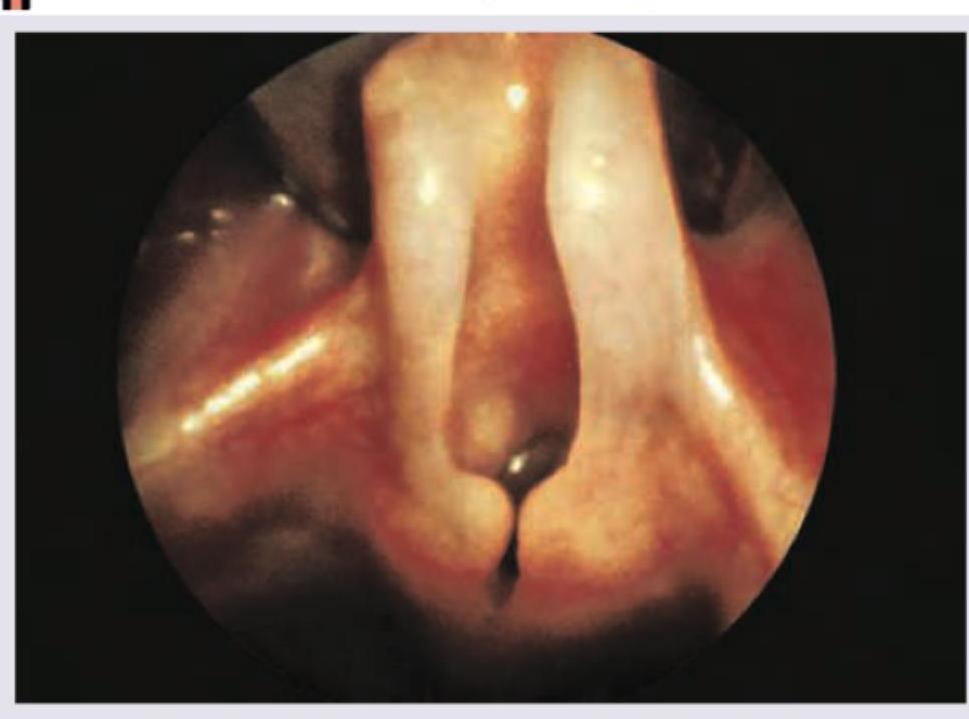
A 14-year-old teenager presents with hoarseness of voice. Which of the following is responsible for the lesion shown in the figure?
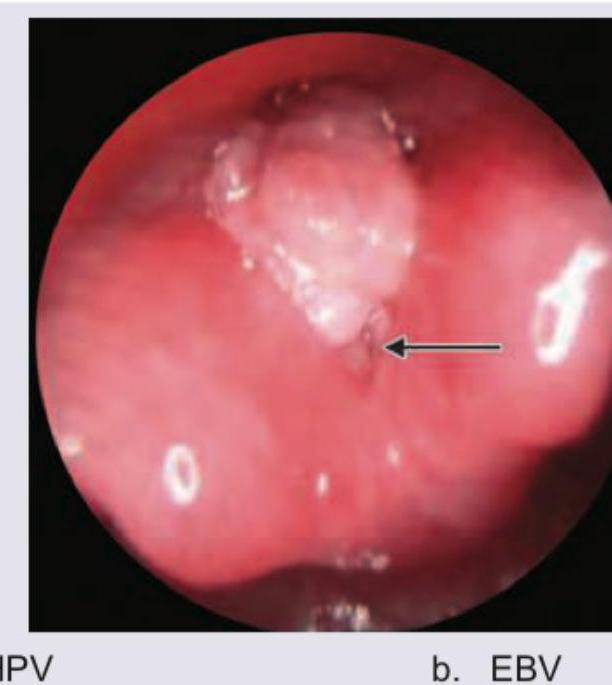
A 60-year-old smoker presents with history of weight loss and thyroid swelling which is hard in consistency. Surgery was performed after which nerve B and D shown in the diagram got involved. All are true about the resultant condition except:
Practice by Chapter
Acute Laryngitis
Practice Questions
Chronic Laryngitis
Practice Questions
Vocal Cord Nodules and Polyps
Practice Questions
Reinke's Edema
Practice Questions
Laryngeal Papillomatosis
Practice Questions
Vocal Cord Paralysis
Practice Questions
Laryngeal Trauma
Practice Questions
Laryngeal Stenosis
Practice Questions
Laryngeal Cancer
Practice Questions
Laryngomalacia
Practice Questions
Epiglottitis
Practice Questions
Voice Disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
