Phototherapy and Biologics for Psoriasis — MCQs

What is the primary condition for which calcitriol is used as a treatment?
Which one of these should not be used in severe widespread psoriasis?
PUVA therapy is used in all except:
A 45 year old female presents with the complaint of pain in the metacarpophalangeal, proximal interphalangeal and metatarsophalangeal joints of both right and left hands. Serology showed positive anti-CCP antibodies. She was placed on infliximab for control. Which of the following need to tested before starting treatment?
In which of the following conditions are Anti-TNF agents contraindicated?
A 40-year-old male presents with fever and abdominal pain and is diagnosed with HIV and TB. What is the most appropriate sequence of treatment?
Treatment of choice for Pustular psoriasis is:
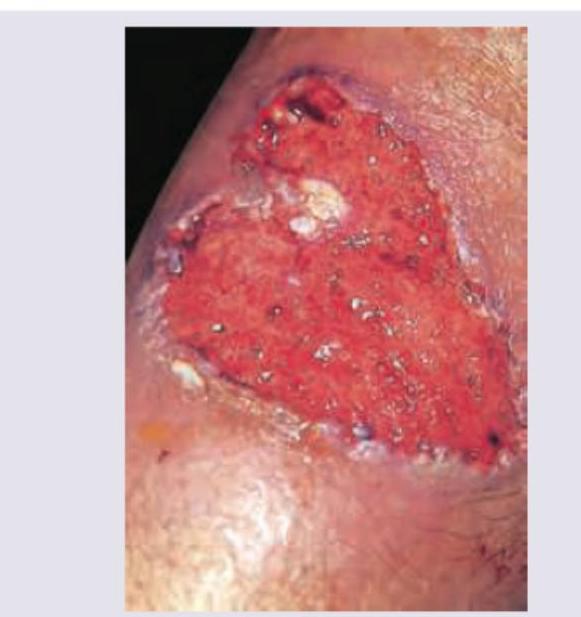
The following lesion appears on the leg of a patient of ulcerative colitis. All are useful in management except:
An 8-year-old girl has extreme photosensitivity since birth. She has recently been diagnosed with skin cancer. What is the diagnosis?
A 16-year-old boy presented with asymptomatic, multiple erythematous annular lesions with a collarette of scales at the periphery of the lesions present on the trunk. What is the most likely diagnosis?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
