Psoriasis — MCQs

On this page
Which of the following is true about the specified skin disease?
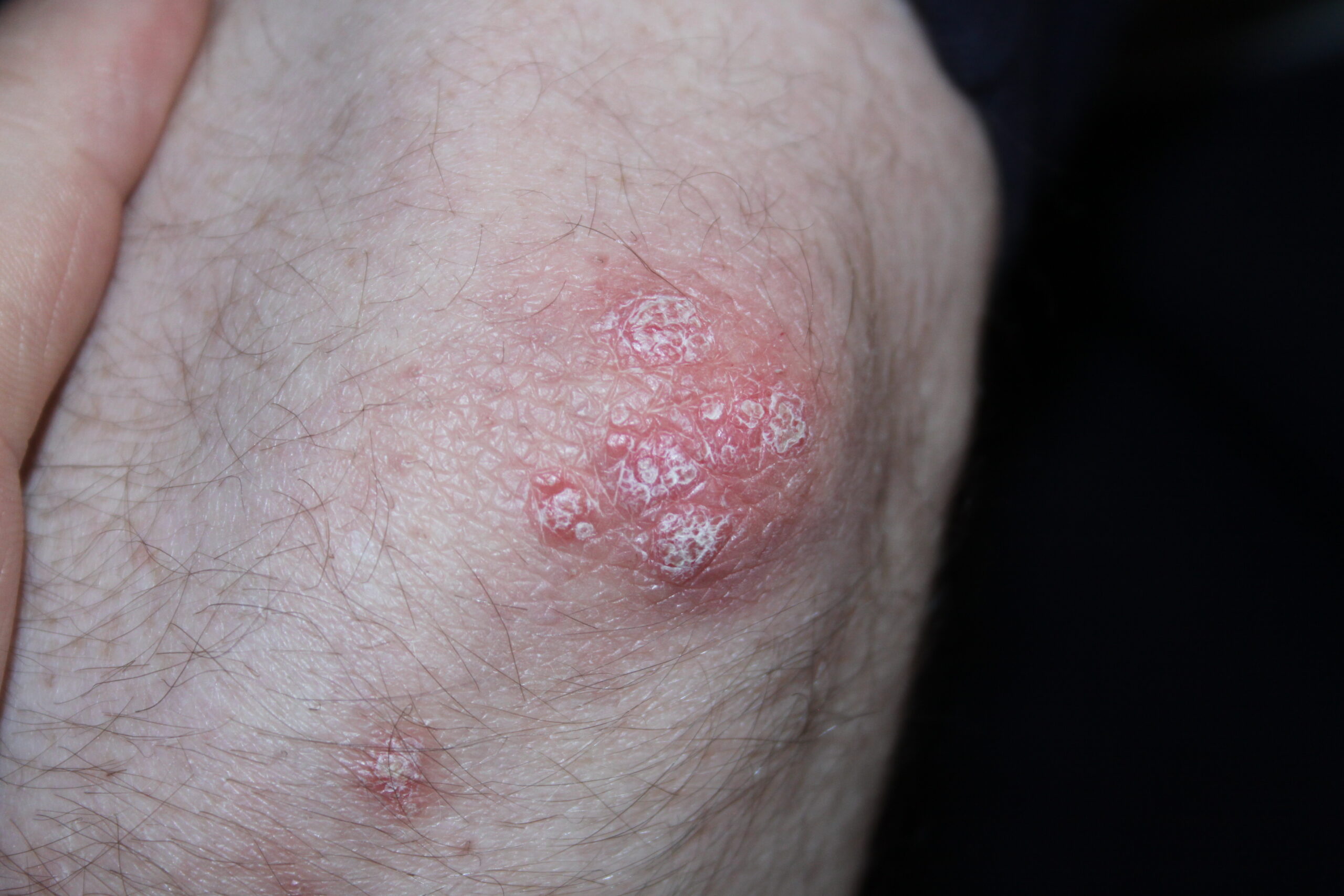
DITRA syndrome is associated with a mutation in which of the following?
Munro's microabscesses are typically seen in which layer of the epidermis?
Chloroquine can cause exacerbation of which of the following conditions?
Which of the following sites is least commonly involved in psoriasis?
Which is the most malignant type of pustular psoriasis?
Ahritis mutilans is seen in which of the following conditions?
Auspitz sign is seen in which of the following conditions?
"Microabscess of Munro" is seen in which of the following conditions?
What is the appropriate treatment for an erythematous skin rash with multiple pus lakes in a pregnant woman?
Practice by Chapter
Pathophysiology of Psoriasis
Practice Questions
Psoriasis Vulgaris
Practice Questions
Guttate Psoriasis
Practice Questions
Erythrodermic Psoriasis
Practice Questions
Pustular Psoriasis
Practice Questions
Palmoplantar Psoriasis
Practice Questions
Nail Psoriasis
Practice Questions
Scalp Psoriasis
Practice Questions
Psoriatic Arthritis
Practice Questions
Topical Therapy for Psoriasis
Practice Questions
Systemic Therapy for Psoriasis
Practice Questions
Phototherapy and Biologics for Psoriasis
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
