Pediatric Dermatology — MCQs

On this page
All of the following result in endogenous pigmentation of teeth except?
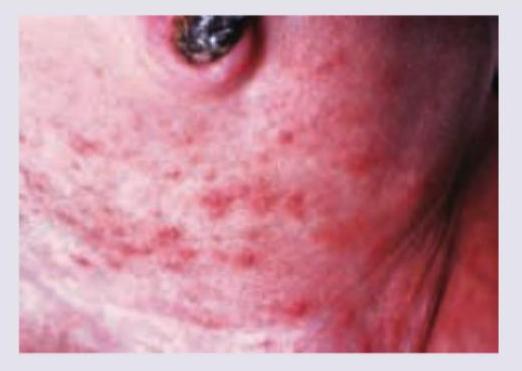
An adolescent boy complains of a splotchy red rash on the nape of his neck, discovered when he had his head shaved for football season. The rash seems to become more prominent with exercise or emotion. His mother notes that he has had the rash since infancy, but that it became invisible as hair grew. He had a similar rash on his eyelids that resolved in the newborn period. What is the most likely diagnosis?
Acrodermatitis enteropathica is inherited in which pattern?
What is true about Acrodermatitis enteropathica?
A child scratches their hand with a pen, resulting in a red wheal that persists for 30 minutes. What is the most likely diagnosis?
A child presents with a vesiculobullous, pustular rash around the mouth and on the extremities, along with alopecia and diarrhea. What is the most likely nutritional deficiency?
A neonate presents with a growing skin lesion, as shown in the image provided. The mother reports that the lesion has been increasing in size daily. What is the appropriate management?
A 6-month-old baby presents with a bright red, raised, soft nodule measuring 2 cm in diameter on the forehead. The lesion has well-defined borders, appeared 2 weeks after birth as a small red spot, and has been growing rapidly over the past few months. The surface has a characteristic strawberry-like appearance with a lobulated texture. What is the most likely diagnosis?
A neonate presents with blotchy rash on the abdomen as shown in the image. What is the diagnosis?
A 6-year-old child born to consanguinity has pallor and intolerance to sunlight. His urine was exposed to Wood's light. Probable diagnosis is:
Practice by Chapter
Neonatal Dermatology
Practice Questions
Infantile Hemangiomas and Vascular Malformations
Practice Questions
Atopic Dermatitis in Children
Practice Questions
Acne in Childhood and Adolescence
Practice Questions
Childhood Exanthems
Practice Questions
Genetic Skin Disorders in Children
Practice Questions
Genodermatoses
Practice Questions
Nutritional Dermatoses in Children
Practice Questions
Pigmentary Disorders in Children
Practice Questions
Hair Disorders in Children
Practice Questions
Child Abuse: Cutaneous Manifestations
Practice Questions
Therapeutic Considerations in Pediatric Dermatology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
