Pediatric Dermatology — MCQs

On this page
What is the dose of zinc used in acrodermatitis enteropathica?
Acrodermatitis enteropathica is characterized by all of the following, EXCEPT:
A 5-year-old boy with a history of atopy presents with multiple asymptomatic oval and circular faintly hypopigmented macules with fine scaling on his face. What is he suffering from?
Harlequin ichthyosis is inherited as?
Which of the following conditions disappear spontaneously in the first year of life?
Which of the following statements is NOT true about Sturge-Weber syndrome?
What is the treatment for impetigo herpetiformes in pregnancy?
These lesions are seen in which condition?
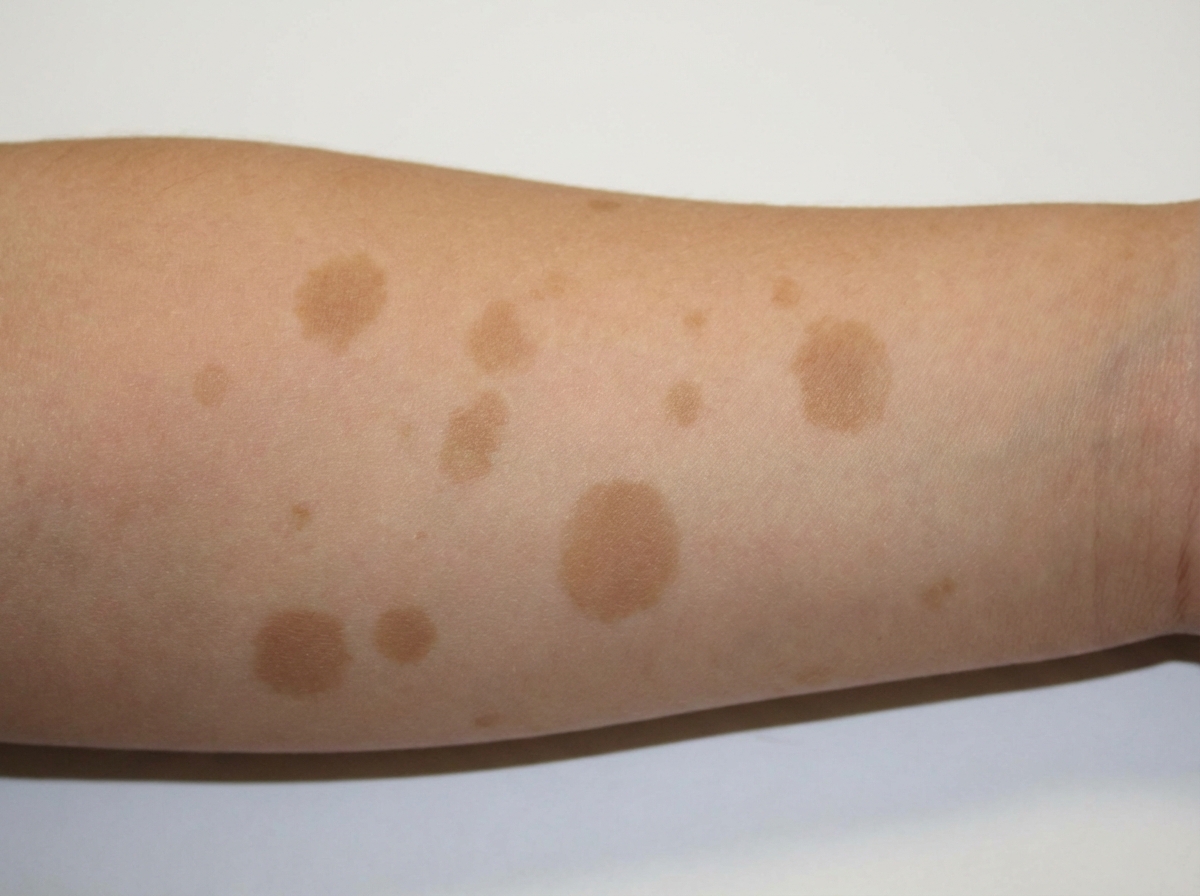
LEOPARD syndrome does not include which of the following?
Which of the following is NOT a feature of Neurofibromatosis-1?
Practice by Chapter
Neonatal Dermatology
Practice Questions
Infantile Hemangiomas and Vascular Malformations
Practice Questions
Atopic Dermatitis in Children
Practice Questions
Acne in Childhood and Adolescence
Practice Questions
Childhood Exanthems
Practice Questions
Genetic Skin Disorders in Children
Practice Questions
Genodermatoses
Practice Questions
Nutritional Dermatoses in Children
Practice Questions
Pigmentary Disorders in Children
Practice Questions
Hair Disorders in Children
Practice Questions
Child Abuse: Cutaneous Manifestations
Practice Questions
Therapeutic Considerations in Pediatric Dermatology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
