Antifungal Therapy — MCQs

What is the Drug of Choice (DOC) for Onychomycosis?
Which of the following is not a part of P. versicolor treatment -
Which of the following drugs are used topically for dermatophytes?
All the following drugs are effective in the treatment of Pityriasis Versicolor except:
Agents most effective and best tolerated in the management of onychomycosis?
Treatment of partner is required in all infections except -
What is the correct term for candidiasis of the penis?
A 70 year old farmer, presented to you with complaints of yellowish discolouration of his finger nails for the past 6 months, he also gives history of recurrent episodes of itching in the groin for which he used to take local home made herbal remedy. On examination 3 of his toe nails also show similar change with tunneling. Which among the following is the best test for rapid confirmation of your diagnosis?
A 30-year-old washerwoman presents with the following lesion. All are correct except:
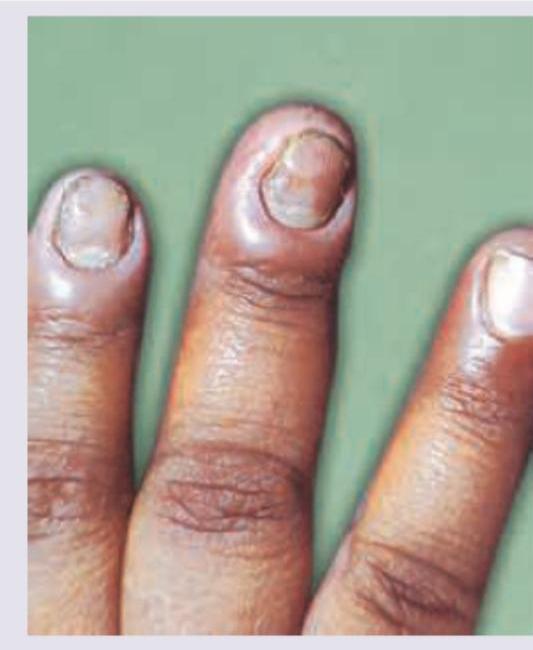
Skin scraping and KOH mounting is done for what condition?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
