Dermatitis and Eczema — MCQs

On this page
The Hanifin & Rajka diagnostic criteria are used for which condition?
A 17-year-old female presents with a pruritic rash localized to the wrist. Papules and vesicles are noted in a bandlike pattern, with slight oozing from some lesions. What is the most likely cause of this rash?
A 25-year-old male presents with recurrent episodes of flexural eczema, contact urticaria, recurrent skin infections, and severe abdominal cramps and diarrhea upon consuming seafood. What is the most likely diagnosis?
What is the characteristic presentation of erythematous lesions with collarettes of scales on the trunk?
An infant presented with erythematous lesions on the cheek and extensor aspect of the upper and lower limbs. There is a family history of asthma. What is the probable diagnosis?
Air-borne contact dermatitis can be diagnosed by?
A 35-year-old woman develops an itchy rash over her back, legs, and trunk several hours after swimming in a lake. Erythematous, edematous papules are noted. The wheals vary in size. There are no mucosal lesions and no swelling of the lips. What is the most likely diagnosis?
Multipleround to oval erythematous patches with fine central scale distributed along the skin tension lines on the trunk is highly suggestive of?
A 22-year-old woman developed small itchy wheals after physical exertion, walking in the sun, eating hot spicy food, and when she was angry. What is the most likely diagnosis?
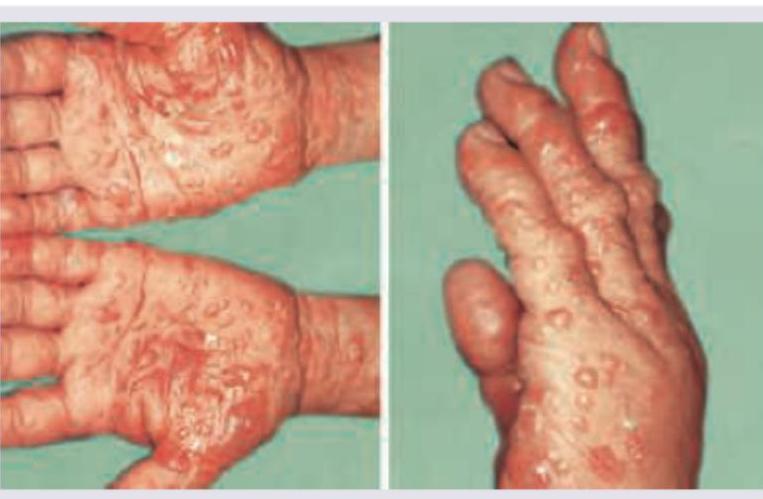
The following are true regarding the picture shown except:
Practice by Chapter
Atopic Dermatitis
Practice Questions
Seborrheic Dermatitis
Practice Questions
Contact Dermatitis: Irritant
Practice Questions
Contact Dermatitis: Allergic
Practice Questions
Nummular Eczema
Practice Questions
Dyshidrotic Eczema
Practice Questions
Stasis Dermatitis
Practice Questions
Asteatotic Eczema
Practice Questions
Lichen Simplex Chronicus
Practice Questions
Autoeczematization (Id Reaction)
Practice Questions
Photosensitive Eczemas
Practice Questions
Treatment Strategies for Eczematous Disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
