Dermatitis and Eczema — MCQs

On this page
What is the most likely cause of these skin changes?
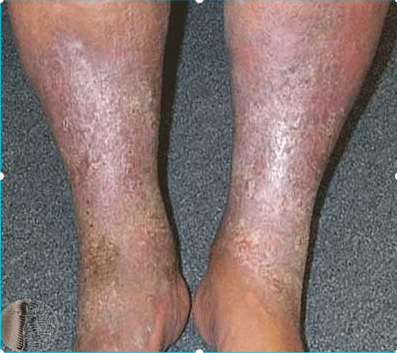
Pompholyx affects which area(s)?
All of the following are exogenous eczema except?
All are skin findings in atopic dermatitis, EXCEPT:
A 15-year-old healthy boy presents with pruritic, erythematous, blocky skin lesions on his arms, legs, and trunk that appear within an hour of consuming seafood. What is the most likely diagnosis?
Pityriasis rosea is best described as:
A 30-year-old male presents with pruritic, flat-topped, polygonal, shiny violaceous papules with flexural distribution. What is the most likely diagnosis?
A 27-year-old male presents with a 3-year history of itchy, excoriated papules on the forehead and exposed parts of the arms and legs. The condition is most severe during the rainy season and completely improves in winter. What is the most likely diagnosis?
What is the best initial treatment for acute contact dermatitis?
Which of the following causes allergic contact dermatitis through air?
Practice by Chapter
Atopic Dermatitis
Practice Questions
Seborrheic Dermatitis
Practice Questions
Contact Dermatitis: Irritant
Practice Questions
Contact Dermatitis: Allergic
Practice Questions
Nummular Eczema
Practice Questions
Dyshidrotic Eczema
Practice Questions
Stasis Dermatitis
Practice Questions
Asteatotic Eczema
Practice Questions
Lichen Simplex Chronicus
Practice Questions
Autoeczematization (Id Reaction)
Practice Questions
Photosensitive Eczemas
Practice Questions
Treatment Strategies for Eczematous Disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
