Blistering Diseases — MCQs

On this page
U-serrated pattern in direct immunofluorescence is seen in:
Acantholysis is characteristic of which of the following conditions?
In pemphigus, circulating antibodies attack which components?
All are true about Dermatitis herpetiformis EXCEPT:
Which of the following antigens are associated with cicatricial pemphigoid?
What percentage of skin involvement is characteristic of toxic epidermal necrolysis?
Intra-epithelial split is seen in which of the following conditions?
A 12-year-old male presented with intensely itchy grouped vesicles on the buttock, trunk, and scalp. On exposure to wheat, they exaggerate. What is the diagnosis?
Desmoplakin is the target antigen in which of the following conditions?
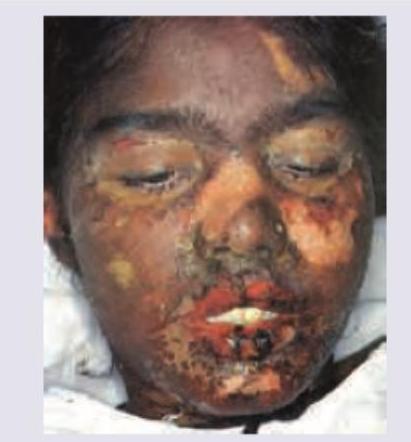
A 25-year-old office assistant in a multinational company was taking diclofenac sodium for low back ache for last few weeks. She presents with the following skin lesions. All are true about the image shown except:
Practice by Chapter
Pemphigus Vulgaris
Practice Questions
Pemphigus Foliaceus
Practice Questions
Bullous Pemphigoid
Practice Questions
Cicatricial Pemphigoid
Practice Questions
Dermatitis Herpetiformis
Practice Questions
Epidermolysis Bullosa
Practice Questions
Linear IgA Bullous Dermatosis
Practice Questions
Pemphigoid Gestationis
Practice Questions
Drug-Induced Bullous Disorders
Practice Questions
Immunofluorescence in Bullous Diseases
Practice Questions
Management of Autoimmune Bullous Diseases
Practice Questions
Genetic Counseling in Inherited Blistering Diseases
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
