Blistering Diseases — MCQs

On this page
Pemphigus vulgaris is caused by what type of process?
Which of the following presents with a "string of pearls appearance"?
Steven-Johnson syndrome involves which type of hypersensitivity reaction?
Prodromal symptoms precede 1 to 2 days before the onset of disease in which of the following conditions?
What is the commonest site of Herpes Gestationis?
Intraepidermal bullae are seen in which condition?
Which of the following is NOT a vesiculobullous lesion?
Which of the following drugs is not associated with drug-induced pemphigus?
Granular deposition of IgA at dermal papillae on immunofluorescence is seen in which condition?
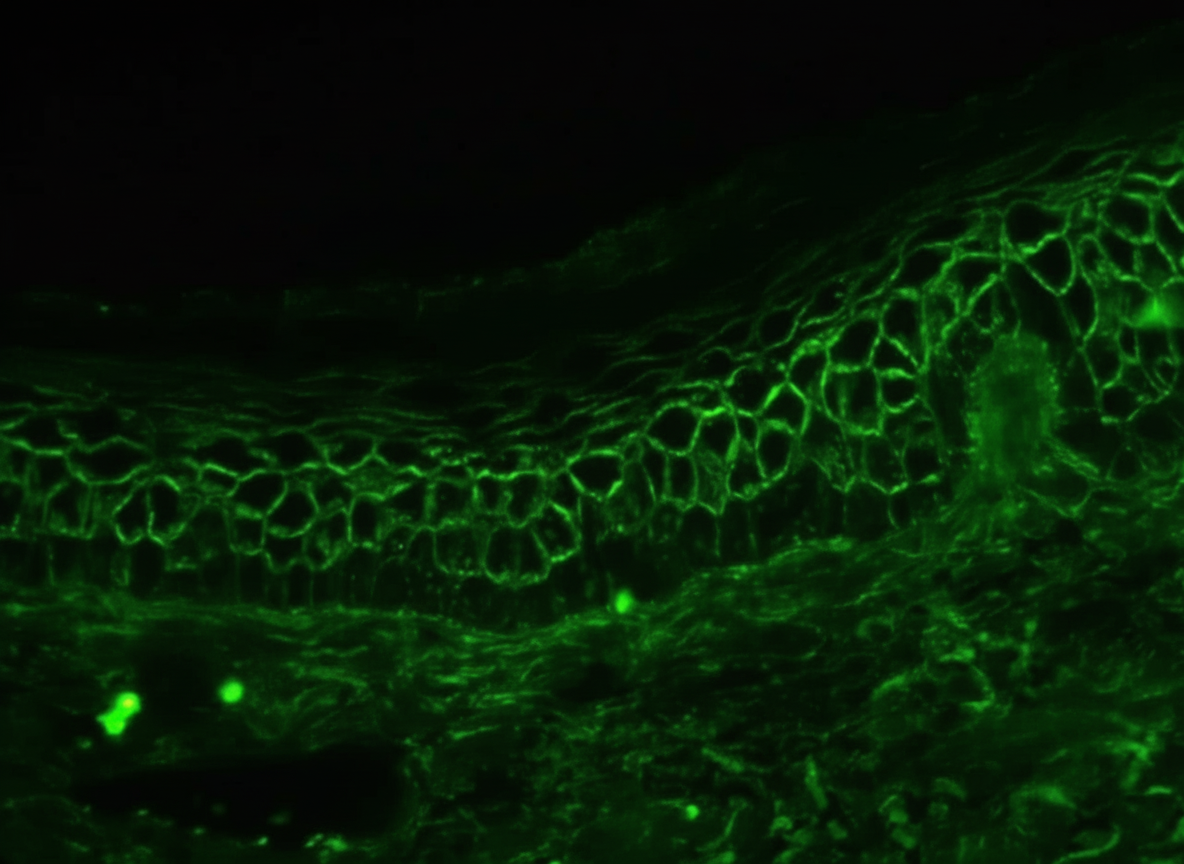
A 25-year-old man complains of eruptions of blisters on his scalp, inner surface of the groin, and in his mouth. The blisters rupture easily and leave large crusted areas. Histologically, the lesions show separation of the stratum spinosum from the basal layer. The results of direct immunofluorescence microscopy for IgG are shown. Which of the following proteins is targeted by IgG autoantibody in the skin of this patient?
Practice by Chapter
Pemphigus Vulgaris
Practice Questions
Pemphigus Foliaceus
Practice Questions
Bullous Pemphigoid
Practice Questions
Cicatricial Pemphigoid
Practice Questions
Dermatitis Herpetiformis
Practice Questions
Epidermolysis Bullosa
Practice Questions
Linear IgA Bullous Dermatosis
Practice Questions
Pemphigoid Gestationis
Practice Questions
Drug-Induced Bullous Disorders
Practice Questions
Immunofluorescence in Bullous Diseases
Practice Questions
Management of Autoimmune Bullous Diseases
Practice Questions
Genetic Counseling in Inherited Blistering Diseases
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
