Autoimmune Skin Diseases — MCQs

On this page
Localized scleroderma is also known as?
Gottron's papules are characteristically found on which of the following locations?
Which of the following is NOT true about Behçet's disease?
A butterfly rash characteristically spares which of the following facial areas?
"En coup de sabre" is seen in:
What is true about Dermatomyositis?
Exposure to sunlight can precipitate which of the following conditions?
A patient presents with a pruritic lesion over the left shoulder exhibiting cigarette paper atrophy and poikiloderma, along with generalized lymphadenopathy. Histopathological examination of the lesion reveals CD4-positive Sézary-Lutzner cells. What is the characteristic dermo-epidermal manifestation of this disease?
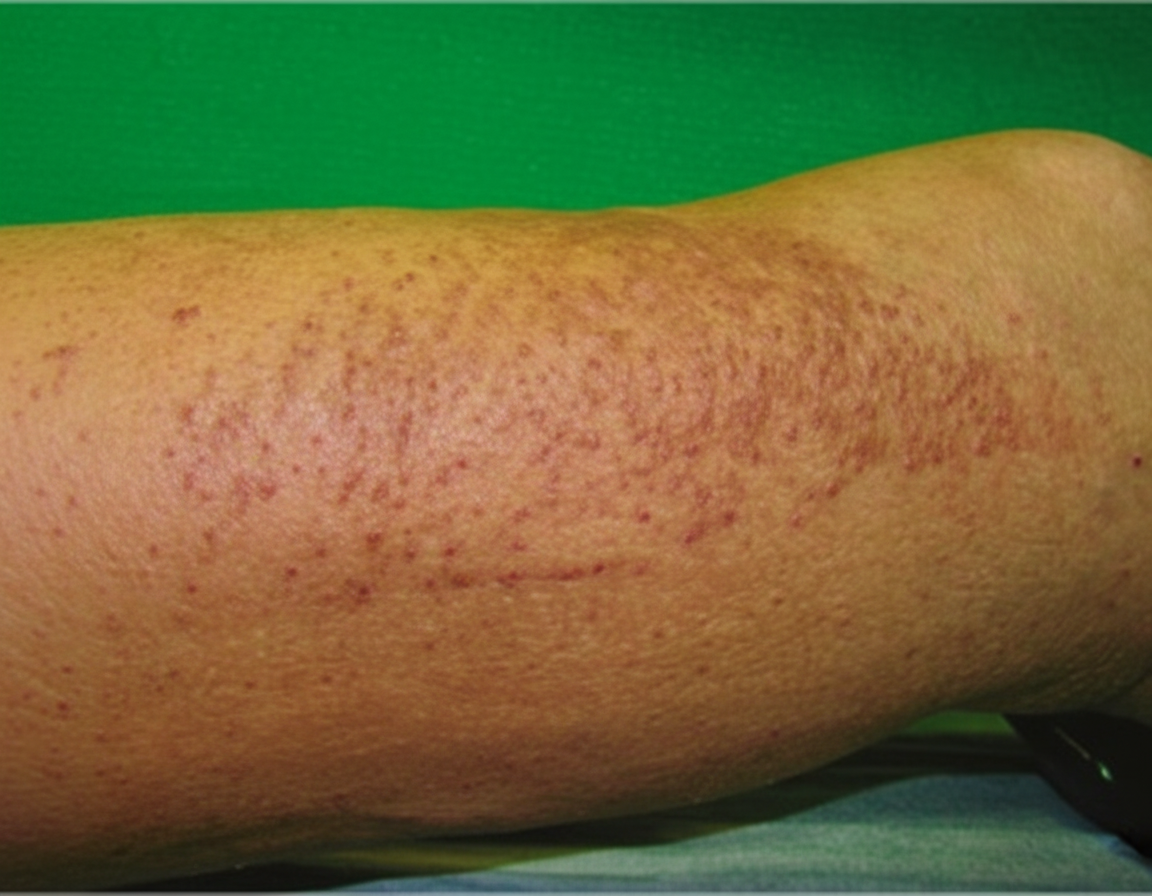
These skin changes developed during treatment for end-stage renal failure. What is the diagnosis?
A 23-year-old male complains of recurrent scaly lesions on the glans penis. The lesions always occurred at the same site and healed with slight hyperpigmentation. What is the most likely diagnosis?
Practice by Chapter
Lupus Erythematosus: Cutaneous Forms
Practice Questions
Lupus Erythematosus: Systemic with Skin Manifestations
Practice Questions
Dermatomyositis
Practice Questions
Scleroderma and Morphea
Practice Questions
Mixed Connective Tissue Disease
Practice Questions
Sjögren's Syndrome: Cutaneous Manifestations
Practice Questions
Relapsing Polychondritis
Practice Questions
Autoimmune Thyroid Disease and the Skin
Practice Questions
Immunobullous Disorders
Practice Questions
Vasculitis
Practice Questions
Diagnostic Methods in Autoimmune Dermatoses
Practice Questions
Management of Autoimmune Skin Diseases
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
