Biostatistics — MCQs

On this page
Which scale is used for classifying data that lacks a particular structure and is presented without inherent order?
The median weight of 100 children was 16 kgs. The standard deviation was 8. Calculate the percentage coefficient of variance.
In a cohort study of 7000 smokers over ten years, 70 developed lung cancer. In a concurrent evaluation of 7000 non-smokers in the same catchment area, 7 developed lung cancer. What is the Relative Risk (RR) for developing lung cancer?
The "Crude death rate" is defined as the number of deaths (from all causes) per 1000 estimated what?
Type 1 Sampling error is classified as?
A village is divided into five relevant subgroups for the purpose of a survey. Individuals from each subgroup are then selected randomly. What is this type of sampling called?
A chi-square test would be most appropriate for testing which one of the following hypotheses?
What is true about the standard normal distribution?
What is the definition of neonatal mortality?
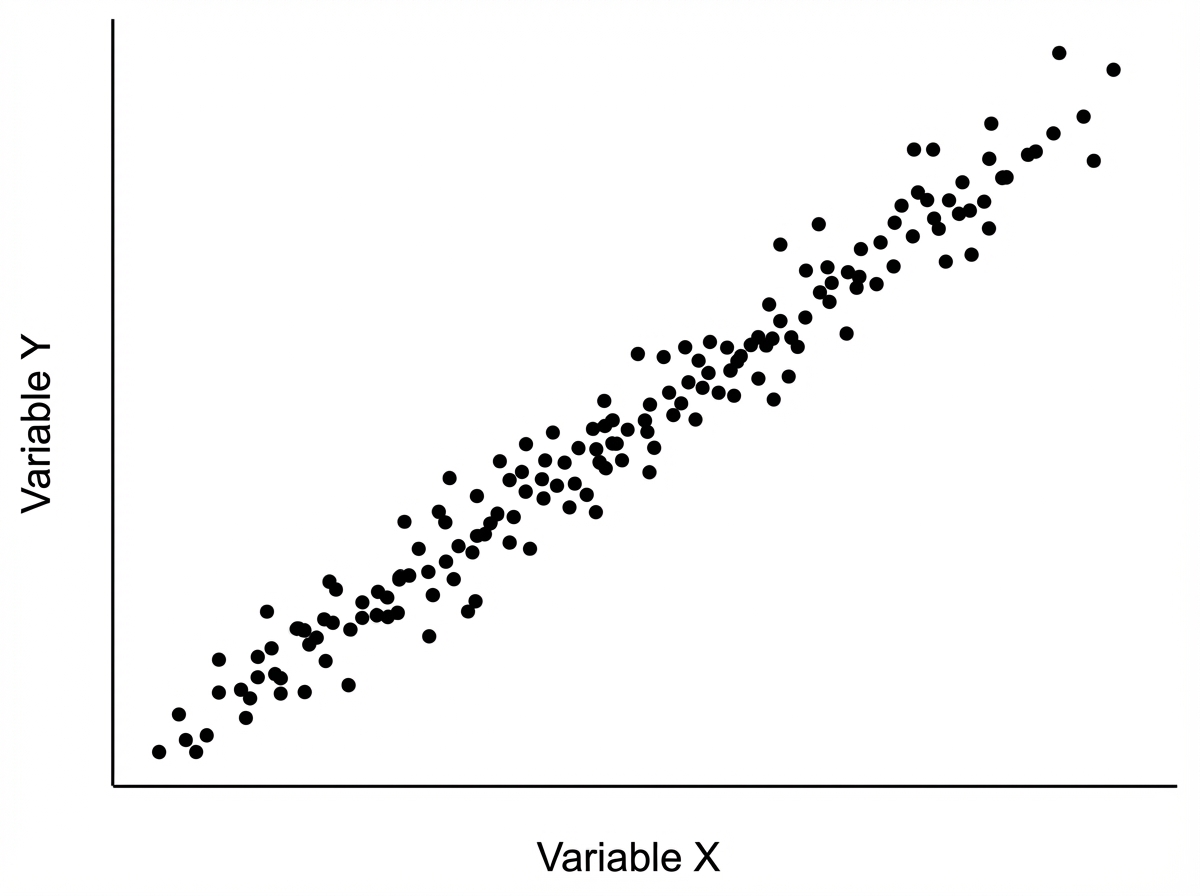
Interpret the statistical graph shown below:
Practice by Chapter
Collection and Presentation of Data
Practice Questions
Measures of Central Tendency
Practice Questions
Measures of Dispersion
Practice Questions
Normal Distribution
Practice Questions
Sampling Methods
Practice Questions
Sample Size Calculation
Practice Questions
Hypothesis Testing
Practice Questions
Tests of Significance
Practice Questions
Correlation and Regression
Practice Questions
Survival Analysis
Practice Questions
Multivariate Analysis
Practice Questions
Statistical Software in Research
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
