Genetic Disorders and Biochemical Pathology — MCQs

On this page
Find the type of inheritance?
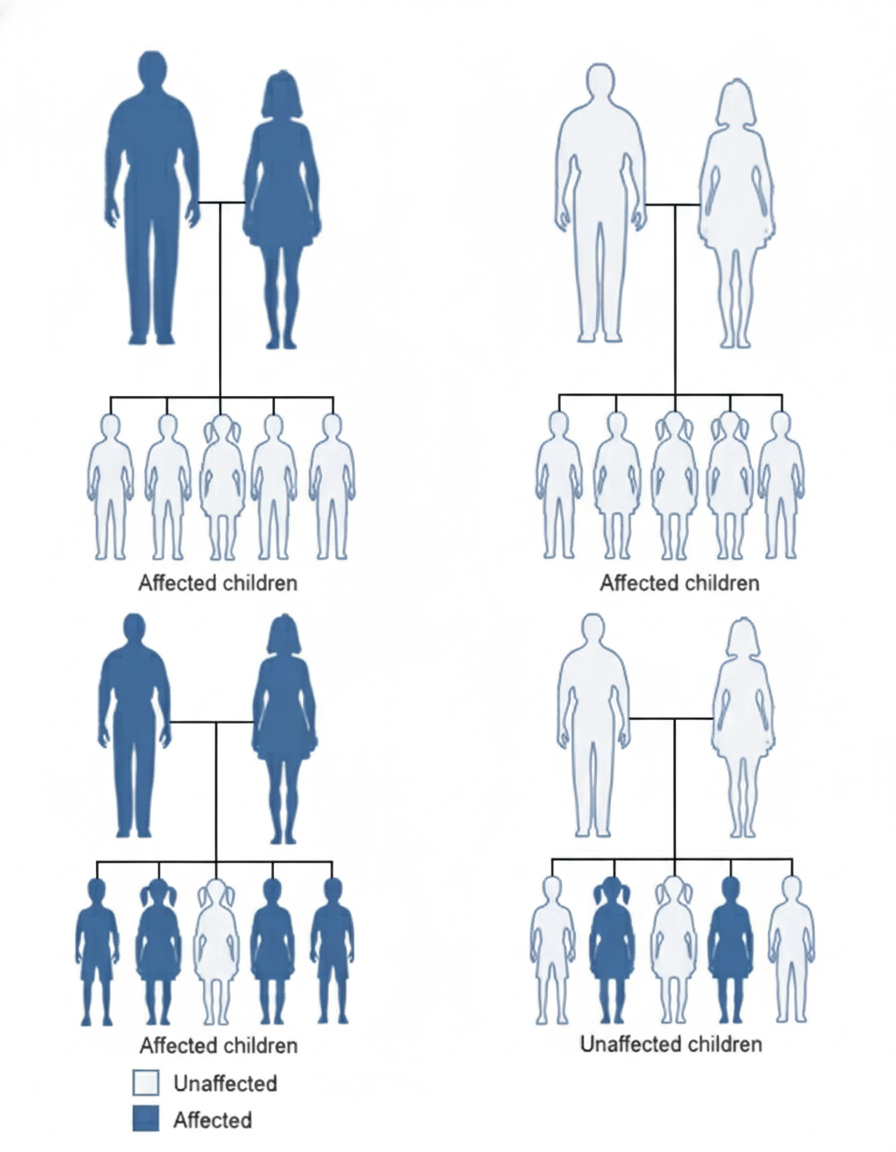
Which enzyme defect causes phenylketonuria?
Which enzyme deficiency leads to Pompe's disease?
Enzyme replacement therapy is available for which of the following conditions?
Which of the following is FALSE regarding hereditary fructose intolerance?
Cirrhosis can be seen in all of the following metabolic diseases EXCEPT?
Which of the following statements about mitochondrial disorders is FALSE?
McArdle disease is caused by a deficiency in the metabolism of which particular compound?
Which of the following conditions does not involve the skin?
An infant presents with hepatosplenomegaly, hypoglycemia, hyperuricemia, and lactic acidosis. Liver biopsy shows normal structured glycogen deposition. Which enzyme is deficient in this infant?
Practice by Chapter
Single Gene Disorders
Practice Questions
Biochemical Diagnosis of Genetic Disorders
Practice Questions
Inborn Errors of Metabolism
Practice Questions
Lysosomal Storage Diseases
Practice Questions
Glycogen Storage Diseases
Practice Questions
Disorders of Lipoprotein Metabolism
Practice Questions
Disorders of Purine and Pyrimidine Metabolism
Practice Questions
Hemoglobinopathies
Practice Questions
Porphyrias
Practice Questions
Biochemical Markers for Disease Diagnosis
Practice Questions
Newborn Screening for Genetic Disorders
Practice Questions
Enzyme Replacement Therapy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
