Respiratory and Airway Management — MCQs

On this page
What is the standard method used to differentiate between endotracheal and esophageal intubation?
In which of the following scenarios is the laryngeal mask airway (LMA) typically not used?
Which of the following systems is specifically designed to produce Positive End-Expiratory Pressure (PEEP) in mechanical ventilation?
The laryngeal mask airway is used for securing the airway in all of the following conditions, EXCEPT:
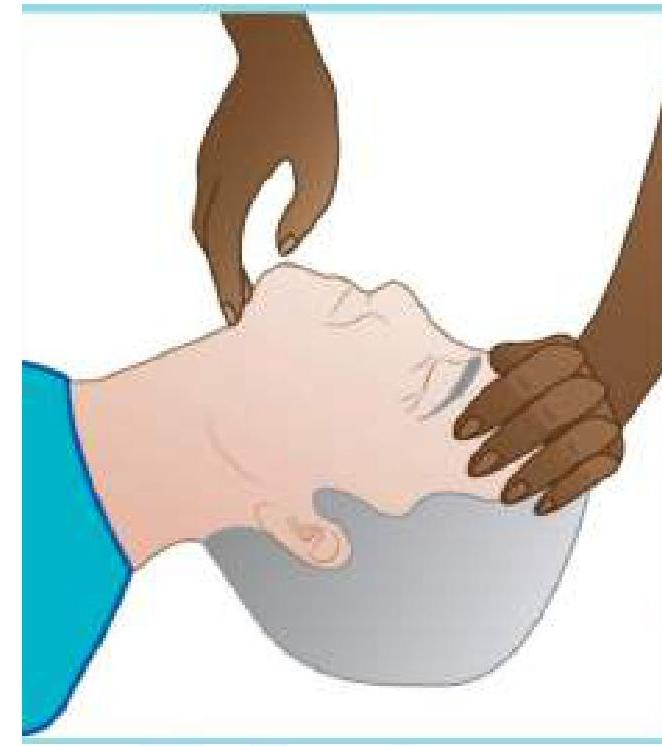
Identify the maneuver being performed.
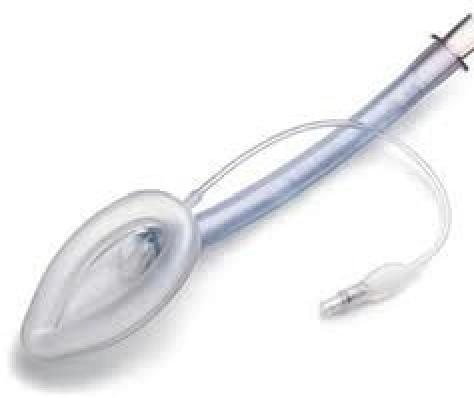
Identify the airway device shown in the image.
What percentage of oxygen is provided to a victim during mouth-to-mouth respiration?
Laryngeal mask airway [LMA] is contraindicated in?
What is the most reliable indicator to prevent esophageal intubation?
Difficult intubation is anticipated in all except the following conditions.
Practice by Chapter
Respiratory Physiology
Practice Questions
Airway Anatomy
Practice Questions
Preoxygenation Techniques
Practice Questions
Mask Ventilation
Practice Questions
Supraglottic Airway Devices
Practice Questions
Direct Laryngoscopy
Practice Questions
Video Laryngoscopy
Practice Questions
Fiberoptic Intubation
Practice Questions
Surgical Airway Management
Practice Questions
One-Lung Ventilation Techniques
Practice Questions
Ventilation Strategies During Anesthesia
Practice Questions
Extubation Criteria and Techniques
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
