Respiratory and Airway Management — MCQs

On this page
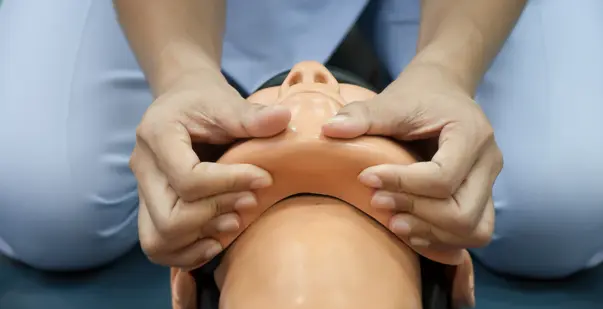
The procedure shown in the image is performed to maintain the airway. Which of the following techniques is being used?
In conventional oxygen therapy, which device will deliver the highest FiO2?
Endotracheal tube in the esophagus is best assessed by:
During rapid sequence intubation in a child after taking brief history and clinical examination next step is:
A patient is admitted following a road traffic accident. He has sustained significant blunt injury to his head, chest and abdomen and has a Glasgow Coma Scale score of 8/15. His saturations are poor at 89% on 15 L of oxygen a rebreathing mask. You note bruising around both eyes and blood-stained fluid issuing from his left ear, which forms concentric circles when dripped on a white sheet. You wish to support his airway to improve oxygenation. The first choice of airway adjunct would be
On doing laparoscopic cholecystectomy patient developed wheezing. Which of the following is used in the treatment?
Helium is used along with oxygen instead of plain oxygen because
A 70 kg young athlete was planned for surgery. During anesthesia, vecuronium was not available, so repeated doses of succinylcholine were given intermittently up to 640 mg. During recovery, the patient was not able to spontaneously respire and move limbs. What is the cause?
All of the following are advantages of LMA except:
Which of the following is an ideal method to prevent aspiration pneumonia?
Practice by Chapter
Respiratory Physiology
Practice Questions
Airway Anatomy
Practice Questions
Preoxygenation Techniques
Practice Questions
Mask Ventilation
Practice Questions
Supraglottic Airway Devices
Practice Questions
Direct Laryngoscopy
Practice Questions
Video Laryngoscopy
Practice Questions
Fiberoptic Intubation
Practice Questions
Surgical Airway Management
Practice Questions
One-Lung Ventilation Techniques
Practice Questions
Ventilation Strategies During Anesthesia
Practice Questions
Extubation Criteria and Techniques
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
