Respiratory and Airway Management — MCQs

On this page
A construction worker met with an accident when a cement block fell on his face. He sustained severe maxillofacial and laryngeal injury. He was not able to open his mouth and is having jaw fracture with obstruction in nasopharynx and oropharynx. To stabilize his airway, the following procedure was done on him. Which option describes the procedure done on him?
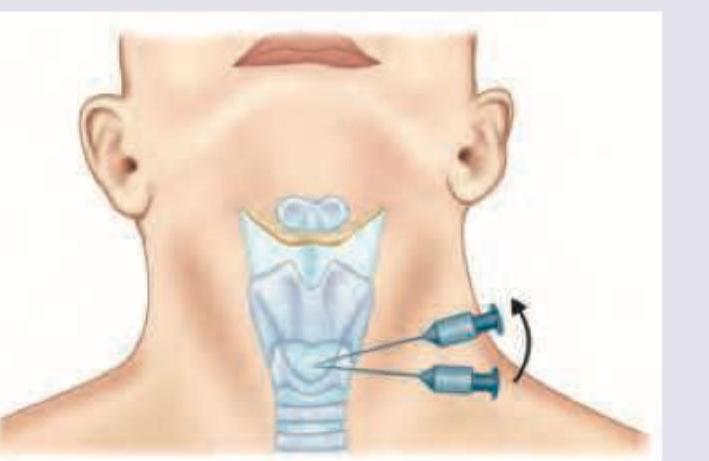
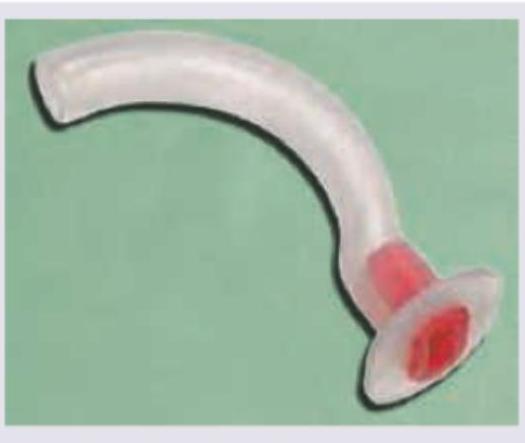
The equipment shown below is used for:
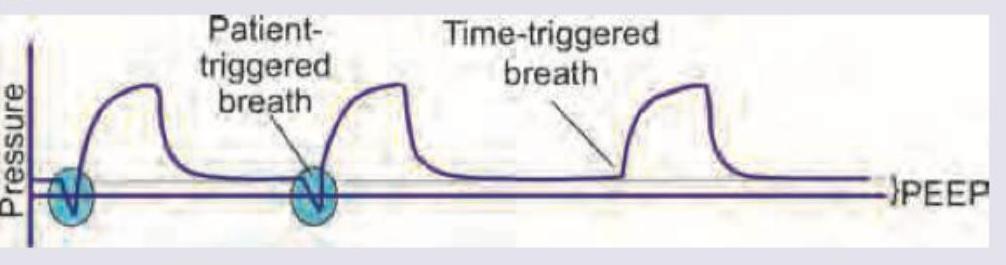
What is the mode of ventilation shown here?
The following ventilation modality is used in:
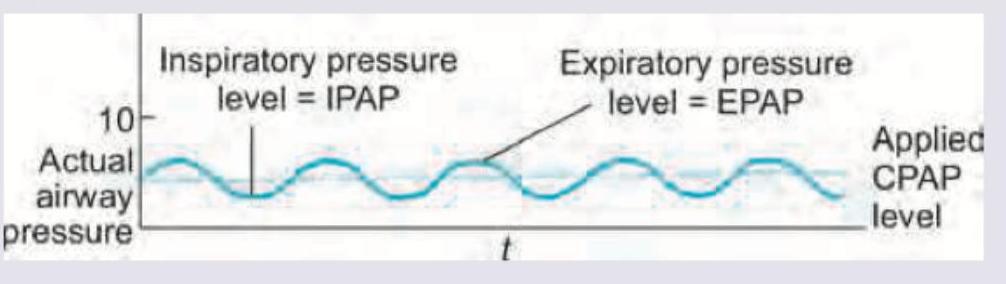
What ventilation modality is shown below?
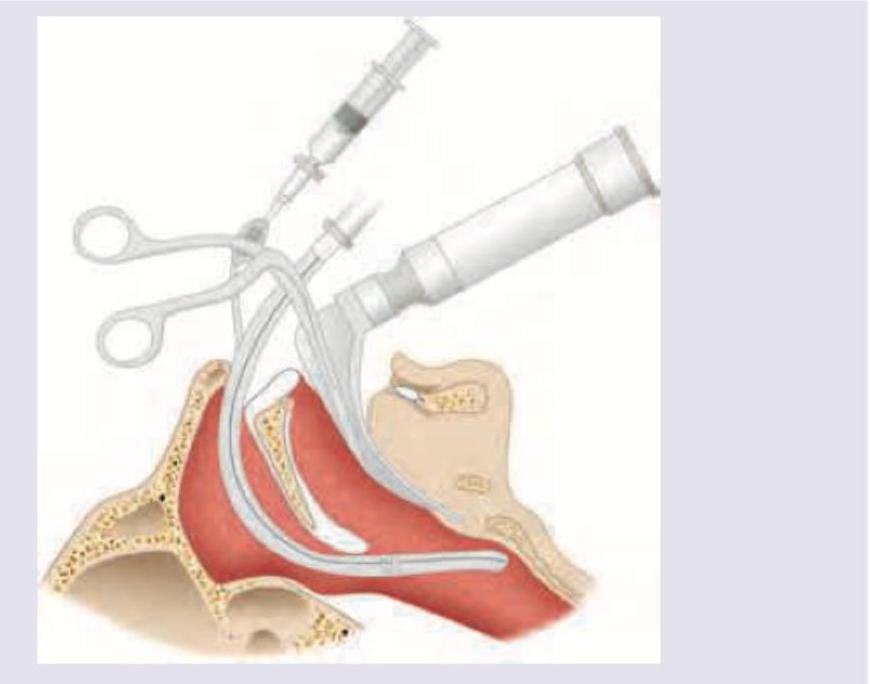
(1) Name the forceps being used in the procedure being performed:
Mallampati test is used for the assessment of :
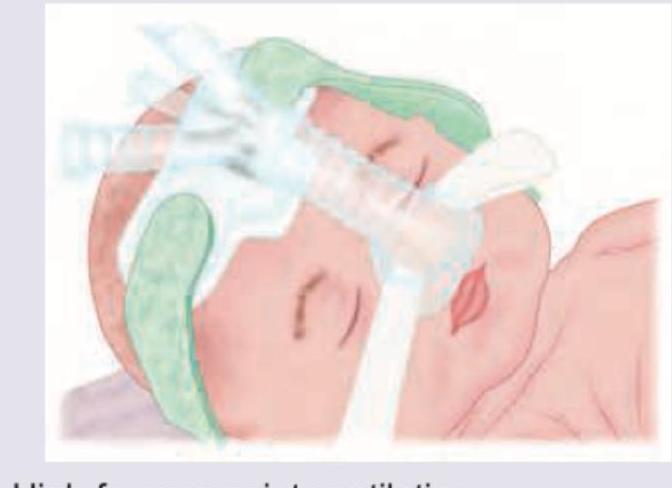
Which of the following conditions are contraindications for noninvasive positive-pressure ventilation in patients with respiratory failure? I. Craniofacial abnormalities II. Significant burns III. Respiratory failure with PaCO_2 of 60 mm Hg IV. Cardiovascular instability Select the correct answer using the code given below :
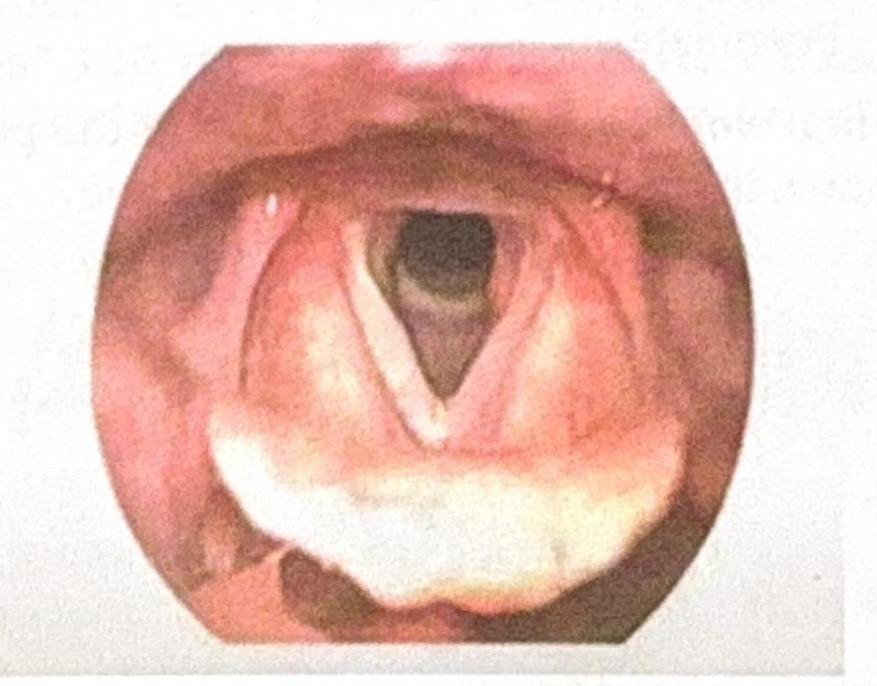
What is the staging system used for the condition seen in the patient after a history of intubation, as shown in the image?
What is the purpose of Positive End-Expiratory Pressure (PEEP)?
Practice by Chapter
Respiratory Physiology
Practice Questions
Airway Anatomy
Practice Questions
Preoxygenation Techniques
Practice Questions
Mask Ventilation
Practice Questions
Supraglottic Airway Devices
Practice Questions
Direct Laryngoscopy
Practice Questions
Video Laryngoscopy
Practice Questions
Fiberoptic Intubation
Practice Questions
Surgical Airway Management
Practice Questions
One-Lung Ventilation Techniques
Practice Questions
Ventilation Strategies During Anesthesia
Practice Questions
Extubation Criteria and Techniques
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
