Respiratory and Airway Management — MCQs

On this page
A patient under anesthesia is found to be in a “cannot intubate, cannot ventilate” (CICV) scenario. What is the next best step in management?
A patient undergoing general anesthesia develops left lung collapse following intubation. On auscultation, breath sounds are heard only on the right side. What is the most likely cause of this condition?
A patient in the ICU with an endotracheal tube now needs a tracheostomy tube. Which type of tube will you use?
Which of the following airway devices helps maintain Fio2 of 0.25-0.60, irrespective of the patient's breathing effort?
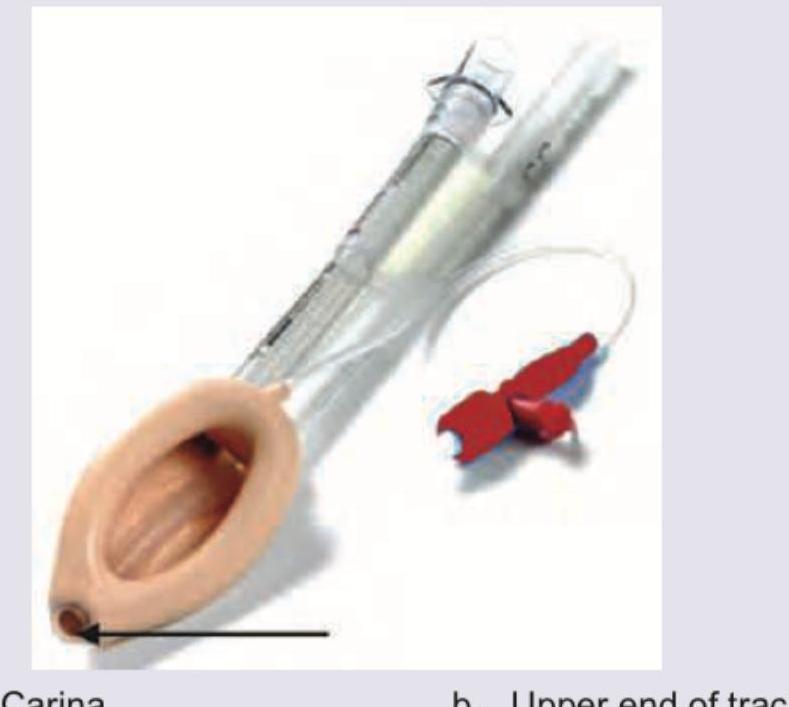
The diagram of a correctly positioned proseal-type Laryngeal Mask Airway is provided below. Above what site is the arrow marked area of the airway positioned?
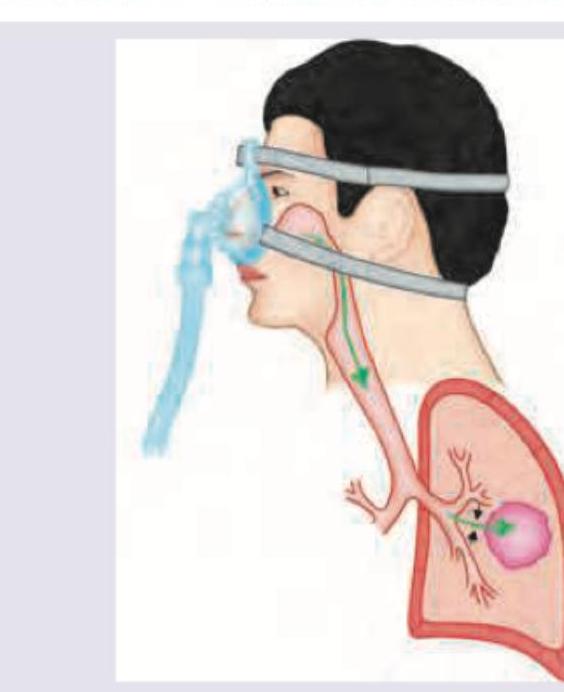
The mode of ventilation shown below is used for:
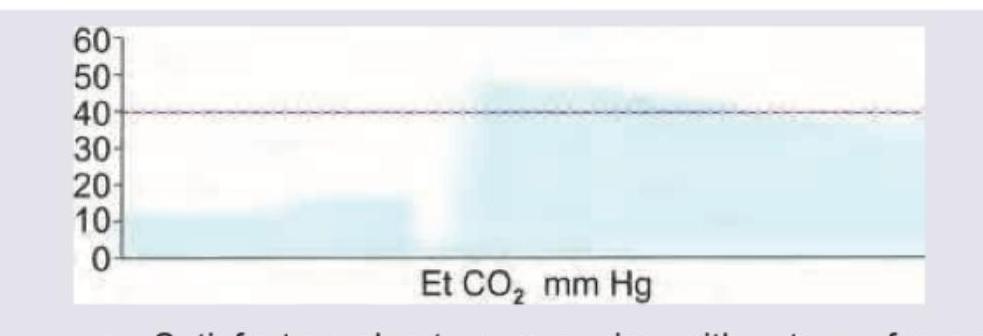
A young intern is managing a patient of Acute MI who developed cardiac arrest when thrombolysis was initiated. The patient was intubated, CPR was performed and one ampoule of adrenaline was given. The capnographic tracing indicates:
The following capnographic tracing represents:
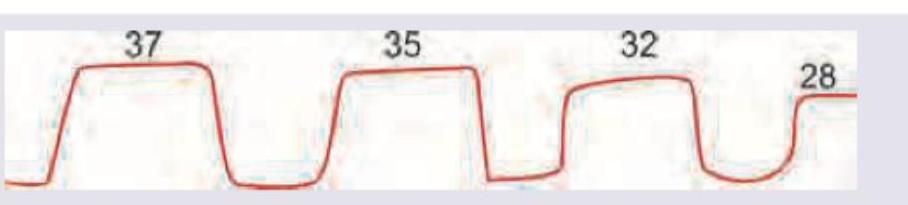
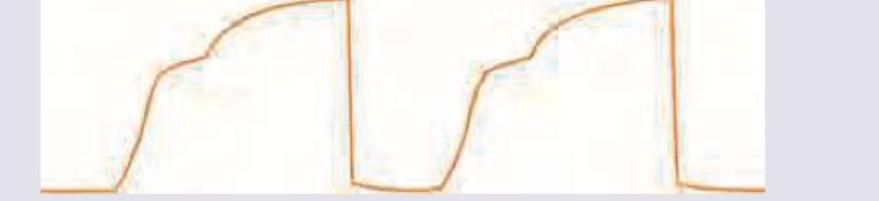
The following capnographic tracing represents:
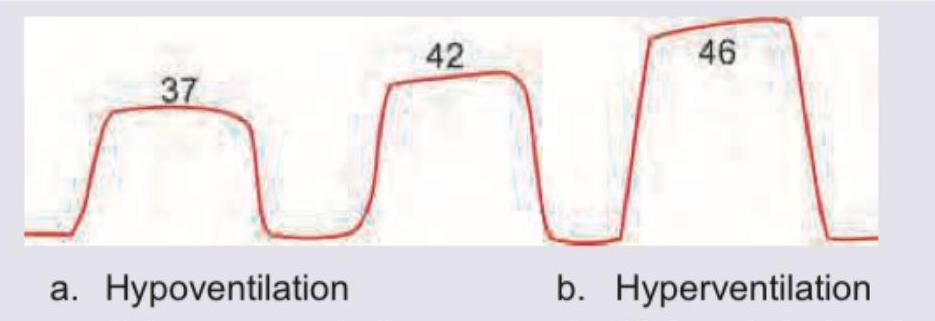
The interpretation for the following capnography is:
Practice by Chapter
Respiratory Physiology
Practice Questions
Airway Anatomy
Practice Questions
Preoxygenation Techniques
Practice Questions
Mask Ventilation
Practice Questions
Supraglottic Airway Devices
Practice Questions
Direct Laryngoscopy
Practice Questions
Video Laryngoscopy
Practice Questions
Fiberoptic Intubation
Practice Questions
Surgical Airway Management
Practice Questions
One-Lung Ventilation Techniques
Practice Questions
Ventilation Strategies During Anesthesia
Practice Questions
Extubation Criteria and Techniques
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
