Respiratory and Airway Management — MCQs

On this page
What is true about a laryngeal mask airway?
In tracheotomy, what is the typical reduction in dead space?
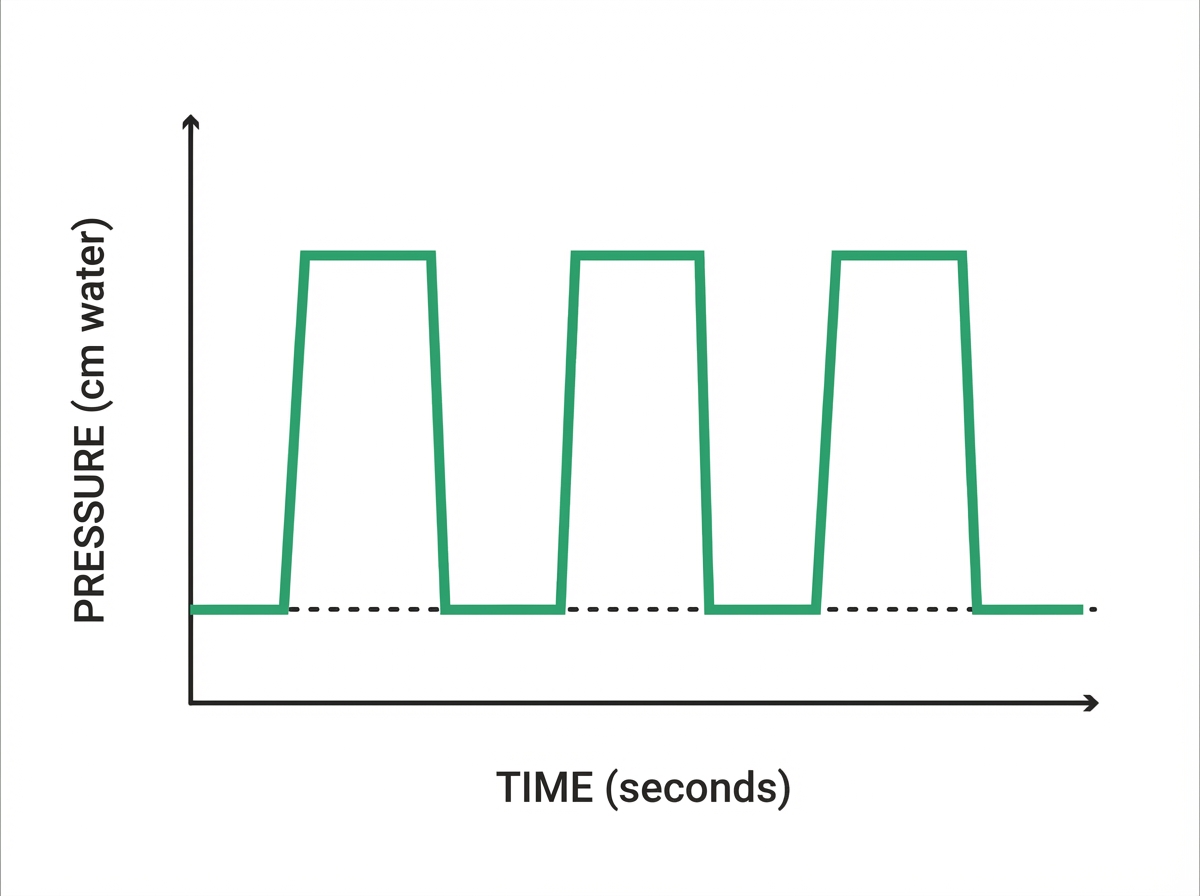
What mode of ventilation is characterized by the pressure-time graph shown?
A throat pack is primarily used for which of the following purposes?
Which laryngoscope is particularly used for pediatric intubation?
A patient with a known history of systemic sclerosis is scheduled for hernioplasty. During pre-operative assessment, the anesthesiologist anticipates difficult intubation based on oral examination findings. Upon laryngoscopy, only the posterior glottis is visible. What is the laryngoscopic grading of the glottis?
Fink's effect is?
What is the commonest sign of aspiration pneumonitis?
Nasal intubation is contraindicated in which of the following conditions?
What is the primary use of a laryngeal mask airway?
Practice by Chapter
Respiratory Physiology
Practice Questions
Airway Anatomy
Practice Questions
Preoxygenation Techniques
Practice Questions
Mask Ventilation
Practice Questions
Supraglottic Airway Devices
Practice Questions
Direct Laryngoscopy
Practice Questions
Video Laryngoscopy
Practice Questions
Fiberoptic Intubation
Practice Questions
Surgical Airway Management
Practice Questions
One-Lung Ventilation Techniques
Practice Questions
Ventilation Strategies During Anesthesia
Practice Questions
Extubation Criteria and Techniques
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
