Respiratory and Airway Management — MCQs

On this page
Which of the following anesthetic agents is known to cause tachypnoea?
In volume-cycled ventilation, what is the typical inspiratory flow rate set at?
What is true about endotracheal intubation?
What is the name of the test performed before drawing an arterial blood gas sample?
Which of the following is contraindicated during this procedure?
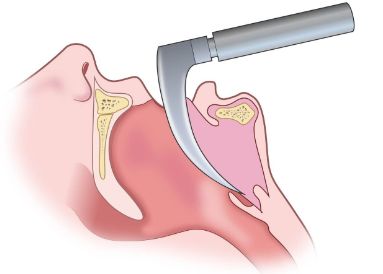
Which anesthetic induction agent is contraindicated in a patient with asthma?
What is the gold standard for confirming the placement of an endotracheal tube?
In anesthetizing the lower anteriors, all of the following techniques are indicated except?
Which intravenous anesthetic agent should be avoided in a patient with bronchoconstriction?
What is a contraindication for nasotracheal intubation?
Practice by Chapter
Respiratory Physiology
Practice Questions
Airway Anatomy
Practice Questions
Preoxygenation Techniques
Practice Questions
Mask Ventilation
Practice Questions
Supraglottic Airway Devices
Practice Questions
Direct Laryngoscopy
Practice Questions
Video Laryngoscopy
Practice Questions
Fiberoptic Intubation
Practice Questions
Surgical Airway Management
Practice Questions
One-Lung Ventilation Techniques
Practice Questions
Ventilation Strategies During Anesthesia
Practice Questions
Extubation Criteria and Techniques
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
