Cardiovascular Anesthesia — MCQs

On this page
Which of the following is most cardiostable?
The best chances of recovery after successful cardiopulmonary resuscitation are seen in which cardiac rhythm?
According to the 2010 ACLS Guidelines by AHA, which of the following pharmacological agents is not used in the management of cardiac arrest?
A 40-year-old lady intraoperatively develops a heart rate of 220 bpm and a blood pressure of 70/40 mmHg. The ECG shows a QRS complex of 120 milliseconds. What is the best management?
What is the most common arrhythmia after sinus tachycardia in an ICU patient?
During the surgical removal of an invasive glioma from the base of the skull, cranial nerves IX and X are accidentally cut bilaterally. What would be the immediate change in the patient's hemodynamic condition?
What is the vasopressor of choice in anesthesia for a patient with aortic stenosis who develops hypotension during surgery?
All of the following are indicated in the management of a patient with the given ECG findings, except?
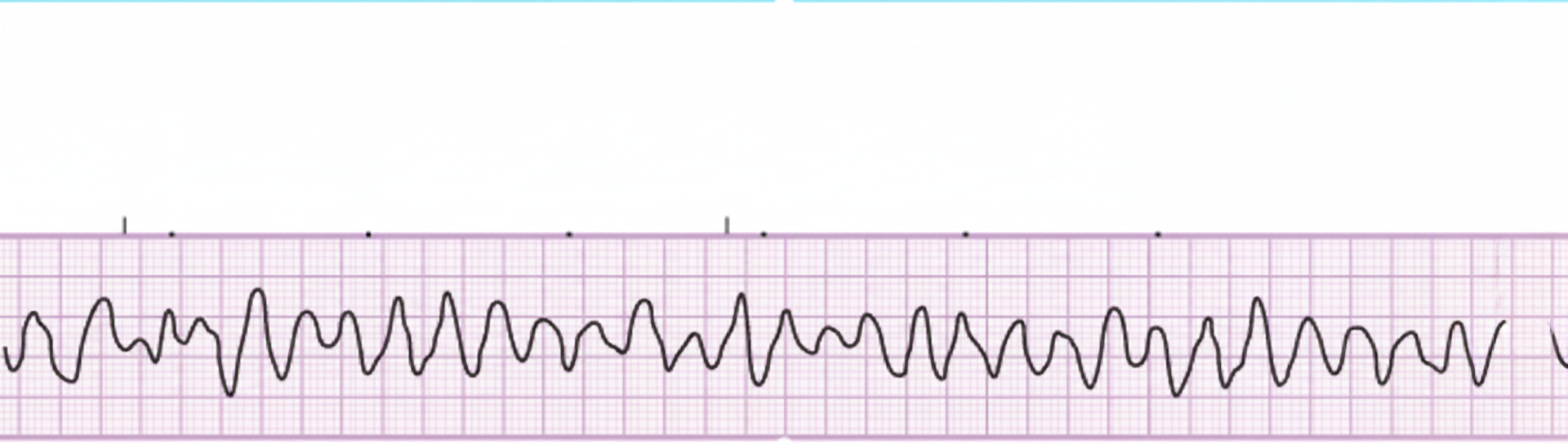
After effective cardiopulmonary resuscitation, what physiological change is observed?
What is the anesthetic of choice for cardiac anesthesia?
Practice by Chapter
Cardiovascular Physiology
Practice Questions
Anesthesia for Coronary Artery Disease
Practice Questions
Valvular Heart Disease Management
Practice Questions
Congenital Heart Disease in Adults
Practice Questions
Cardiopulmonary Bypass Principles
Practice Questions
Myocardial Protection Strategies
Practice Questions
Inotropes and Vasopressors
Practice Questions
Vasodilators in Cardiac Anesthesia
Practice Questions
Transesophageal Echocardiography
Practice Questions
Off-Pump Cardiac Surgery
Practice Questions
Management of Cardiac Pacemakers and ICDs
Practice Questions
Fast-Track Cardiac Anesthesia
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
