Anesthetic Equipment and Monitoring — MCQs

On this page
Vapour concentration in a breathing system is monitored by all except:
Regarding the oxygen flush valve, all of the following are true EXCEPT:
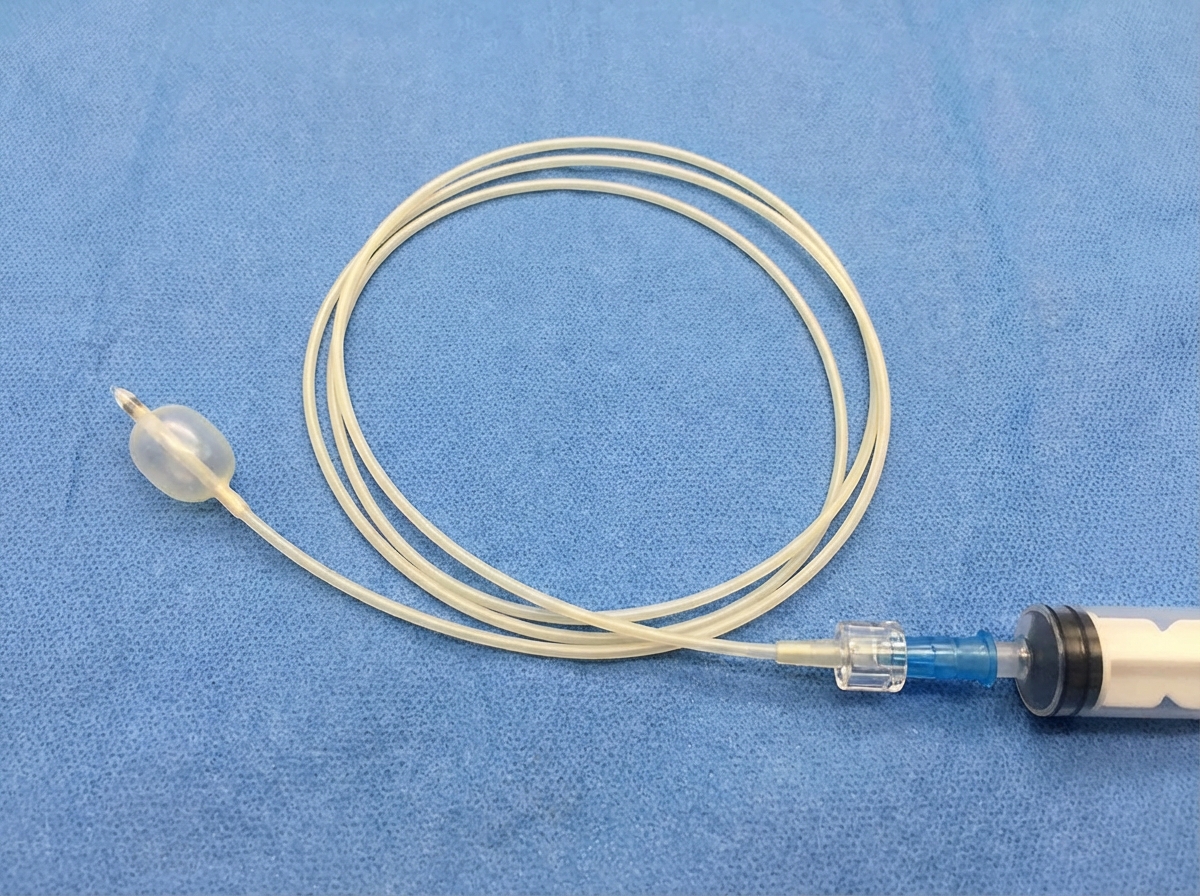
Which instrument is shown in the image?
Which of the following does NOT increase CO2 absorption in the anesthetic circuit?
Which of the following statements is true about Sevoflurane?
Which of the following will produce decreased EEG activity?
What does the partition coefficient of a gas measure?
Depth of anesthesia by inhalation anesthetics depends upon which of the following factors?
The 'train of four' is characteristically used in concern with which of the following?
Central line may be inserted in all of the following veins except?
Practice by Chapter
Anesthesia Machine Components
Practice Questions
Breathing Systems
Practice Questions
Vaporizers
Practice Questions
Gas Cylinders and Pipeline Supply
Practice Questions
Anesthesia Ventilators
Practice Questions
Standard Monitoring: ECG, BP, Pulse Oximetry
Practice Questions
Capnography
Practice Questions
Neuromuscular Monitoring
Practice Questions
Temperature Monitoring
Practice Questions
Invasive Hemodynamic Monitoring
Practice Questions
Equipment Troubleshooting
Practice Questions
Safety Features in Modern Anesthesia Equipment
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
