Anesthetic Equipment and Monitoring — MCQs

On this page
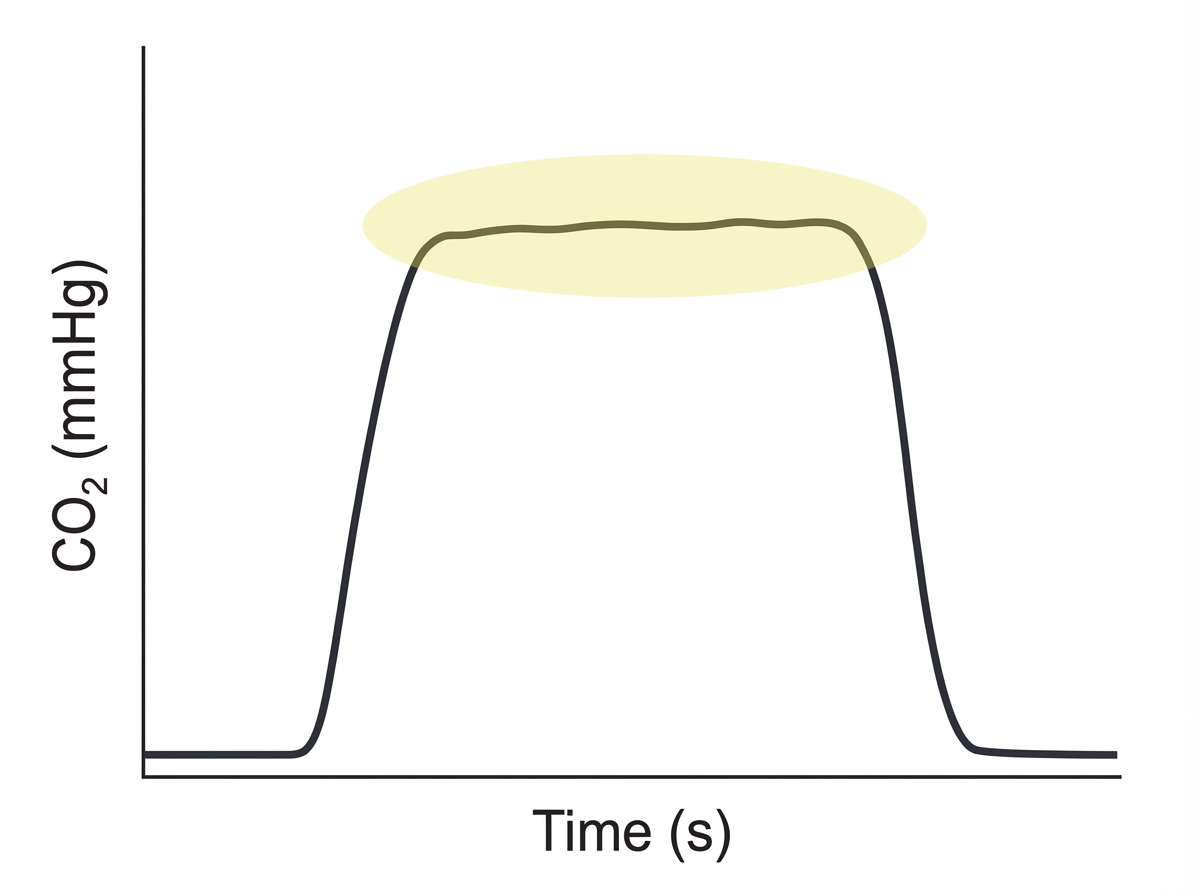
The circled part of the given capnograph reflects which of the following?
What is the standard color of an oxygen cylinder?
Minimum alveolar concentration is an indicator of?
Which of the following non-invasive methods is used in detecting the position of tubes during ventilation?
Veril's sign is seen in which condition?
Which of the following is NOT an intermediate-acting muscle relaxant?
All are constituents of soda lime except?
What is the purpose of nitrogen gas filled in an anesthetic cartridge?
Which muscle is most resistant to a non-depolarizing neuromuscular block?
What is true about Sugammadex?
Practice by Chapter
Anesthesia Machine Components
Practice Questions
Breathing Systems
Practice Questions
Vaporizers
Practice Questions
Gas Cylinders and Pipeline Supply
Practice Questions
Anesthesia Ventilators
Practice Questions
Standard Monitoring: ECG, BP, Pulse Oximetry
Practice Questions
Capnography
Practice Questions
Neuromuscular Monitoring
Practice Questions
Temperature Monitoring
Practice Questions
Invasive Hemodynamic Monitoring
Practice Questions
Equipment Troubleshooting
Practice Questions
Safety Features in Modern Anesthesia Equipment
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
