Anesthetic Equipment and Monitoring — MCQs

On this page
Which color Entonox gas cylinder should be ordered?
A 60-year-old female patient underwent modified radical mastectomy under general anesthesia. She is very anxious preoperatively. What monitor might the anesthetist have used during surgery to ensure she does not recall intraoperative events?
Laudanosine is a metabolite of which of the following neuromuscular blocking agents?
Which of the following statements are true about an N2O cylinder?
What is the diameter and length of the component marked with an arrow?
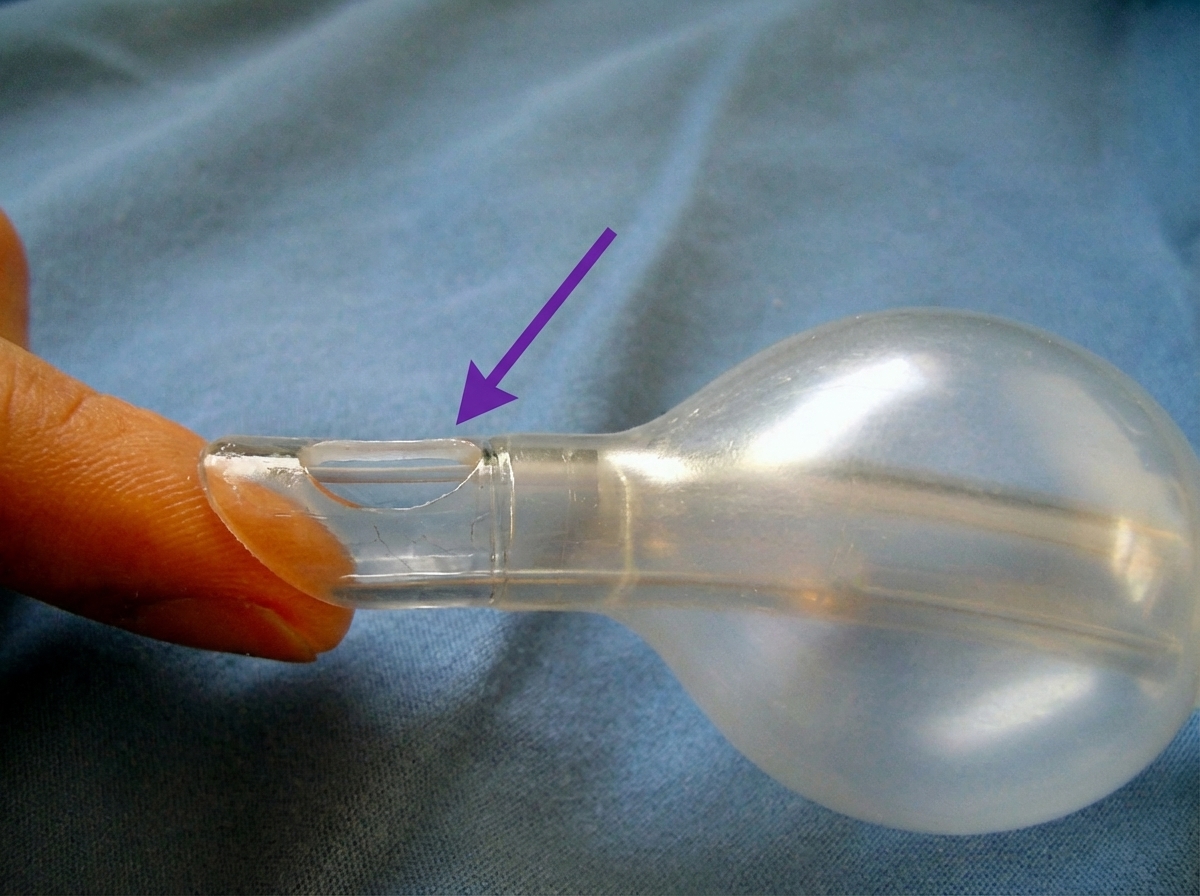
What is the amount of vasoconstrictor in 1 ml of 2% Lignocaine solution with 1:200,000 adrenaline?
Which anesthetic equipment can provide 100% oxygen?
Which pattern of capnograph is indicative of endotracheal tube obstruction?
Ayer's T Piece is classified as which of the following Mapelson circuits?
This type of flow-time graph is typically observed in which mechanical ventilator mode?
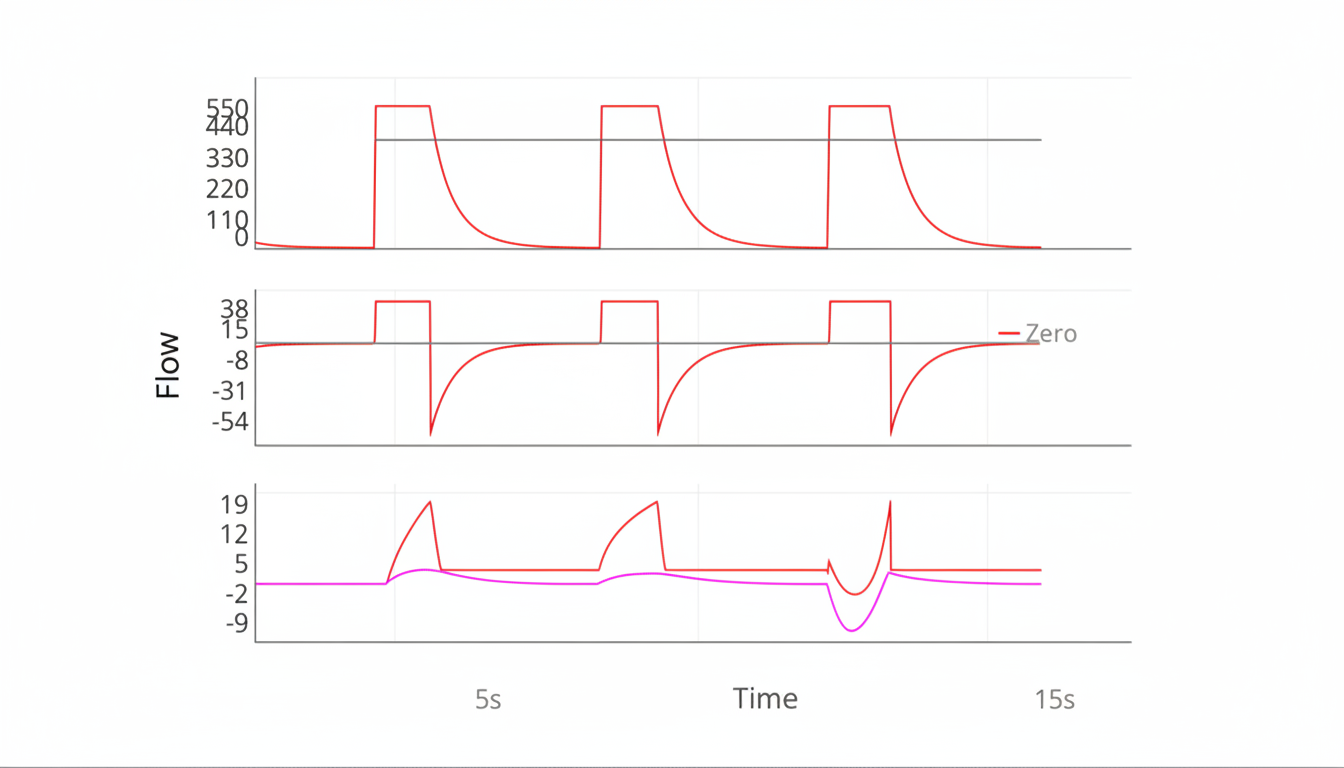
Practice by Chapter
Anesthesia Machine Components
Practice Questions
Breathing Systems
Practice Questions
Vaporizers
Practice Questions
Gas Cylinders and Pipeline Supply
Practice Questions
Anesthesia Ventilators
Practice Questions
Standard Monitoring: ECG, BP, Pulse Oximetry
Practice Questions
Capnography
Practice Questions
Neuromuscular Monitoring
Practice Questions
Temperature Monitoring
Practice Questions
Invasive Hemodynamic Monitoring
Practice Questions
Equipment Troubleshooting
Practice Questions
Safety Features in Modern Anesthesia Equipment
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
