Anesthetic Equipment and Monitoring — MCQs

On this page
The waveform shown in the image represents which of the following physiological parameters?
In the image shown, identify the function of the marked structure on the endotracheal tube.
Which is the best confirmatory method to ensure the central line is in the jugular vein?
Resistance of the tube shown below is primarily because of
Which of the following is a dimension of the medical device shown?
The given carbon dioxide absorber canister is showing absorbent exhaustion. Which indicator dye is responsible for this color change?

For the following recording and display, which wavelength of light is used?
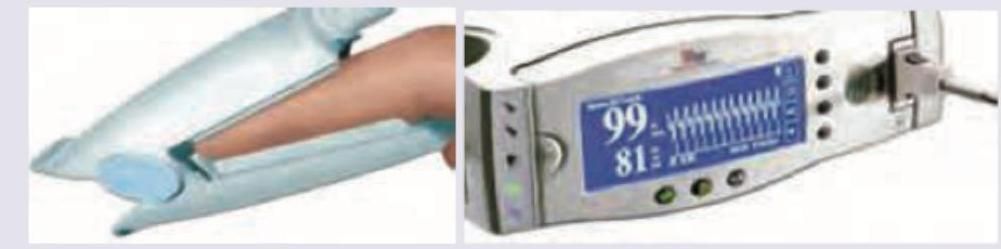
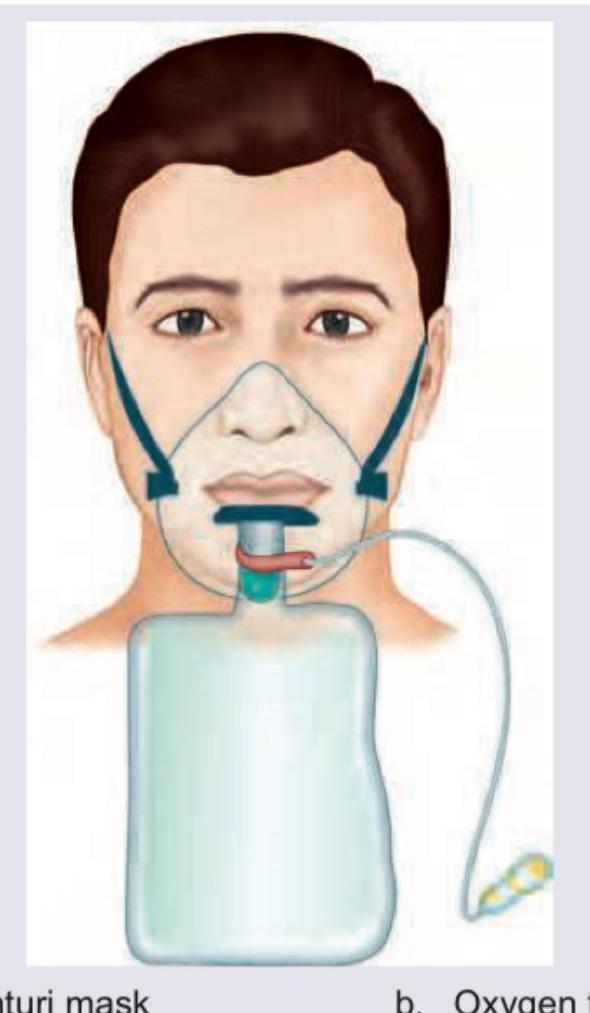
The following image shows:
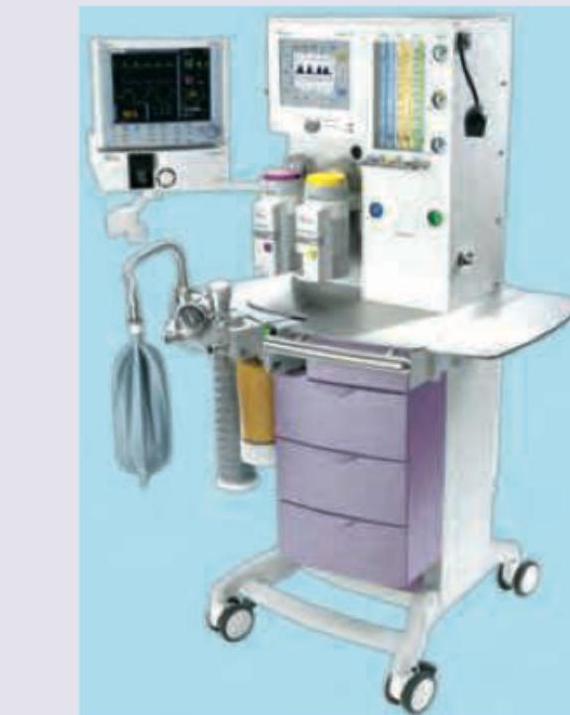
The machine shown below is used for \qquad :
The following cannula is \qquad guage:

Practice by Chapter
Anesthesia Machine Components
Practice Questions
Breathing Systems
Practice Questions
Vaporizers
Practice Questions
Gas Cylinders and Pipeline Supply
Practice Questions
Anesthesia Ventilators
Practice Questions
Standard Monitoring: ECG, BP, Pulse Oximetry
Practice Questions
Capnography
Practice Questions
Neuromuscular Monitoring
Practice Questions
Temperature Monitoring
Practice Questions
Invasive Hemodynamic Monitoring
Practice Questions
Equipment Troubleshooting
Practice Questions
Safety Features in Modern Anesthesia Equipment
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
