Anesthetic Equipment and Monitoring — MCQs

On this page
Sugammadex is used for what purpose?
What is the clinically relevant dose of neuromuscular blocker required for clinically useful relaxation?
The provided capnography (ETCO2) curve depicts which of the following conditions?
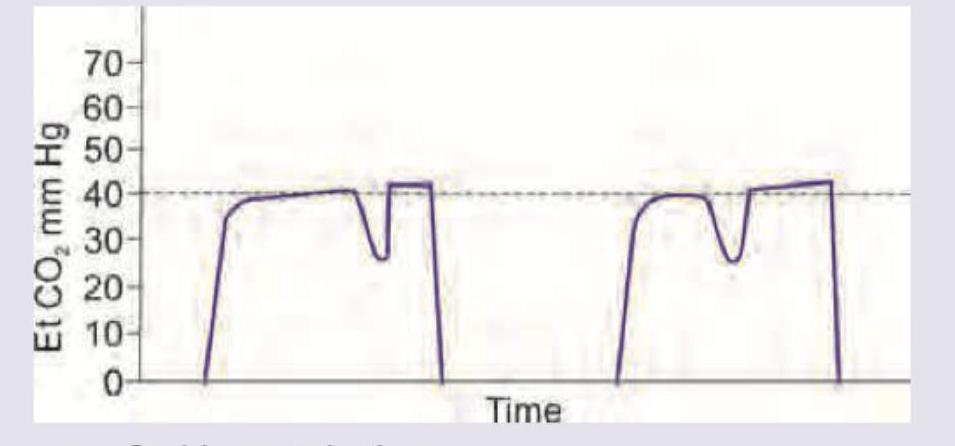
Nasal intubation is contraindicated in which of the following conditions?
What is the most sensitive method for non-invasive monitoring of cardiovascular ischemia in the perioperative period?
Which of the following anesthetic agents has the least diffusion coefficient?
Central venous pressure (CVP) and pulmonary wedge pressure provide an accurate assessment of all of the following EXCEPT?
What is the color of a 22 gauge IV cannula?
What is true about Nitrous Oxide (N2O)?
All of the following are safety measures to prevent the delivery of a hypoxic gas mixture to the patient, except –
Practice by Chapter
Anesthesia Machine Components
Practice Questions
Breathing Systems
Practice Questions
Vaporizers
Practice Questions
Gas Cylinders and Pipeline Supply
Practice Questions
Anesthesia Ventilators
Practice Questions
Standard Monitoring: ECG, BP, Pulse Oximetry
Practice Questions
Capnography
Practice Questions
Neuromuscular Monitoring
Practice Questions
Temperature Monitoring
Practice Questions
Invasive Hemodynamic Monitoring
Practice Questions
Equipment Troubleshooting
Practice Questions
Safety Features in Modern Anesthesia Equipment
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
