Anesthetic Equipment and Monitoring — MCQs

On this page
What is the recommended patient position for orotracheal intubation?
Barium hydroxide lime is not used as a carbon dioxide absorbent in a circle system because:
Which of the following anesthetic agents is not compatible with soda lime?
Which nerve is most commonly used for neuromuscular monitoring under anesthesia?
The material used for a vaporizer should have which of the following qualities?
In clinical anesthesia, which nerve is the most commonly used site for monitoring neuromuscular response during anesthesia and in intensive care units?
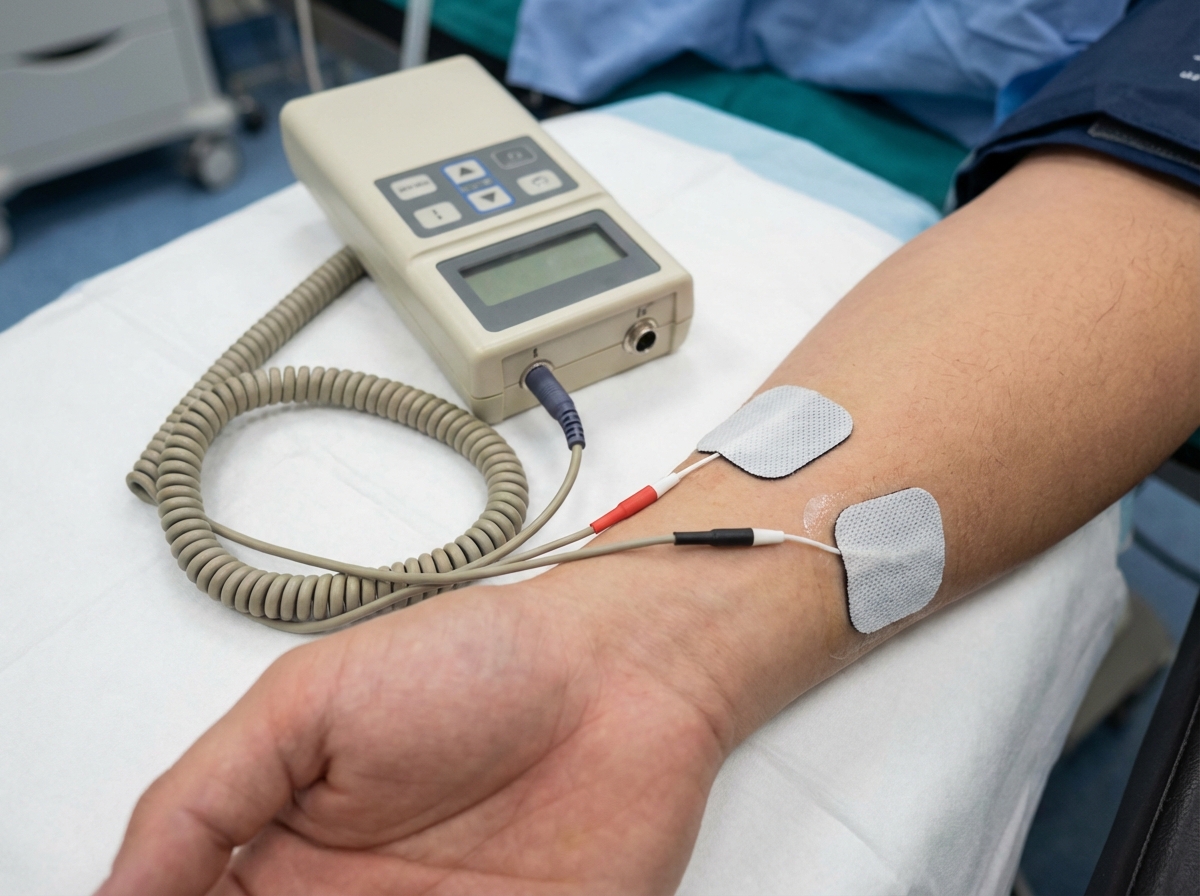
What is the primary use of the depicted device?
What is the name of the test performed before drawing an arterial blood gas sample?
The volatility of an anesthetic agent is directly proportional to lowering the flow in the portal vein. Portal flow is maximally reduced by which agent?
What is Wydase?
Practice by Chapter
Anesthesia Machine Components
Practice Questions
Breathing Systems
Practice Questions
Vaporizers
Practice Questions
Gas Cylinders and Pipeline Supply
Practice Questions
Anesthesia Ventilators
Practice Questions
Standard Monitoring: ECG, BP, Pulse Oximetry
Practice Questions
Capnography
Practice Questions
Neuromuscular Monitoring
Practice Questions
Temperature Monitoring
Practice Questions
Invasive Hemodynamic Monitoring
Practice Questions
Equipment Troubleshooting
Practice Questions
Safety Features in Modern Anesthesia Equipment
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
