Anesthetic Equipment and Monitoring — MCQs

On this page
Which of the following conditions is NOT associated with the shown graph?
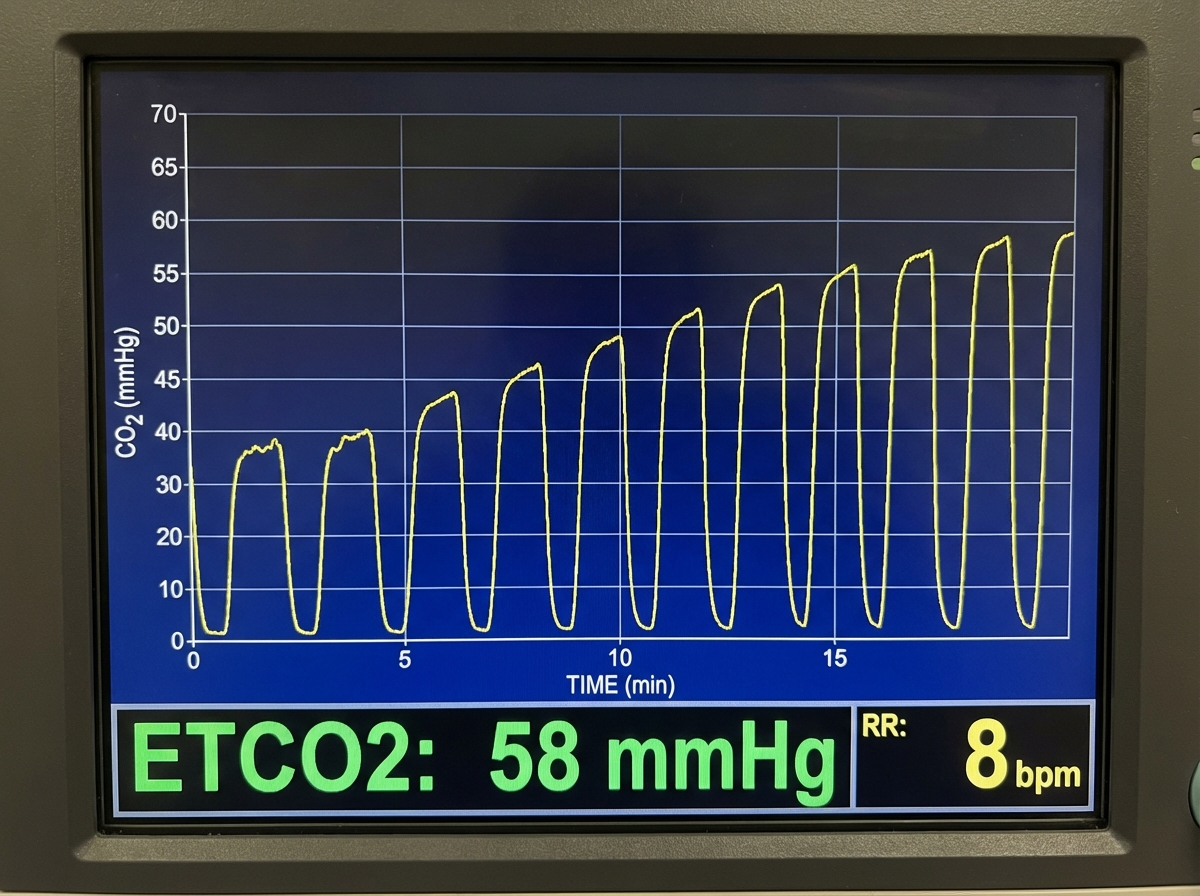
Which of the following tubes is used in surgery for cleft palate repair?
Bains' circuit is which type of Mapleson circuit?
All of the following are used for grading coma in the Glasgow Coma Scale except:
Which of the following statements are true about the Bain circuit?
What is the ratio of O2 to N2O in Entonox?
Which drug is used as an alternative to succinylcholine for intubation?
All of the following are methods of arterial blood pressure monitoring except:
Which condition causes end-tidal CO2 to be increased to its maximum level?
What is the color of a nitrous oxide cylinder?
Practice by Chapter
Anesthesia Machine Components
Practice Questions
Breathing Systems
Practice Questions
Vaporizers
Practice Questions
Gas Cylinders and Pipeline Supply
Practice Questions
Anesthesia Ventilators
Practice Questions
Standard Monitoring: ECG, BP, Pulse Oximetry
Practice Questions
Capnography
Practice Questions
Neuromuscular Monitoring
Practice Questions
Temperature Monitoring
Practice Questions
Invasive Hemodynamic Monitoring
Practice Questions
Equipment Troubleshooting
Practice Questions
Safety Features in Modern Anesthesia Equipment
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
