Upper Limb — MCQs

On this page
A rock climber falls on their shoulder, resulting in a chipping off of the lesser tubercle of the humerus. Which of the following structures would most likely have structural and functional damage?
A patient has a tiny (0.2 cm), but exquisitely painful tumor under the nail of her index finger. Prior to surgery to remove it, local anesthetic block to a branch of which of the following nerves would be most likely to achieve adequate anesthesia?
Which nerve passes through the spiral groove of the humerus?
Injury to which of the following nerves leads to foot drop?
What is the nerve injury that causes a "claw hand" deformity as shown in the image?
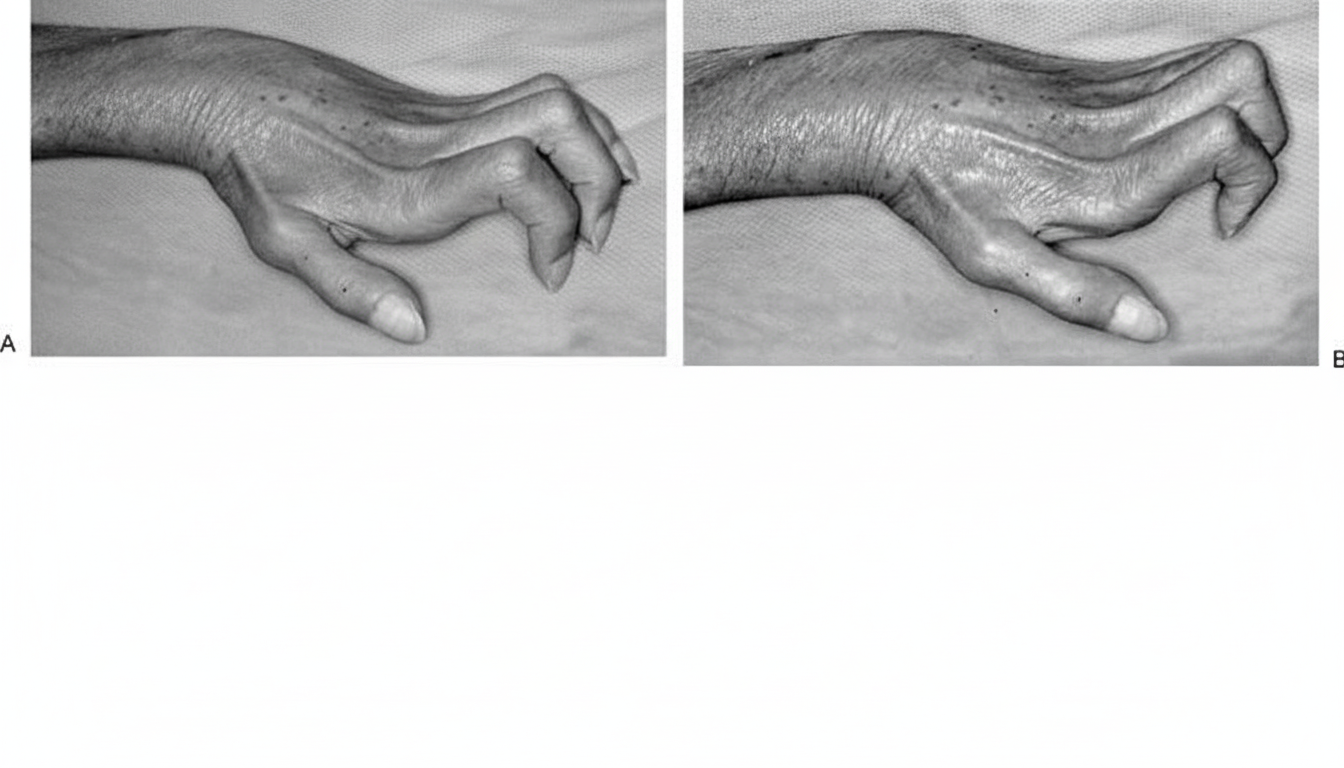
Which of the following arteries does NOT participate in the anastomosis around the scapula?
Which among the following muscles receives dual nerve supply?
Postoperative examination revealed that the medial border and inferior angle of the left scapula became unusually prominent (projected posteriorly) when the arm was carried forward in the sagittal plane, especially if the patient pushed with outstretched arm against heavy resistance (e.g., a wall). What muscle must have been denervated during the axillary dissection?
All of the following statements about the brachial plexus are true EXCEPT:
The image shows a clinical finding in a patient's upper limb. Based on these findings, at which anatomical level has the patient most likely sustained a lesion?
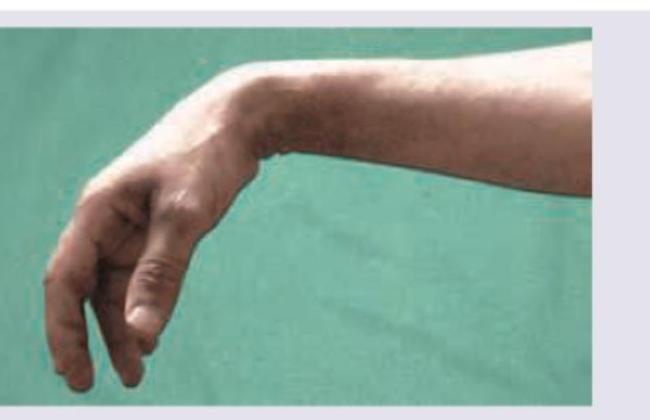
Practice by Chapter
Pectoral Region and Axilla
Practice Questions
Arm and Cubital Fossa
Practice Questions
Forearm and Hand
Practice Questions
Joints of Upper Limb
Practice Questions
Nerves of Upper Limb
Practice Questions
Arterial Supply and Venous Drainage
Practice Questions
Lymphatic Drainage
Practice Questions
Muscles and Their Actions
Practice Questions
Applied Anatomy and Clinical Correlations
Practice Questions
Surface Anatomy and Landmarks
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
