Upper Limb — MCQs

On this page
Palmar interossei are absent in which of the following digits?
Klumpke's palsy is due to injury to which part of the brachial plexus?
Which muscle forms the posterior wall of the axilla?
All are true about carpal bones except?
The test performed below shows involvement of which of the following nerve?
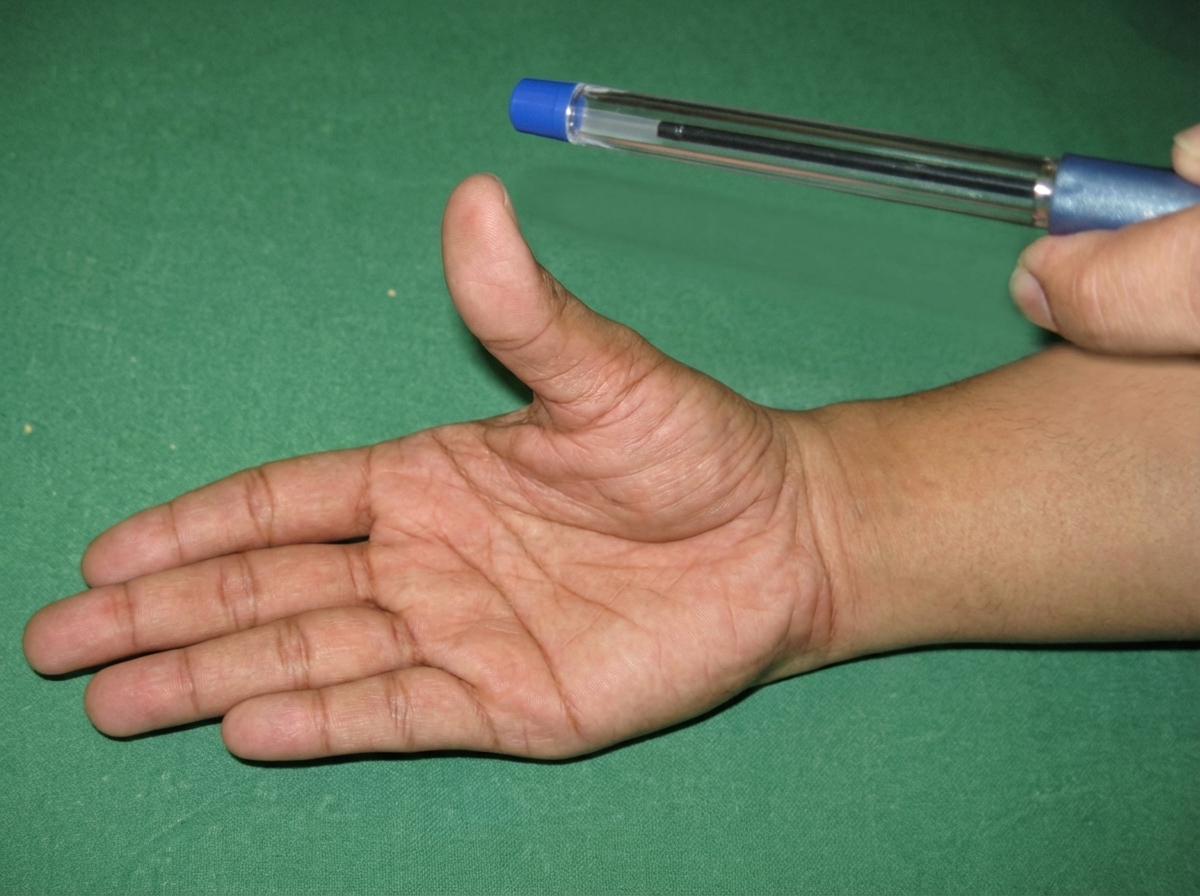
Which of the following muscles has no action at the shoulder joint?
What is the major action of the muscles that cause flexion of the MCP joint and extension of the IP joints?
Claw hand is caused by which of the following conditions?
What is the largest carpal bone?
Upper boundary of quadrangular space is formed by?
Practice by Chapter
Pectoral Region and Axilla
Practice Questions
Arm and Cubital Fossa
Practice Questions
Forearm and Hand
Practice Questions
Joints of Upper Limb
Practice Questions
Nerves of Upper Limb
Practice Questions
Arterial Supply and Venous Drainage
Practice Questions
Lymphatic Drainage
Practice Questions
Muscles and Their Actions
Practice Questions
Applied Anatomy and Clinical Correlations
Practice Questions
Surface Anatomy and Landmarks
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
