Upper Limb — MCQs

On this page
The axis of abduction and adduction of digits passes through the center of which metacarpal bone?
What nerve innervates the short head of the biceps brachii?
The axillary nerve is a branch of which part of the brachial plexus?
All of the following are true statements about the joints of the upper limb EXCEPT:
A 16-year-old boy sustained a severe radial nerve injury due to a midshaft humerus fracture following a motorcycle fall. Which of the following conditions would most likely result from this injury?
Winging of scapula is due to:
The fourth dorsal interosseous muscle is innervated by?
For which of the following nerve palsies is the below test detected?
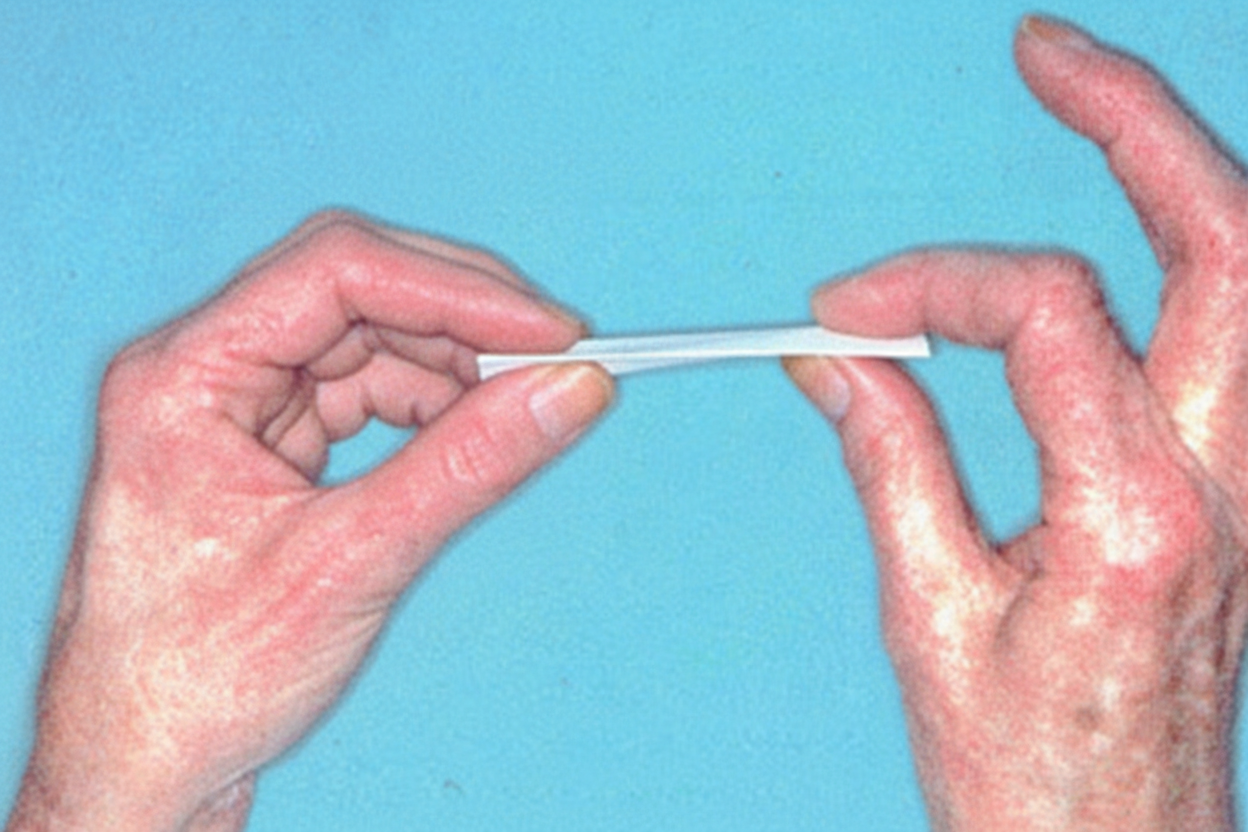
A patient presents with a deep stab wound in the middle of the forearm, resulting in impaired movement of the thumb. Examination suggests a lesion of the anterior interosseous nerve. Which of the following muscles is paralyzed?
Which of the following muscles is spared when the radial nerve is injured in the radial groove?
Practice by Chapter
Pectoral Region and Axilla
Practice Questions
Arm and Cubital Fossa
Practice Questions
Forearm and Hand
Practice Questions
Joints of Upper Limb
Practice Questions
Nerves of Upper Limb
Practice Questions
Arterial Supply and Venous Drainage
Practice Questions
Lymphatic Drainage
Practice Questions
Muscles and Their Actions
Practice Questions
Applied Anatomy and Clinical Correlations
Practice Questions
Surface Anatomy and Landmarks
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
