Upper Limb — MCQs

On this page
Entrapment neuropathy at the arcade of Frohse involves which nerve?
What are the roots involved in Erb's palsy?
A 19-year-old boy sustained a shoulder injury after falling from a motorbike. The doctor diagnosed him with Erb's palsy. Which of the following signs and symptoms would NOT be observed in this condition?
Which is the first ossification center to appear around the elbow joint?
The musculocutaneous nerve pierces which of the following muscles?
Froment's sign is a clinical feature of which condition?
A 52-year-old woman presented with weakness of shoulder movements. Investigations revealed quadrangular space syndrome. Which of the following nerves is likely to be affected?
Fracture of the surgical neck of the humerus leads to loss of abduction movement of the corresponding shoulder joint due to injury of which nerve?
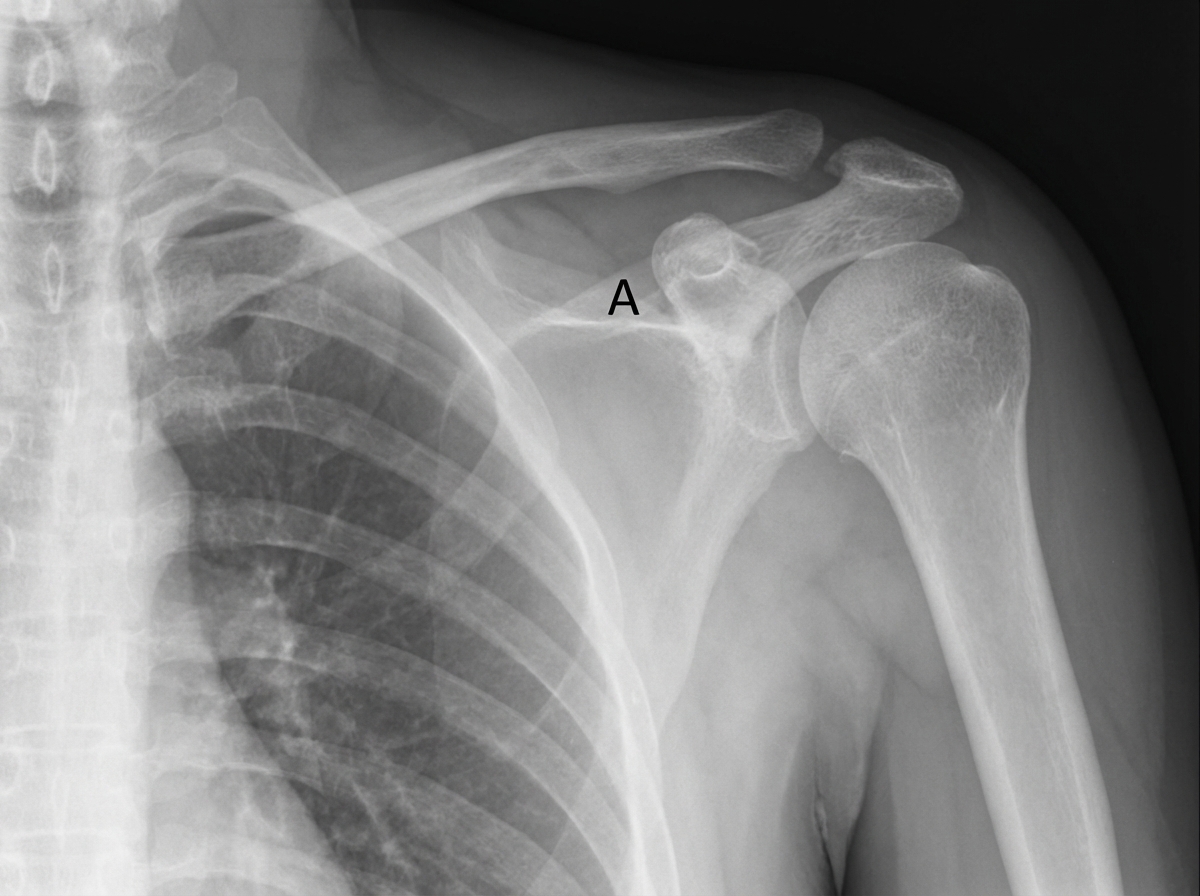
An 11-year-old boy falls down the stairs. A physician examines a radiograph of the boy's shoulder region. If the structure indicated by the letter A is calcified, which of the following muscles is most likely paralyzed?
Froment's sign is seen in which nerve palsy?
Practice by Chapter
Pectoral Region and Axilla
Practice Questions
Arm and Cubital Fossa
Practice Questions
Forearm and Hand
Practice Questions
Joints of Upper Limb
Practice Questions
Nerves of Upper Limb
Practice Questions
Arterial Supply and Venous Drainage
Practice Questions
Lymphatic Drainage
Practice Questions
Muscles and Their Actions
Practice Questions
Applied Anatomy and Clinical Correlations
Practice Questions
Surface Anatomy and Landmarks
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
