Upper Limb — MCQs

On this page
All of the following structures form the border of the quadrangular space, EXCEPT?
The head of the scapula articulates with which part of the humerus?
Which is the weakest portion of the shoulder joint capsule?
At what age are the four carpal bones present?
The wrist joint is formed by the articulation of which structures?
Which of the following statements about long flexor tendons is FALSE?
Which nerve arises from a root of the brachial plexus?
The neurovascular bundle in the axilla is surrounded by a sheath derived from which structure?
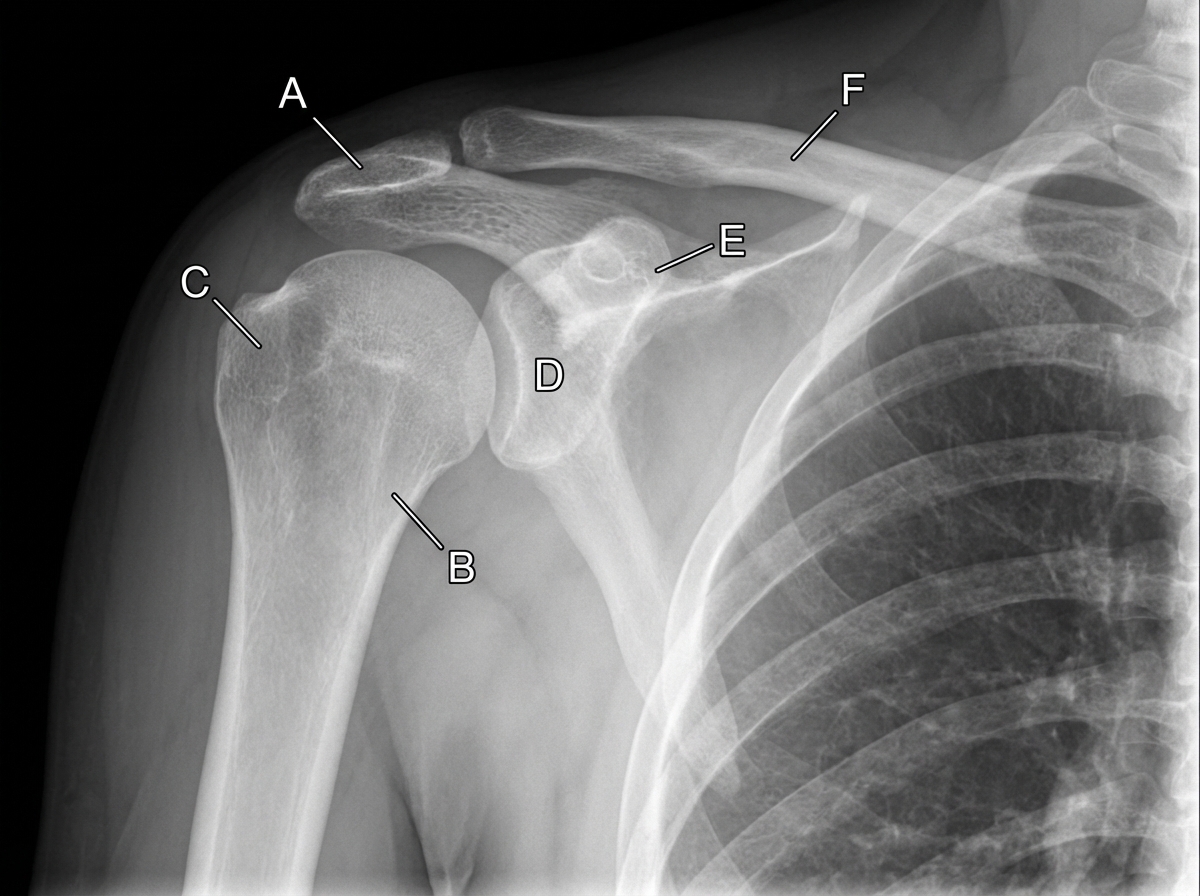
An 11-year-old boy falls down the stairs. A physician examines a radiograph of the boy's shoulder region. If the structure indicated by the letter B is fractured, which of the following structures is most likely injured?
The forcible separation of the head of the radius from the capitulum of the humerus is mainly prevented by which structure?
Practice by Chapter
Pectoral Region and Axilla
Practice Questions
Arm and Cubital Fossa
Practice Questions
Forearm and Hand
Practice Questions
Joints of Upper Limb
Practice Questions
Nerves of Upper Limb
Practice Questions
Arterial Supply and Venous Drainage
Practice Questions
Lymphatic Drainage
Practice Questions
Muscles and Their Actions
Practice Questions
Applied Anatomy and Clinical Correlations
Practice Questions
Surface Anatomy and Landmarks
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
